Vitamin D is one of those quiet nutritional workhorses—small in dose, significant in consequence. For many breastfeeding families, the plan is simple: ensure an infant receives vitamin D for healthy bones, muscle function, and immune regulation. Yet the “usual” method—drops—doesn’t always fit real life. Maybe your baby gags at the taste, you’re frequently away from home, or you simply prefer a gentler approach. This guide focuses on how to support vitamin D intake for infants without drops, using breastfeeding mom’s dose strategies and other practical alternatives that can fit a variety of routines.
Understanding the Goal: Vitamin D Status in Breastfed Infants
Breast milk is a remarkable food, but it doesn’t automatically supply high levels of vitamin D, especially in regions with limited sunlight. Vitamin D is fat-soluble, and its presence in breast milk depends largely on the mother’s vitamin D status. That’s why “mother-first” approaches can work: when the breastfeeding parent has adequate vitamin D, the nutrient can be transferred to the infant through milk.
Consider the physiology like a relay race. Sunlight exposure, dietary intake, and supplementation influence the parent’s blood vitamin D level. Then vitamin D moves into milk and becomes available to the baby. The infant benefits, but the timing and consistency matter. Short bursts of sun or sporadic supplementation often create uneven results. Consistent, measurable dosing is typically the key to a reliable plan.

Breastfeeding Mom’s Dose: How Indirect Supplementation Can Work
Giving vitamin D “without drops” often means increasing the breastfeeding parent’s vitamin D intake so that breast milk becomes the delivery vehicle. This approach can be especially helpful for infants who refuse or struggle with direct oral drops.
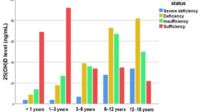
In practice, the breastfeeding parent supplements vitamin D at a dose determined with a clinician, typically guided by current medical guidance and the mother’s baseline vitamin D level (sometimes assessed with a blood test for 25-hydroxyvitamin D). The goal is to raise the mother’s stores enough to supply the infant consistently.
Why does this strategy require care? Because the relationship between maternal dose and infant vitamin D status isn’t perfectly identical for every body. Factors like body mass, skin pigmentation, latitude, season, and milk volume can influence transfer. A clinician can help tailor the dose and timing to reduce the risk of overshooting.
Safety First: Upper Limits, Monitoring, and When to Be Cautious
Vitamin D is powerful—powerful enough that “more” isn’t always “better.” While deficiency is common, excessive vitamin D can cause hypercalcemia (high calcium levels), which can be harmful. Therefore, the safety plan should be more than a guess; it should be a protocol.
Key safety considerations include existing medical conditions (such as kidney issues), use of certain medications (including some anticonvulsants or steroids), and a history of high calcium or vitamin D levels. If the breastfeeding parent is already taking a prenatal vitamin or high-dose supplement, stacking additional vitamin D can unintentionally create a surplus.
If your family wants maximum assurance, ask about monitoring. A blood test can clarify whether the chosen maternal dose achieves the desired vitamin D status without drifting into excess. Even without testing, follow clinician recommendations closely and avoid improvising with high-dose regimens.
Choosing the Right Supplement Form for the Breastfeeding Parent
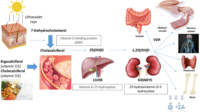
When replacing infant drops with a maternal-dosing strategy, the supplement selection matters. Many vitamin D products use either D3 (cholecalciferol) or D2 (ergocalciferol). In most supplementation contexts, D3 is commonly favored for its effectiveness at raising and maintaining vitamin D levels.
Also consider the absorption pathway. Vitamin D is fat-soluble, which means it generally absorbs best when taken with a meal containing some dietary fat. That detail sounds mundane, but it can change outcomes. A supplement taken on an empty stomach may be less reliably absorbed.
If swallowing pills isn’t feasible, look for alternative formats for the breastfeeding parent—such as softgels—so the mother’s routine remains consistent. Consistency is the silent engine behind better vitamin D status.
What to Expect: Timelines, Transfer, and Realistic Outcomes
Vitamin D isn’t instant. Even when you adjust maternal supplementation, the infant’s status improves over time as the parent’s vitamin D levels stabilize and transfer through milk. Families often notice improvement in the “shape” of routine first (less stress, fewer dosing fights), then see biochemical benefit later.
A typical approach involves starting the maternal dose as recommended and maintaining it consistently. If lab work is planned, it’s usually timed to allow levels to equilibrate rather than repeated every few days. Expect a gradual arc, not a sudden jump.
During the transition, some clinicians may recommend reassessing the need for direct infant supplementation depending on risk factors. Examples of higher risk include limited sun exposure for the household, darker skin pigmentation without adequate sunlight, or a history of maternal deficiency.
Sunlight Strategies: An Adjunct, Not a Replacement
Sunlight can support vitamin D production in the skin, and it can be tempting to rely on it alone. However, sunlight is unreliable. Cloud cover, seasonality, sunscreen use, latitude, and time spent outdoors can all shift vitamin D synthesis dramatically.
For breastfeeding parents, reasonable outdoor time may help as a complement. Yet for infants, direct sun exposure recommendations are more conservative due to skin sensitivity and safety considerations. The common pathway is: mother gets appropriate sunlight exposure within safe guidelines, and vitamin D supplementation fills the gaps.
Think of sunlight as background scoring, while supplements and consistent milk transfer are the main theme.
Dietary Support: Breast Milk’s Limits and the Parent’s Role
Dietary vitamin D can contribute, though it usually isn’t enough on its own for reliable infant protection. Foods such as fatty fish (like salmon or sardines), fortified dairy or plant milks, and egg yolks contain vitamin D, but intake varies and can be modest.
A breastfeeding parent can prioritize vitamin D-rich foods while still supplementing strategically. This combination often creates a more stable supply and may allow for lower supplement doses under clinician guidance.
However, dietary changes are slow and uneven. Breastfeeding routines already demand precision; supplements often provide the predictability that food alone cannot.
Alternative Delivery Methods (Without Infant Drops)
If the goal is “no drops,” there are still options—though many are also limited by availability, taste preferences, or infant age. For the breastfeeding parent approach discussed above, the infant doesn’t receive direct dosing at all, which is usually the cleanest “no drops” solution.
Other possibilities may include fortified foods or infant formulas when supplementation is medically appropriate. For breastfed infants, formula introduction is a larger decision and should be made carefully to avoid disrupting breastfeeding goals. Fortified products and clinician-guided supplementation can be part of a broader plan, but they don’t replace the need for individualized guidance.
Remember: if your plan shifts away from infant drops, ensure the alternative route is actually delivering adequate vitamin D consistently. Convenience is valuable, but adequacy is the nonnegotiable.
When to Consult a Clinician: Red Flags and High-Risk Situations
Some situations warrant extra caution. If the baby has symptoms that could suggest poor vitamin D status—such as poor growth patterns, unusual bone findings, or persistent fussiness—seek medical advice promptly. While symptoms aren’t always specific, early evaluation reduces the chance of delay.
High-risk families often benefit from earlier discussion: preterm infants, exclusively breastfed infants with limited maternal vitamin D intake, households with minimal sunlight, or parents with known vitamin D deficiency. In these cases, a clinician may recommend testing or a more structured maternal dosing plan.
Ask for a tailored plan that addresses your household’s reality: your routine, your diet, your sun exposure patterns, and your preferences around dosing.
Building a Practical Routine: Consistency, Reminders, and Minimizing Stress
Successful vitamin D strategies are rarely complicated; they are consistent. Choose a daily moment tied to a reliable behavior—breakfast, lunch, or a recurring caregiving routine. Set a reminder if it helps. The more seamless the plan feels, the more likely it will survive the chaotic middle weeks of parenting.
If you’re already taking prenatal vitamins, check the vitamin D content before adding extra. Many families accidentally double up. Keep a simple log for a few weeks: what you took, when you took it, and any changes in diet or sun exposure. This isn’t for perfection—it’s for clarity if you later review a plan with a clinician.
In the end, avoiding drops should feel like relief, not risk. When maternal dosing is tailored safely, vitamin D can reach the infant through milk, supporting healthy development while preserving the calm you want around feeding.