Can you have “normal” blood levels and still be deficient—like finding your shoes on the rack but noticing the laces never quite reach? It sounds impossible, but biology has a way of turning certainty into a soft riddle. Standard lab results often look tidy. Meanwhile, your cells may be running a little short on the resources they need to perform at full volume. This is where “functional” deficiency enters the conversation: not a simple lab-score problem, but a real-world performance problem.
“Normal” on paper vs. “normal” in your biology
Most routine blood tests are designed to answer a straightforward question: Is the concentration above or below a reference interval? That interval is statistically derived, which can be useful—and also a little blunt. Your physiology, however, operates with more nuance than a number.
A result can fall within the reference range and still be functionally inadequate because the body’s requirements vary. Age, sex, genetics, medication use, diet, inflammation, sleep quality, and even stress physiology can shift how much of a nutrient—or how much of a protective mechanism—your system truly needs.
Think of it like measuring Wi‑Fi signal strength. The meter might read “acceptable,” yet your streaming keeps buffering. The network is technically “online,” but it’s not delivering at the level your life demands.
Functional deficiency: the difference between quantity and capability
Functional deficiency occurs when the body lacks the effective capacity to carry out certain processes, even if bulk markers appear “normal.” In other words, your system may have enough of a substance in circulation, but not enough usable activity at the cellular level.
This can happen due to poor conversion, impaired transport, increased turnover, or suboptimal utilization. Sometimes the lab value measures the wrong “unit of meaning.” For instance, a nutrient might be present, but the enzymes that depend on it may not be operating efficiently.
In functional terms, deficiency can manifest as fatigue, reduced exercise tolerance, cognitive fog, unusual susceptibility to stressors, or persistent symptoms that don’t correlate neatly with standard markers. It’s not “nothing is wrong.” It’s “the wrong question may have been asked.”
Why reference ranges can be misleadingly comforting
Reference ranges are typically broad, aiming to capture the majority of healthy individuals. But “majority” is not the same as “optimal.” Some people sit comfortably near the lower end, and their bodies remain stable. Others hover in the middle and begin to show early warning signs—especially under physiologic pressure.
Reference intervals also don’t always account for context: pregnancy, athletic training loads, chronic inflammation, or genetic variants that alter how your metabolism behaves. The same numerical value might be adequate for one person and insufficient for another.
There’s also the timing issue. Blood draws are snapshots. Nutrient status can fluctuate across the day, after meals, with seasonal variation, and in response to acute illness. A single measurement can miss a trend.
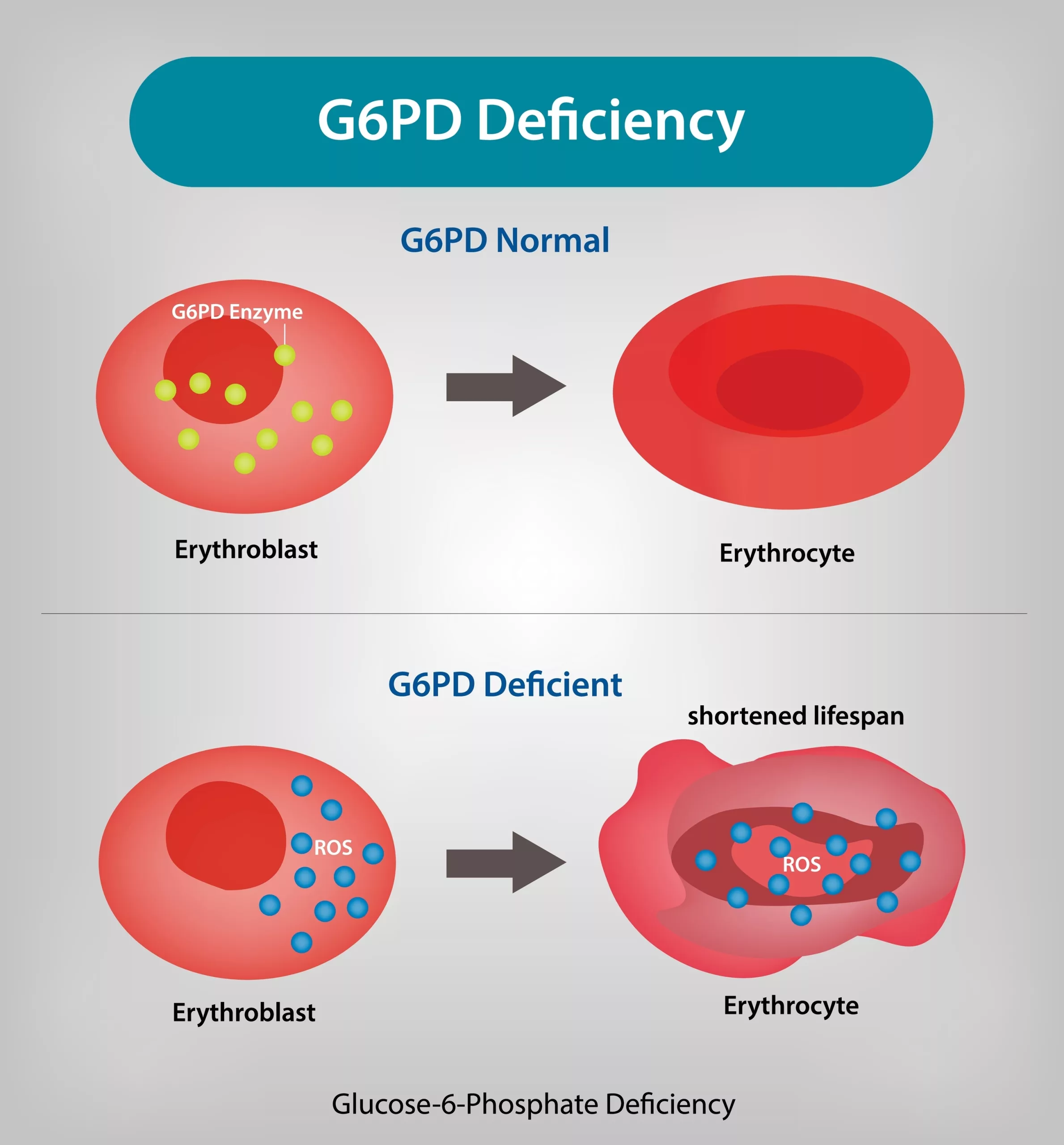
G6PD as an example of “function first” physiology
Some deficiencies reveal themselves not through low levels of a substance, but through vulnerability of a pathway. G6PD (glucose-6-phosphate dehydrogenase) is a classic illustration of how function matters. When G6PD activity is reduced, red blood cells can become more fragile under certain triggers, even if you’re not constantly seeing obvious abnormality in a routine blood panel.
What’s tricky is that symptoms—or lab changes—may only appear when you’re exposed to specific stressors. That means a person can appear “fine” most of the time, yet still have underlying susceptibility.
Common triggers can include certain medications, infections, or oxidative stressors. The practical lesson is simple but powerful: “normal” results don’t always equal “normal resilience.”

Functional testing: asking smarter questions
Functional evaluation tries to measure what actually matters for performance—how well systems operate. Instead of focusing only on concentration, it looks at activity, patterns, and downstream effects. This might include targeted enzymatic measures, specialized blood assessments, or markers that reflect how the body is handling stress and repair.
Some approaches examine how nutrients interact with pathways. Others look for evidence of increased demand. For example, if oxidative load is high, your body may “spend” certain protective resources faster than they can be replaced. That can create a functional shortage despite seemingly acceptable baseline numbers.
In clinical practice, the most revealing tests are often those that correlate with your symptoms and life context. The same result might be interpreted differently for a desk worker versus a competitive endurance athlete, or for someone under chronic infection pressure versus someone in stable remission.
Signs you might be “normal but deficient”
Functional deficiency rarely wears a name tag. Instead, it often shows up as a pattern:
• Symptoms that persist despite “acceptable” labs. The lab looks boring, but your body feels loud.
• Tolerance changes. You get tired sooner, recover slower, or feel mentally sluggish under stress.
• Triggered episodes. Certain exposures—illness, new medication, intense training—lead to disproportionate effects.
• Subtle biochemical clues. Even when totals are “normal,” accompanying indices may hint at inefficiency, heightened turnover, or compensatory mechanisms.
Sometimes, the most informative clue is what improves: dietary adjustments, targeted supplementation, better sleep, or reducing oxidative stress. If function improves while the “normal” marker stays similar, it suggests the deficiency was functional rather than purely numerical.
The role of diet, absorption, and bioavailability
Even a nutritionally adequate diet can fail to deliver functional availability. Absorption problems, medication interactions, gut dysbiosis, and inflammatory states can reduce how much actually becomes usable inside cells. Bioavailability is the key word here—quantity is only the opening act.
Some nutrients require specific transport mechanisms or cofactors to do their jobs. If those supporting systems are strained, the nutrient might exist in the bloodstream but not reach effective concentrations at the cellular level.
In practical terms: a person may eat well but still be deficient functionally if absorption is compromised, or if metabolic demand is unusually high.
Medication and oxidative stress: the stealth disruptors
Certain medications can alter nutrient status, enzyme activity, or redox balance. In some scenarios, oxidative stress can “burn through” protective systems faster than the body can replenish them.
This is why timing and history matter. A normal blood result prior to starting a medication doesn’t guarantee normal function after several weeks. Likewise, a healthy period can hide vulnerability that appears only during infection.
Your body is not a static warehouse. It’s a dynamic factory with shifting workloads. When demand rises or production efficiency drops, functional deficiency becomes more visible.
Working with clinicians: turning mystery into clarity
If you suspect you’re “normal on paper but deficient in practice,” a thoughtful next step is to discuss your symptoms, exposures, and goals with a qualified clinician. Request an approach that includes both conventional and functional perspectives—because the goal is not to chase abnormality for its own sake. The goal is to align measurements with real outcomes.
Ask questions like: Which pathways might be impaired? Are there signs of increased demand or poor utilization? Would targeted functional testing clarify the issue? Sometimes a broader panel or an activity-based assessment reveals what a single number concealed.
Remember: the most useful lab is the one that explains your lived experience.
When to seek urgent attention
If symptoms involve severe anemia signs, fainting, yellowing of the skin, dark urine, shortness of breath, or sudden worsening after a trigger, urgent evaluation is warranted. Functional vulnerabilities can occasionally escalate quickly.
Even when the story seems “lab-normal,” your safety comes first. If your body is raising a red flag, treat it like a high-priority signal, not a mere inconvenience.
The takeaway: normal ranges aren’t the whole narrative
So, can you have a normal blood level but still be deficient? Yes—especially when the deficiency is functional. The number might land in range, while the underlying capacity to operate smoothly does not. Your biology is not a spreadsheet; it’s an orchestra. Sometimes the sheet music looks fine, but the performance falters because an instrument’s tuning is off.
If you’re experiencing persistent symptoms, triggered reactions, or reduced resilience, consider that your “normal” lab may be incomplete information. The next chapter may require functional testing, context-aware interpretation, and a plan that respects how your body actually works.