Winter has a way of rearranging the body’s priorities. Sunlight dwindles, routines compress, and even the most energetic mornings can feel dimmer. In that hush, vitamin D often becomes a silent variable—one that many people suspect, few people quantify, and almost everyone underestimates. The intriguing twist is that “taking vitamin D” isn’t a one-size ritual. It’s more like tuning an instrument: the right dose, at the right time, guided by how your body is already behaving.
Reframing Winter as a Sunlight Equation
Most conversations about vitamin D start with the supplement bottle. But a more useful perspective begins earlier—with the physics of seasons. Vitamin D is synthesized in the skin when ultraviolet (UV) light is available. When winter arrives, the UV angle changes and the opportunity for natural production shrinks dramatically. Even if you still walk outside, clouds, window glass, clothing coverage, and latitude can make the difference between “some exposure” and “enough exposure.”
So the question becomes not “Should I take vitamin D?” but “What gap is winter creating for me?” That shift in thinking is curious on purpose. It encourages you to treat dosage as responsive rather than reflexive. Short days can mean your body’s baseline changes—slowly, quietly, and sometimes without obvious symptoms until later.
Dosage Adjustments: The Real Art Is Individualization
Dosage adjustments aren’t merely about choosing a number. They’re about aligning intake with your body’s current status, your risk factors, and your tolerance. People often assume vitamin D functions like a simple fuel. In reality, it behaves more like a regulator—affecting calcium absorption, musculoskeletal maintenance, immune signaling, and possibly mood-related pathways through downstream biology.
When you adjust your dose in winter, consider that requirements can shift across the same person year-to-year. One winter might call for a modest maintenance approach; another might reveal persistently low levels on lab testing. Seasonal strategy also matters: starting earlier can prevent a slow slide, while waiting until late winter can mean you spend months playing catch-up.
Common Winter Starting Points (and Why Caution Still Matters)
Many adults take vitamin D3 in winter because it’s often well tolerated and commonly used for supplementation. Yet “common starting points” should feel like scaffolding, not architecture. Some people begin with a moderate daily dose; others prefer weekly or higher intermittent dosing strategies. The choice should reflect your consistency habits—because consistency often beats intensity.
Here’s the key curiosity: the best dose is rarely the highest one you can buy. Bigger doses can increase the chance of side effects, especially over time. While vitamin D is fat-soluble—meaning it can accumulate—the body generally uses it in a regulated manner. That’s exactly why overshooting can become a problem if it’s prolonged without monitoring.

Who Typically Needs a Larger Dose Response?
Winter reduces vitamin D synthesis for many people, but not everyone is affected equally. Risk factors can shift your needs upward. Darker skin pigmentation can reduce UV-induced production. Older age can also lower the efficiency of vitamin D metabolism. People with limited sun exposure—due to indoor work, mobility limitations, or cultural clothing practices—often face a bigger seasonal drop.
Body composition matters too. Vitamin D is stored in fat tissue, and individuals with higher body fat may require different dosing to reach the same blood levels. Additionally, conditions affecting absorption—such as certain gastrointestinal disorders—or medications that interfere with vitamin D metabolism can change the equation.
There’s also an often-overlooked category: people who feel “off” during winter. Fatigue, low motivation, and reduced physical endurance may have multiple causes. Yet vitamin D insufficiency can be part of the story, not the entire story. Thinking in layers is wiser than seeking a single culprit.
How to Think About Blood Levels: Testing as a Compass
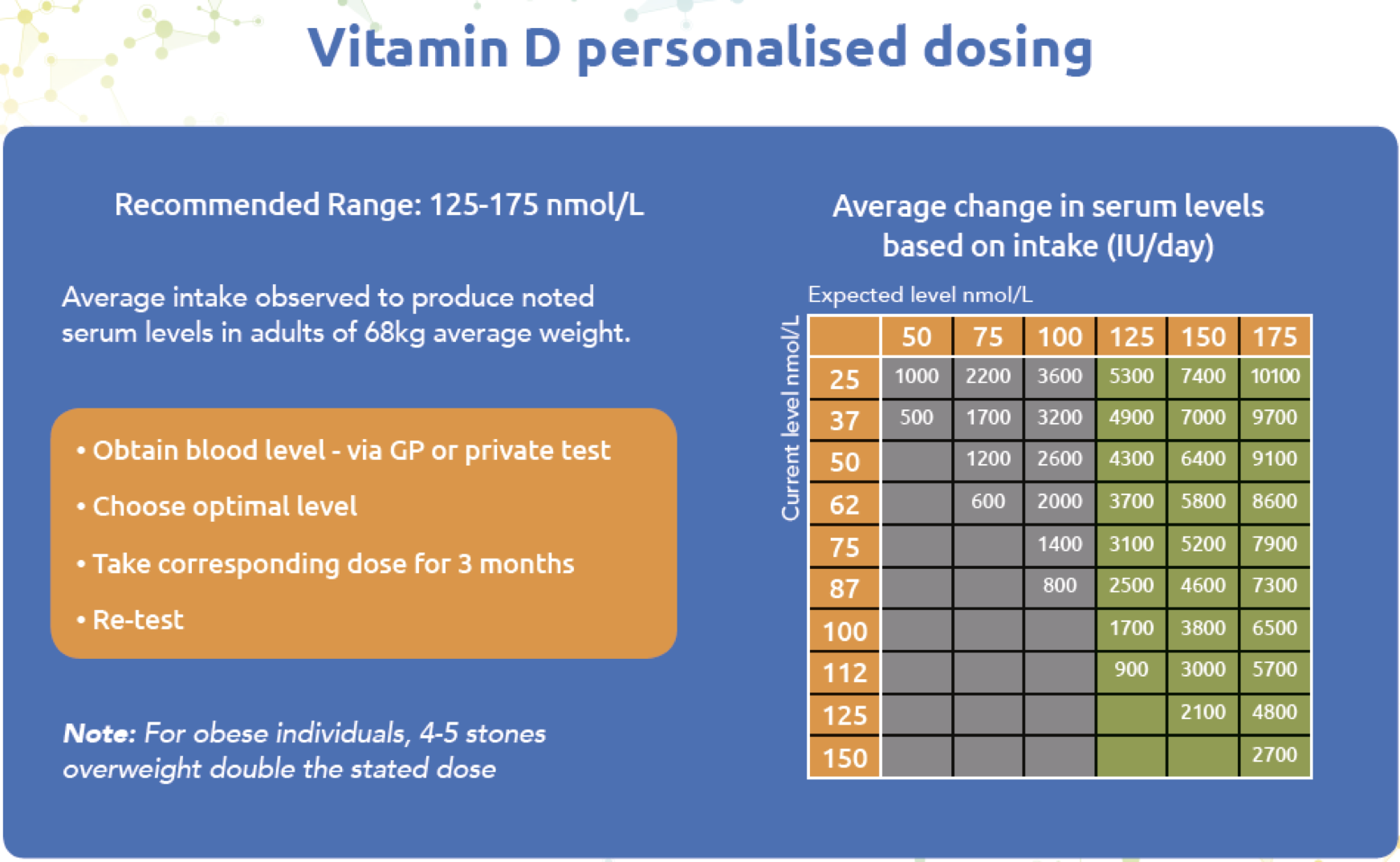
If you want a dosage adjustment that feels less like guesswork, testing provides a compass. A common approach is to measure 25-hydroxyvitamin D, the circulating marker that reflects vitamin D status. Then intake can be adjusted with intention: raise if low, maintain if borderline, and avoid excess if already robust.
Timing the test can also influence interpretation. Testing right at the start of winter may show your pre-season baseline, while testing later might reveal how your body responded to supplementation. Neither approach is “wrong.” Each answers a different question.
Still, lab interpretation isn’t always a straight line. Personal physiology, concurrent nutrients (especially calcium and magnesium), and general health can change how vitamin D translates into outcomes. A test is not a prophecy; it’s a datapoint.
Daily vs Weekly: Choose a Rhythm You Can Sustain
Dosage adjustments often come in two popular rhythms: daily micro-doses or weekly lump-sum dosing. Daily intake may offer steadier blood levels and can be easier for those who prefer habit-based routines. Weekly dosing can simplify scheduling and may reduce the friction of forgetting.
But the subtle decision is behavioral. The best plan is the one that survives real life—busy weeks, travel, and the mild chaos of winter schedules. If you consistently miss doses, a higher intermittent plan won’t rescue the situation. It may simply create uneven intake.
When adjusting your dosing frequency, consider how your body responds over time and how you feel. Even if symptoms are nonspecific, patterns can emerge: improved stamina, better recovery after workouts, or a more stable mood. These are not guaranteed, but they are plausible, especially when deficiency is present.
Pairing Supplements With Nutrition: Calcium, Magnesium, and More
Vitamin D doesn’t work in isolation. Its primary role includes helping the body absorb calcium. If calcium intake is inadequate, the benefits of vitamin D may not fully materialize. Dietary calcium can come from dairy products, fortified alternatives, leafy greens, and certain calcium-set tofu varieties.
Magnesium also plays a supporting role in vitamin D metabolism. Without enough magnesium, downstream processes can become less efficient. Some people focus narrowly on vitamin D and overlook magnesium-rich foods such as nuts, seeds, legumes, and whole grains.
This is where the promise of a shift in perspective becomes real: supplementation is not a standalone event. It’s a choreography with meals, hydration, and overall nutrient adequacy.
Safety and Upper Limits: The Line You Don’t Want to Cross
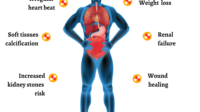
Winter dosing should come with respect for boundaries. Because vitamin D is fat-soluble, excess can accumulate. Prolonged high intake may lead to elevated calcium levels, which can strain kidneys and cause uncomfortable symptoms such as nausea, constipation, confusion, or excessive thirst and urination.
Safety isn’t about fear; it’s about precision. The most prudent strategy is to choose an appropriate dose, reassess after a reasonable interval, and avoid stacking multiple products that unknowingly overlap. Many multivitamins contain vitamin D. Some “immune support” formulas also add it. A quick label scan can prevent accidental overconsumption.
Signs Your Winter Plan Might Need Revision
Sometimes the body gives hints. If fatigue persists despite consistent supplementation, the issue may be vitamin D insufficiency—or it may be something else entirely, such as sleep disruption, thyroid changes, iron deficiency, or stress-related physiology. If you experience symptoms that could suggest too much calcium or too high vitamin D intake, that’s a clear signal to pause and reassess.
Revision is not failure. It’s refinement. A dosage adjustment should feel iterative, like recalibrating a compass after changing terrains. You’re not chasing perfection; you’re building a reliable seasonal strategy.
Putting It Together: A Winter Supplement Strategy That Feels Intelligent
A thoughtful winter vitamin D plan often looks like this: start with awareness (how winter reduces sunlight), choose a dosing rhythm you can actually maintain, account for risk factors, and consider testing to guide refinement. Then support the process with nutrition—calcium and magnesium included—and keep safety in view by avoiding excess from overlapping supplements.
Winter can make everything feel slower. But your approach doesn’t have to be. With a curious, data-informed, individualized lens, dosage adjustments become less about guessing and more about aligning. The result is not just a supplement routine, but a seasonal practice that respects your biology—and that quietly changes how winter feels.