Ever wondered why your body seems to “forget” bone upkeep right when life gets busier after 40? One season you’re effortlessly active, and the next you notice stiffness, a slight loss of height, or a lingering ache that wasn’t there before. Here’s the playful truth: bones don’t complain loudly. They simply thin, quietly, like an eraser shaving down a pencil line. The good news? You can build a practical, repeatable Vitamin D–anchored protocol to help maintain bone density.
The Hidden Timing Problem: Why Bone Density Shifts After 40
After 40, the balance between bone resorption and bone formation can tilt. Resorption begins to outpace formation, especially if you’re sedentary, under-sunlit, or not adequately nourished. Bone is not static—it’s living architecture. Think of it like a city constantly renovating its buildings. When maintenance budgets shrink, the scaffolding becomes weaker.
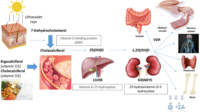
Vitamin D plays the starring role here because it supports calcium absorption in the gut and helps coordinate mineralization. If Vitamin D is insufficient, your body may be “sending calcium signals” without enough calcium arriving. That mismatch can contribute to reduced bone density over time.
First, a Quick Self-Check: Are You at Risk?
Before starting any protocol, take a realistic inventory. Risk doesn’t always announce itself. Consider these common contributors:
Low sun exposure, frequent indoor days, darker skin pigmentation (which reduces cutaneous Vitamin D synthesis), dietary patterns low in calcium, smoking, excessive alcohol, chronic corticosteroid use, thyroid irregularities, and early menopause (for women) can all nudge the system toward bone loss.
Another challenge: training inconsistency. If exercise is sporadic, bones receive fewer “loading” signals. Bone responds to mechanical demand—less demand means less strengthening stimulus.
If possible, talk with a clinician about screening if you have additional risk factors, such as prior fractures or long-term medication use. A baseline matters, because progress is easier to verify than to guess.
Vitamin D: The Anchor Nutrient in Your Bone-Density Protocol
Vitamin D is best thought of as a conductor. It helps orchestrate calcium and bone metabolism. But the “right dose” isn’t one-size-fits-all. Your starting status determines how much support you need.
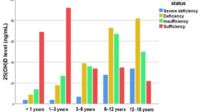
A common, practical approach is to measure a blood marker—25-hydroxyvitamin D. This gives clarity, not vibes. From there, dosing can be tailored. Many adults use daily dosing or structured weekly regimens depending on preference and clinician guidance.
Challenge to expect: digestive tolerance and absorption. Some people absorb better with meals containing fat, while others experience stomach discomfort with certain forms. If you’re prone to reflux or sensitive digestion, take Vitamin D with a substantial meal and monitor tolerance.
Recommended Testing: Labs That Actually Help
Your protocol becomes smarter when it’s measurable. Consider discussing these lab categories with a healthcare professional:
25(OH)D — your Vitamin D status.
Calcium and phosphorus — baseline mineral context.
Parathyroid hormone (PTH) — can rise when Vitamin D is low, a useful “signal” of imbalance.
Sometimes clinicians also evaluate renal function because Vitamin D metabolism and calcium handling depend on kidney health.
When labs guide the plan, you avoid the twin dangers of under-dosing and over-optimizing. Bone wants consistency, not volatility.
Calcium Matters More Than You Think (Even When Vitamin D Is Perfect)
Vitamin D can’t perform without calcium. Imagine an orchestra where one key instrument is silent. Even with excellent conduction, the melody won’t land.
A bone-friendly target is to meet daily calcium needs through food first. Dairy (milk, yogurt, kefir), fortified plant milks, calcium-set tofu, sardines with bones, and certain leafy greens can meaningfully contribute. If food intake is modest, supplements may be considered.
Supplement strategy note: calcium is better handled in smaller doses. Many people find that splitting doses improves absorption and reduces gastrointestinal upset.
And here’s an uncommon but helpful framing: aim for “calcium availability,” not just total grams. Spacing intake across the day often improves utilization.
Exercise: The Mechanical Spell That Tells Bones to Strengthen
If Vitamin D is the conductor, exercise is the rehearsal. Bones respond to mechanical loading—especially resistance training and weight-bearing work. Think of bones as sensory structures: they detect strain and respond by remodeling.
Include:
Resistance training — squats, hip hinges, presses, rows, and step-ups. These create targeted stress that stimulates remodeling.
Weight-bearing activity — brisk walking, stair climbing, hiking, dancing.
Balance and agility — improves fall resistance, a critical factor for fracture prevention.
Try a cadence that you can sustain: 2–4 sessions per week for resistance training is often a solid starting point. Progress gradually. The challenge is not “going hard once.” The challenge is training hard enough, often enough, with excellent form.
The Protocol Schedule: A Realistic Weekly Rhythm
Here’s a practical template. Adapt it to clinician recommendations and lab results.
Daily: Vitamin D taken with a meal (often the largest or fattier one), plus calcium-rich nutrition throughout the day.
Exercise: Resistance training 2–4 days weekly, weight-bearing 3–7 days weekly depending on tolerance, and balance work 3–5 days weekly (short sessions count).
Reassessment: Repeat Vitamin D testing after an interval recommended by a clinician—commonly several months—to confirm the protocol is hitting the desired biochemical range.
Don’t underestimate rest days. Bones strengthen when recovery happens; muscles recover too. A bone-safe routine feels challenging but not chaotic.
Diet Beyond Supplements: Protein, Magnesium, and “Bone-Friendly” Support
Vitamin D and calcium are foundational, but bone remodeling is multidimensional. Protein supports the collagen matrix that gives bone its tensile strength. Inadequate protein intake can weaken that scaffold, even if minerals are present.
Magnesium helps with mineral metabolism and Vitamin D activation pathways. Foods such as nuts, seeds, legumes, whole grains, and leafy greens can contribute magnesium without requiring a separate supplement plan.
Vitamin K2 (commonly discussed in bone health circles) may support calcium utilization pathways. Fermented foods and certain animal sources contain it, while some people use supplements—ideally discussed with a healthcare professional, especially if you take anticoagulants.
Common Pitfalls: Why People Stall After Starting
One year of motivation doesn’t always survive the following year. The protocol often breaks in predictable places:
Inconsistent dosing — forgetting days leads to underperformance.
Overlooking food calcium — Vitamin D cannot compensate for low intake.
Low-impact-only habits — swimming is excellent for fitness, but bones often need targeted loading.
Ignoring balance — improving strength without fall prevention is like tightening bolts while leaving loose hinges.
Also, consider medication interactions. Some drugs affect Vitamin D metabolism, calcium absorption, or bone turnover. If you take long-term medications, bring this protocol into the conversation with a clinician.
Safety and Boundaries: How to Avoid Overdoing It
Vitamin D is fat-soluble, which means excess can accumulate. That’s why lab-guided dosing is valuable. Symptoms of excess Vitamin D and hypercalcemia can include nausea, constipation, fatigue, and confusion—serious issues that should be addressed promptly.
Stay within recommended limits unless a clinician is actively supervising higher dosing. If you have kidney disease, a history of kidney stones, or hyperparathyroidism, professional guidance is especially important.
Make It Stick: A Bone-Confidence Mindset for the Long Run
Here’s the final playful challenge: can you treat bone density like a daily ritual rather than a rare event? Small choices compound—Vitamin D with meals, calcium-rich meals, two strength sessions, a short balance drill, and a walk that happens even when your schedule looks messy.
With a coherent Vitamin D–anchored protocol and consistent mechanical loading, your bones receive a clear message: we’re building strength, not merely chasing numbers. Bone health becomes less about fear and more about craftsmanship—steady, deliberate, and quietly powerful.