Kidney stones often arrive like an uninvited visitor: quiet at first, then unmistakably painful. Yet beneath the ache lives a subtler story—one about mineral chemistry, microscopic crystallization, and the body’s ongoing negotiation with calcification. In recent nutrition conversations, two acronyms keep appearing for their potential relevance to this negotiation: D3 and K2. Together, they’re sometimes discussed as a strategy for supporting kidney health and reducing calcification risk. But the real intrigue isn’t just in what they “do.” It’s in how they may help shift the body’s perspective—nudging minerals toward the right destinations, and away from the wrong ones.
Understanding Calcification Risk: When “Minerals” Become “Crystals”
Kidney stones are not merely deposits; they are organized assemblies that begin as microscopic crystals. Calcium-based compounds are among the most common offenders, and their formation is influenced by urine chemistry—pH, volume, inhibitor availability, and concentration. When urine becomes saturated with stone-forming ions, crystallization becomes statistically more likely. From there, the process can accelerate as crystals aggregate and resist natural “anti-stone” mechanisms.
Here’s the curious part: not all calcium is the same in biological terms. The body treats minerals like a logistics network. When regulation falters, calcium can be recruited into inappropriate pathways. Calcification, in this framing, isn’t only a kidney issue—it’s a whole-body coordination problem. D3 and K2 enter the conversation because they sit near the junction where mineral handling, tissue signaling, and calcium routing overlap.
Vitamin D3: The Primer for Mineral Signaling
Vitamin D3 (cholecalciferol) functions less like a simple nutrient and more like a molecular messenger. Its best-known role is supporting calcium absorption in the gut. But “supporting absorption” is not automatically synonymous with “stone prevention.” In fact, the relationship between vitamin D and stones is nuanced: vitamin D can raise calcium availability, and in certain contexts that could theoretically increase urinary calcium. The key is not just dosage—it’s balance, timing, and the body’s downstream ability to direct minerals appropriately.
When vitamin D status is deficient, calcium absorption and bone mineralization may suffer. That can trigger compensatory physiology, including shifts in parathyroid hormone signaling. Over time, these changes can indirectly affect urine chemistry and the stability of mineral phases. In other words, the question becomes: is the body running on a shortage that distorts the system? Or is the system already saturated and needs restraint?
D3 helps “set the stage.” But stagecraft matters. Without proper partners, the play can go sideways.

Vitamin K2: The Redirector of Calcium’s Fate
Vitamin K2 is often described as a “calcium courier” because it supports proteins that regulate where calcium should—or should not—accumulate. The best-known mechanism involves activating vitamin K–dependent proteins such as osteocalcin (bone-related) and matrix Gla protein (associated with preventing inappropriate calcification in tissues). While the kidney is the site where stones form, the broader mineral environment influences urinary composition. If the body is encouraged to handle calcium in a more orderly fashion, the urine may be less primed for crystal formation.
K2 doesn’t create calcium from nothing. Instead, it refines the body’s ability to use calcium where it belongs. Consider how this changes the perspective: rather than trying to block calcium entry or “starve” minerals—which can be physiologically clumsy—K2 suggests an optimization strategy. It nudges mineral traffic toward structural storage and away from chaotic deposition.
Different forms of K2 exist, including MK-7 and MK-4. They have different kinetics in the body, which may matter for timing and consistency. The deeper point is that K2 is not about one dramatic effect; it is about sustained biochemical governance.
The “D3 + K2” Theory: More Than a Pairing, a Workflow
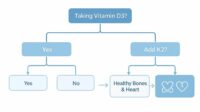
The combined idea of D3 + K2 is often framed as a workflow: D3 improves mineral availability and signaling; K2 supports proteins that guide calcium placement and discourage ectopic mineralization. When these are mismatched—high D3 without adequate K2, for instance—the body’s ability to manage calcium’s destination could be stressed. That stress, in theory, may contribute to conditions that favor calcification.
But even this theory deserves humility. Kidney stones are heterogeneous. Calcium oxalate stones differ from uric acid stones, and cystine stones follow their own rules. Some people are primarily driven by urine volume; others by inhibitors like citrate; others by hypercalciuria. Therefore, D3 + K2 is not a universal “stone antidote.” It is more plausibly a support mechanism for a certain slice of the mineral-handling puzzle.
The promise is a shift in mindset: from reaction to prevention, from crude supplementation to aligned physiology, from “more nutrients” to “better orchestration.”
Calcification Risk and Why Placement Matters
Calcification risk is not solely about calcium intake. It’s about the equilibrium between promotors and inhibitors of crystallization. In urine, inhibitors such as citrate can keep crystals from growing and aggregating. In tissues, regulatory proteins influence whether calcium settles into structured frameworks or inappropriate niches.
When mineral placement is well-regulated, calcium is likelier to be incorporated into bone and kept from roaming. When placement is poorly regulated, calcium can become more “available” for problematic pathways—potentially including stone formation. D3 provides a lever by increasing calcium absorption, and K2 supports the locking mechanisms that direct calcium toward preferred destinations.
There’s also an emotional dimension to this chemistry: the body prefers order. Give it the right signals, and it often knows what to do. The goal is to strengthen those signals, not to wrestle the system with guesswork.
Who Might Benefit: Context, Risk Profiles, and Stone Types
Not every kidney stone story is the same. If someone has a history of calcium-based stones, or urinary patterns suggesting increased calcium availability, the D3 + K2 framework may feel more relevant. Conversely, individuals with different stone etiologies may need other interventions: urine alkalinization strategies, cystine-binding approaches, or oxalate-targeted nutrition patterns.
Risk is also influenced by factors such as dehydration, dietary sodium, high-dose vitamin C (in some contexts), and metabolic conditions. Medication history can matter too. Some drugs affect calcium handling or urine pH. In that sense, D3 and K2 should be evaluated as pieces of a larger board, not as lone chess knights delivering checkmate.
Still, the curiosity remains justified: for certain people, correcting vitamin D deficiency and ensuring adequate K2 status might support healthier mineral governance—and that is, at minimum, a plausible prevention pathway.
Dosage Caution: The Fine Line Between Support and Excess
Here is where practicality matters. Vitamin D3 is powerful. Too little may lead to deficiency-related downstream changes; too much may increase calcium availability beyond what the body can manage. That doesn’t mean D3 should be avoided. It means it should be treated with respect.
Similarly, K2 is involved in coagulation pathways. If someone uses anticoagulant therapy such as warfarin, vitamin K intake can interfere with medication effects. That’s not a reason for panic—it’s a reason for coordination with healthcare professionals.
Rather than chasing mega-doses, an evidence-informed approach often begins with assessing baseline status (such as 25-hydroxyvitamin D) and evaluating whether supplementation is truly needed. Then the conversation can shift from speculation to calibration.
Beyond Supplements: The Anti-Stone “Environment” You Can Control
Even perfect mineral signaling can be undermined by unfavorable urine conditions. Hydration is foundational. A higher urine volume dilutes stone-forming ions, reducing saturation. Dietary sodium is another lever: high sodium can increase urinary calcium excretion. Meanwhile, dietary patterns that support citrate—often through fruits and vegetables—may help keep crystals from gaining momentum.
Oxalate also plays a role in calcium oxalate stones. Limiting very high-oxalate foods in susceptible individuals can reduce the burden of stone-forming material. But the goal isn’t deprivation for its own sake; it’s targeted moderation aligned with personal risk.
Think of the body like a river system. D3 + K2 may influence the mineral traffic rules, while hydration and diet influence the flow rate and chemical composition that determine whether crystals can form.

Timing and Consistency: The Quiet Power of Regularity
Supplements work best when they integrate into routine physiology. Vitamin D3 is typically absorbed with dietary fat, and consistency may matter more than occasional large dosing for maintaining stable status. K2’s different forms may also suggest different preferences for timing, though the overarching principle is steady support rather than sporadic swings.
Long sentences can describe biochemistry; short sentences can describe lived reality. People often notice that prevention is less dramatic than treatment. It’s the daily accumulation of favorable conditions—regular hydration, consistent dietary choices, and balanced micronutrients—that makes the biggest difference.
In this sense, D3 + K2 becomes less like a “cure” and more like a maintenance contract.
Monitoring Progress: Turning Curiosity into Evidence
Because kidney stone prevention is individualized, monitoring strengthens the connection between theory and reality. Healthcare providers may evaluate urine parameters such as volume, pH, calcium, oxalate, citrate, and supersaturation. Blood tests may also assess vitamin D status and calcium balance. The aim is to see whether interventions are improving the biochemical environment.
This is where the shift in perspective becomes practical. Instead of guessing, you measure. Instead of hoping, you track. Instead of reacting to a painful episode, you aim for fewer surprises.
Summing Up: A Promise of Better Mineral Logistics
D3 + K2 for kidney stone prevention is best understood as an approach to mineral logistics—supporting calcium handling in a way that may reduce calcification risk under the right conditions. Vitamin D3 helps calibrate calcium absorption and signaling. K2 supports calcium-dependent proteins that may discourage inappropriate calcification and support orderly mineral placement.
Yet prevention is not a single lever. It’s a system: hydration, dietary sodium moderation, citrate support, appropriate oxalate handling when relevant, and careful supplementation that respects individual risk and medication considerations. When these pieces align, the story shifts from crisis to continuity.
Kidney stones don’t only reflect what the body lacks. Sometimes they reflect what the body mismanages. D3 + K2 proposes a more elegant question: what if the goal isn’t just to reduce minerals, but to redirect them with intention?