Can you really build up high vitamin D levels when your calendar refuses to cooperate with the sun? It sounds like a mischievous riddle—one part sunshine, one part skepticism. Yet the human body is surprisingly pragmatic. Vitamin D production begins with sunlight, but it’s not the only pathway. If you’re living in a cloud-heavy city, working indoors, or simply allergic to the idea of spending hours outside, you may still have options that feel like clever workarounds rather than lost causes.
Vitamin D: Why Sunlight Matters (and Why It’s Not the Only Door)
Vitamin D is often called the “sunshine vitamin” because ultraviolet B (UVB) light helps your skin manufacture it. When UVB photons hit your skin, a chemical cascade begins, ultimately producing vitamin D in a form that your body can use after further processing by the liver and kidneys. The twist is that UVB availability varies wildly—by latitude, season, time of day, cloud cover, and even air pollution.
So, if your sun exposure is low, your body may struggle to keep production high. But “low sun” doesn’t automatically mean “low vitamin D.” Your overall vitamin D status is shaped by multiple inputs: diet, supplements, body composition, genetics, and how your routine interacts with your environment. In other words, vitamin D is a team sport, not a solo performance by the sun.
The Hidden Challenge: Your Routine vs. UVB Reality
Here’s where the playful question turns into a practical challenge. Many people assume that “some daylight” equals “enough UVB.” But daylight can be bright without being UVB-rich. Winter sunlight, for instance, may be visually ample yet chemically stingy. Window glass also blocks much UVB radiation, meaning that indoor sitting near a bright window is not the same as outdoor exposure.
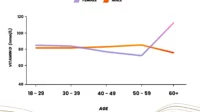
Skin tone, age, and clothing coverage can further alter UVB absorption. A higher melanin content generally reduces vitamin D synthesis, and as people age, the skin’s ability to convert precursors can decline. Add long workdays, sunscreen habits, and time spent behind screens, and the sun becomes less of a reliable supplier.
How Low Sun Exposure Affects Your Numbers
When UVB stimulation is minimal, vitamin D levels can drift downward over time. The body does store vitamin D in fat tissue, which can buffer you for a while. But that buffer isn’t infinite. Think of it like a pantry: it helps during short shortages, yet sustained scarcity eventually makes itself known.
Low vitamin D may not always announce itself dramatically. Instead, it can manifest as subtle fatigue, muscle aches, or a general sense of “something feels off.” Over time, inadequate vitamin D can contribute to reduced calcium absorption, which matters for bone health. The skeletal system tends to be patient—until it isn’t.
Can You Still Reach High Vitamin D Levels? Yes, Through Alternative Routes
The crucial question is not whether sunlight is important—it is. The crucial question is whether you can supplement the sunlight gap. In practice, higher vitamin D levels can be achieved through:
Dietary sources (especially fatty fish, egg yolks, and fortified foods).
Supplementation (vitamin D3 is often favored for raising blood levels).
Medical guidance when deficiency is suspected or confirmed.
Diet can help, but it’s often difficult to consistently achieve robust vitamin D intake from food alone—unless you’re eating fortified products regularly or you include vitamin D-rich foods as part of your routine. That’s why supplements frequently become the “bridge” for people with low sun exposure.
Food as a Vitamin D Compass: What Actually Helps
If your sun exposure is low, you may want to treat food like a compass—small but consistent. Fatty fish (salmon, sardines, mackerel) can provide meaningful vitamin D. Egg yolks contain a bit, and some mushrooms can contribute vitamin D when exposed to UV light during cultivation. Fortified dairy alternatives, fortified milk, and fortified cereals can also make your intake more predictable.
Still, many everyday eating patterns don’t supply enough vitamin D to reach “high” status for everyone. The gap between what’s on the label and what’s needed by the body can be wide. This is where personalization becomes essential.

Supplements: The Most Direct Strategy (But Not a Free-for-All)
Supplements can raise vitamin D levels even when sun exposure is limited. Many people choose vitamin D3 because it tends to be effective at improving blood concentrations. Dosage, however, is not one-size-fits-all. Your baseline vitamin D level, body weight, dietary intake, and overall health all influence how much you need.
A cautious approach is wise. Too little can fail to correct the deficiency; too much over time can be problematic. Excess vitamin D can increase calcium levels, which may lead to symptoms such as nausea, weakness, and kidney-related concerns. The key is to use supplementation intentionally—ideally guided by a clinician and supported by lab testing.
Testing and Interpreting Results: Beyond “Low” and “Normal”
If you’re wondering whether you can have high vitamin D levels with low sun exposure, the most reliable answer comes from a blood test. Commonly measured as 25-hydroxyvitamin D, this marker reflects vitamin D status more accurately than testing active forms.
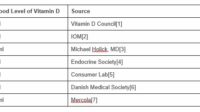
Interpretation depends on the laboratory’s reference range and your personal context. Some people aim for higher targets under medical supervision, especially when deficiency is confirmed. Others focus on sufficiency. Either way, testing helps turn guesswork into precision, and precision is often the difference between “hope” and “success.”
Why Some People “Beat the Sun” Better Than Others
Your body may handle vitamin D differently than someone else’s body. Factors like genetics, gut health, and absorption efficiency can influence outcomes. Certain medications can also affect vitamin D metabolism. Body composition matters too, because vitamin D is fat-soluble; in some individuals, vitamin D can be sequestered in adipose tissue, altering how much is available in circulation.
This is why the phrase “high vitamin D” is less about a trophy number and more about your functional status. A person can have a certain lab value and still feel poorly, while another feels great at a different number. Context is the plotline.
Practical Lifestyle Hacks for Low-Sun Living
You may not control the sky, but you can optimize your habits. Consider:
Consistency: regular fortified foods or supplements can be more effective than sporadic spikes.
Timing: when taking supplements, choose a routine you’ll actually follow. Some people find taking vitamin D with meals that include fat improves absorption.
Mindful sunscreen strategy: if you’re always covered or always indoors, supplementation becomes more important. If you use sunscreen outdoors, recognize that it can reduce vitamin D synthesis—though it’s still essential for skin cancer risk management.
Outdoor breaks: even brief outdoor exposure can contribute, especially during months with stronger UVB.
These tweaks are not dramatic. They are steady. And steady often wins.
The Bottom Line: High Vitamin D Without Much Sun Is Possible
So, can you have high vitamin D levels with low sun exposure? Yes—but it usually requires structure rather than wishful thinking. Sunlight is a major lever, yet food and supplements can compensate, sometimes quite effectively. The best route is individualized: test your levels, understand your intake, and choose a plan that is both safe and sustainable.
In the end, the riddle resolves into a strategy. Even if the sun rarely visits your schedule, vitamin D can still be coaxed into becoming abundant—one informed decision at a time.