In older adulthood, the body can feel like a library with aging scaffolding: books remain, yet the shelves grow wobbly. Two systems quietly determine whether those shelves stay upright—muscle that provides strength and bones that provide structure. Vitamin D sits at the center of that architecture. It is less a single nutrient and more a conductor of calcium, muscle function, and skeletal remodeling. When vitamin D drifts too low, the performance degrades. When it is restored thoughtfully, the body can regain a steadier rhythm—one that supports both sarcopenia prevention and long-term bone health.
Sarcopenia and the Quiet Collapse of Power
Sarcopenia is not simply “weakness.” It is a progressive decline in skeletal muscle mass and function, often accompanied by slower gait, reduced grip strength, and an increased vulnerability to falls. It is a creeping erosion: the decline may look gradual, but the consequences are immediate when daily tasks become labored—rising from a chair, climbing stairs, or carrying groceries.
Muscle needs more than calories. It needs signaling. It needs calcium handling. It needs mitochondrial efficiency. Vitamin D appears in these pathways like a backstage engineer tuning the gears that allow contraction, recovery, and endurance. While vitamin D does not “build muscle” in a direct, instant way, inadequate levels can correlate with poorer muscle performance and a higher risk of decline.
Think of muscle fibers as engines. Vitamin D helps maintain the electrical and chemical choreography that allows those engines to ignite reliably. Without sufficient vitamin D, the ignition system becomes erratic—more fuel is required for the same output, and fatigue arrives sooner.
Bone Health: Remodeling Requires a Reliable Signal
Bones are not inert. They are living scaffolds continually remodeled through a balance of formation and resorption. With age, this balance can tip, leading to reduced bone mineral density and greater fragility—an invitation to fractures even after minor stress. Osteoporosis and osteopenia become less theoretical and more practical concerns.
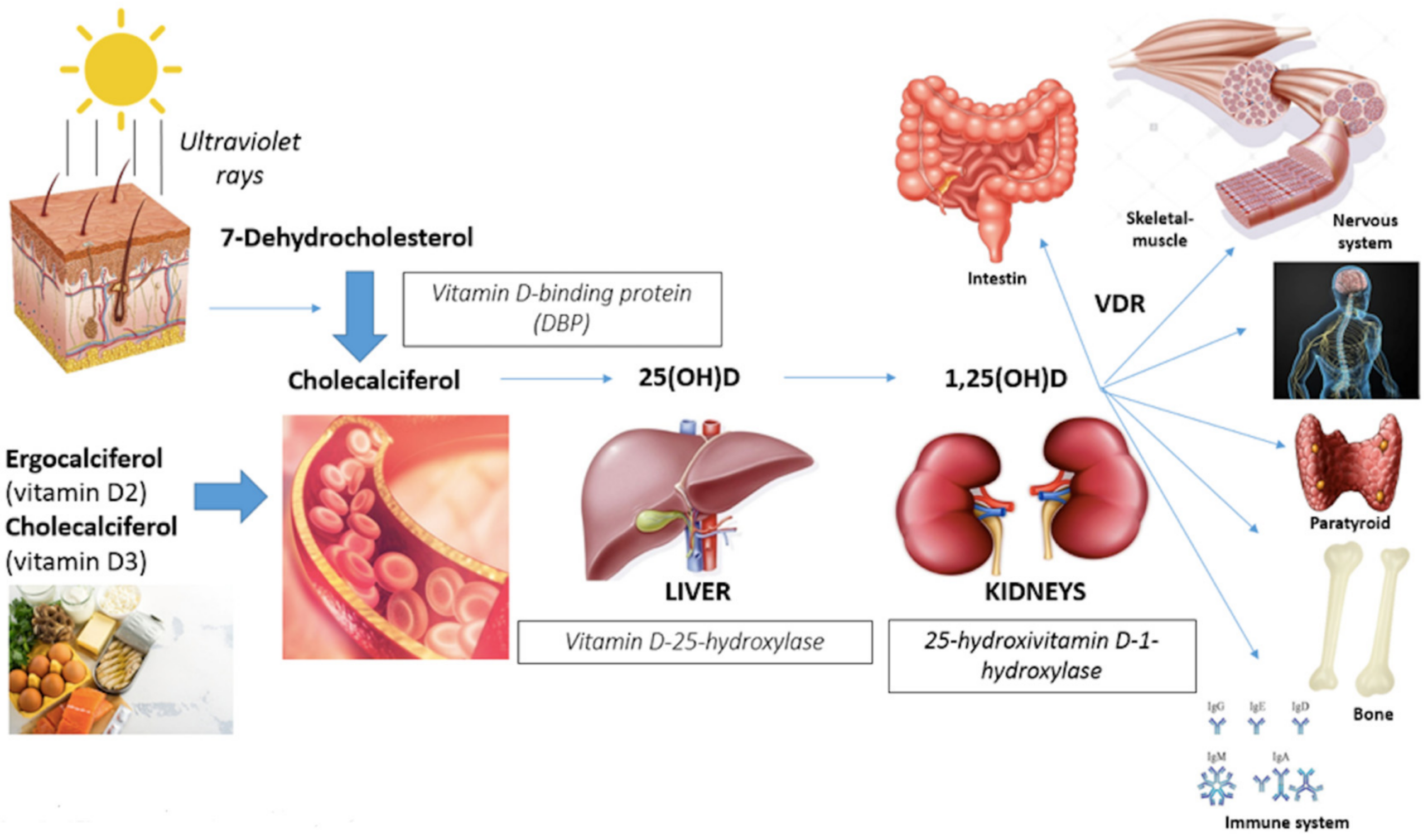
Vitamin D is crucial because it supports intestinal absorption of calcium and phosphate. Calcium is the building block; vitamin D is the courier that delivers the materials to where mineralization needs them. If vitamin D is scarce, calcium absorption drops. The body may compensate by borrowing calcium from bone, which can weaken the skeleton over time.
In this way, vitamin D functions like a foreman overseeing a construction site. Without it, materials arrive late, work is incomplete, and the final structure is less resilient.
How Vitamin D Influences Muscle Function
The relationship between vitamin D and muscle is multifaceted. Vitamin D receptors appear in muscle tissue, suggesting a direct role in muscle biology. It supports pathways involved in protein synthesis, muscle cell differentiation, and neuromuscular function.
Muscle contraction is an intricate choreography. Calcium is the central propellant. Vitamin D supports calcium availability and influences how muscle cells manage calcium dynamics. When those dynamics falter, muscle strength and power decline.
Vitamin D also interacts with inflammation and oxidative stress—two processes that often intensify with age. Excess inflammatory signaling can impair muscle quality, turning exercise adaptations into harder-won victories. With adequate vitamin D, the body may be more capable of mounting effective repair and maintaining functional capacity.
Short sentence, long impact: when vitamin D is adequate, the muscular “signal-to-noise ratio” improves.
Mechanisms at the Crossroads: Calcium, Nerves, and Inflammation
Falls are a bridge between muscle weakness and bone injury. Vitamin D can influence fall risk through several indirect routes. It affects muscle strength, coordination, and potentially reaction time. It also supports nerve function through calcium-dependent signaling.
Meanwhile, aging is often accompanied by a pro-inflammatory drift. Chronic, low-grade inflammation can degrade muscle performance and bone microarchitecture. Vitamin D’s immunomodulatory properties may help restrain that drift, creating a biological environment more favorable to strength and skeletal integrity.
Picture the body as a city. Muscle and bone are different neighborhoods, but they share utilities. Vitamin D helps keep the utilities running—power lines for calcium movement, communication channels for nerve signaling, and regulators for inflammatory traffic.
Osteosarcopenia: When Bone and Muscle Decline Together
There is a convergence phenomenon sometimes described as the overlap of osteopenia/osteoporosis with sarcopenia. This combined vulnerability—sometimes framed as “osteosarcopenia”—is especially relevant for older adults, because muscle weakness increases the risk of falls while weakened bones increase the consequence of each fall.
In practical terms, this is why vitamin D can be a strategic priority. Restoring vitamin D status can support both ends of the problem: the engine of movement and the framework that absorbs impact.
When both muscle and bone are under strain, recovery becomes slower. Vitamin D is one of the factors that may help tilt the balance back toward resilience.
Testing and Targeting: Knowing Where the Body Stands
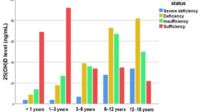
Vitamin D status is typically assessed by measuring serum 25-hydroxyvitamin D, the most useful indicator of body stores. Because sun exposure varies widely—latitude, skin tone, clothing habits, seasonal changes, indoor lifestyle—assumptions can mislead. Two people can live the same lifestyle and have very different vitamin D levels due to differences in absorption, diet, body composition, and genetic variability.
Once levels are known, supplementation can be individualized. The goal is not maximality; it is adequacy—enough to support muscle function and bone metabolism without excessive dosing.
Long sentence, simple conclusion: dosing should be calibrated to both lab results and clinical context, including age, medication profile, kidney function, and overall fracture risk.
Supplementation Strategies: Dose, Consistency, and Context
Vitamin D can be obtained through limited dietary sources and sunlight exposure, but supplementation often becomes the reliable route for older adults. Many regimens use daily dosing or periodic higher doses depending on medical guidance. Consistency matters. Vitamin D behaves like a seasonal account balance; fluctuating levels can lead to uneven physiological support.
It is also important to ensure adequate calcium intake. Vitamin D without sufficient dietary calcium is like a key without a door—processes need both elements to work smoothly. Some individuals may require calcium supplementation, but that decision should be individualized.
If magnesium is low, certain metabolic steps may also be impaired. Protein intake also shapes outcomes for muscle—vitamin D helps set conditions, but muscle still requires building materials and training stimulus.
Consider this an ecosystem, not a single lever. Vitamin D is powerful, yet it performs best in harmony with nutrition, exercise, and overall health management.
Safety Considerations: Avoiding the Extremes
While vitamin D is generally safe when appropriately dosed, excessive intake can raise calcium levels and increase the risk of complications such as hypercalcemia. This is particularly relevant for individuals with kidney disease, certain granulomatous disorders, or those taking medications that affect calcium balance.
Monitoring can matter. Clinicians may recommend follow-up labs, especially for those on long-term supplementation, those with complex medical histories, or those receiving higher doses.
Moderation is not a limitation; it is precision. The body prefers stable, sustainable support to abrupt surges.
Exercise Synergy: Vitamin D Works Like a Match with Movement
Vitamin D and exercise are complementary. Resistance training improves muscle mass and strength, while vitamin D supports the biological environment that may enhance recovery and functional gains. Balance training and gait training can reduce falls, and that protective effect multiplies the value of skeletal health.
Think of vitamin D as the lighting in a workshop. Strength training provides the carpentry. Bone health benefits from mechanical loading, and adequate vitamin D supports the mineralization response.
Even a simple routine—progressive resistance exercises, regular walking, structured balance practice—can create the stimulus that the body can translate into better strength. Vitamin D helps ensure the translation is efficient.
Nutrition and Lifestyle: Strength is Not a Single-Ingredient Story
Vitamin D interacts with the broader dietary pattern. Protein sufficiency supports muscle protein synthesis. Omega-3 fatty acids may influence inflammation. Fruits and vegetables supply antioxidants that can help counter oxidative stress. Adequate calories prevent catabolic drift.
Sleep, hydration, and smoking cessation also matter. Bone health and muscle function are both sensitive to the endocrine environment, and chronic stress can interfere with recovery processes.
Sunlight exposure can contribute, but practical barriers—winter seasons, mobility limits, and skin cancer concerns—often make supplementation a more controlled strategy. The best plan respects both safety and consistency.
Taking Action: A Practical, Patient-Centered Approach
The most compelling appeal of vitamin D is its dual relevance. It touches the muscle engine and the skeletal framework—two systems that age often compromises simultaneously. For older adults, this makes it a cornerstone candidate in a comprehensive plan aimed at functional independence.
Start with awareness: consider testing if vitamin D status is unknown, especially if there is limited sun exposure, dietary insufficiency, history of falls, or known low bone mineral density. Next, incorporate supplementation when indicated, paired with calcium adequacy and sufficient protein. Then, anchor the plan with resistance training and balance work.
In the end, vitamin D is not merely about numbers on a lab report. It is about staying upright, moving with confidence, and reducing the odds that a small misstep becomes a major setback.
Altogether, vitamin D is a stabilizer—an internal signal that helps keep muscles responsive and bones resilient, so everyday life remains less precarious and more firmly within reach.