Your stomach has a way of turning meals into meaning. It isn’t just churning food—it’s staging a chemical symphony where acid acts like the conductor’s baton. And yet, when people begin taking calcium and vitamin D as if they were simple supplements, they sometimes forget one intimate truth: timing matters, and the stage matters too. The “stomach acid factor” is the quiet hinge on which absorption swings, especially when calcium meets the acidic microclimate of your meal.
Acid as the Invisible Architect
Think of gastric acid as an invisible architect—unseen, unromantic, but essential. It prepares the dinner you eat by loosening bonds, improving solubility, and helping your digestive environment process minerals that would otherwise remain stubbornly inert.
Calcium, in particular, doesn’t merely “arrive” in the body. It must be unlocked from its chemical form. When acid is available at the right moment, certain calcium compounds may dissolve more readily. That dissolution can influence how efficiently calcium travels onward to where absorption occurs.
This is why the phrase “take calcium and D with meals” often isn’t just habit—it’s strategy. It aligns supplement delivery with the same physiological window that helps food itself be transformed.
Why Timing Beats Willpower
Shortly after a meal begins, the digestive system shifts gears. Acid secretion can rise, gastric pH may fall, and enzymes start working at full intensity. Your supplement, if taken at the same time, enters a landscape designed to process dietary substances.
In contrast, taking calcium on an empty stomach can sometimes create a mismatch. The supplement arrives at a time when the stomach is calmer, and the surrounding chemistry may not be as supportive. The result might be less efficient absorption—or simply more digestive discomfort, depending on the person.
Long sentences have their place, but digestion has even more: when you pair calcium with the meal that triggers your body’s biochemical choreography, you’re not just taking something—you’re coordinating with your physiology.
Calcium Forms: Not All Calcium Is Created Equal
Calcium is a category, not a single substance. Different forms behave differently in the stomach. Some are more forgiving about acidity, while others may be more dependent on an acidic environment.
For example, calcium carbonate is often advised with meals because its solubility improves when stomach acid is present. Calcium citrate, by comparison, is generally less dependent on acidity, and some people tolerate it better—yet meals can still help reduce stomach-related irritation for many individuals.
The “stomach acid factor” becomes more than a concept when you choose a product. Checking the label for the type of calcium can clarify which approach is likely to work best for your body’s chemistry.
Vitamin D: The Key That Helps Calcium Enter the Story
Vitamin D is not the door—it’s the permission slip. It helps regulate calcium absorption and supports bone mineralization. Without adequate vitamin D status, calcium can arrive and still struggle to be used effectively.
Because vitamin D is fat-soluble, it often benefits from the presence of dietary fat. That doesn’t mean you need to eat junk food; it means that taking vitamin D alongside a meal—especially one containing some fat—may improve its absorption compared with taking it on a fasting stomach.
So the pairing makes narrative sense: calcium provides the mineral substance, while vitamin D provides the biological “stage directions” that help your body incorporate it.
A Subtle Balancing Act: Acid Too Low, Acid Too High
Most people think of stomach acid only as an enemy—something associated with heartburn. But acid isn’t only a villain; it’s also a tool. Both extremes can complicate the mineral pipeline.
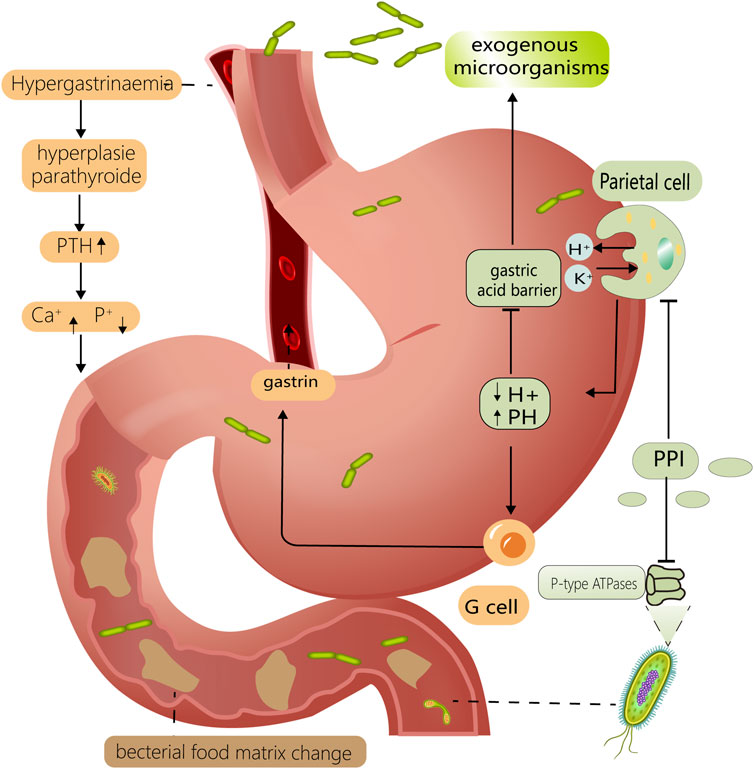
If gastric acid is chronically suppressed—sometimes due to long-term use of acid-reducing medications—calcium absorption may shift. That doesn’t automatically mean supplements are useless. It means the strategy should be individualized: the form of calcium, the timing, and overall dietary context matter.
On the other hand, if someone experiences frequent reflux, taking calcium in a way that aggravates symptoms can backfire emotionally. The stomach doesn’t care about supplement intentions; it cares about sensation. For some people, splitting doses, changing forms, or coordinating with meals can reduce irritation.
How to Take Calcium and D with Meals (Practical Precision)
Start with consistency. A stable routine trains your digestive timing. Many people do well when taking calcium and vitamin D with the first substantial meal of the day or with lunch—times when digestion is most reliably active.
If your dose is high, consider dividing it. Calcium absorption can be more efficient in smaller increments. This also tends to feel gentler on the stomach. Your body may prefer a “series of sips” rather than one “large gulp.”
Pairing with a meal that includes some fat can be particularly supportive for vitamin D. Think of it as providing travel companions—nutrients moving together rather than arriving alone at an empty station.
When Stomach Acid Becomes a Medical Conversation
There are times when this topic deserves clinical attention. Persistent reflux, unexplained digestive changes, or symptoms like bloating and discomfort after supplement use warrant a careful conversation with a healthcare professional.
People taking medications that reduce stomach acid—commonly proton pump inhibitors or similar therapies—may have altered gastric conditions. That doesn’t invalidate calcium and D. It means the “stomach acid factor” is no longer a theoretical variable—it’s a measured one.
Also consider underlying conditions affecting digestion or absorption. If the stomach is compromised, the solution often isn’t simply adding more supplements. It’s adjusting the entire plan: formulation, timing, and nutrition.
Dietary Allies: Food That Supports the Pipeline
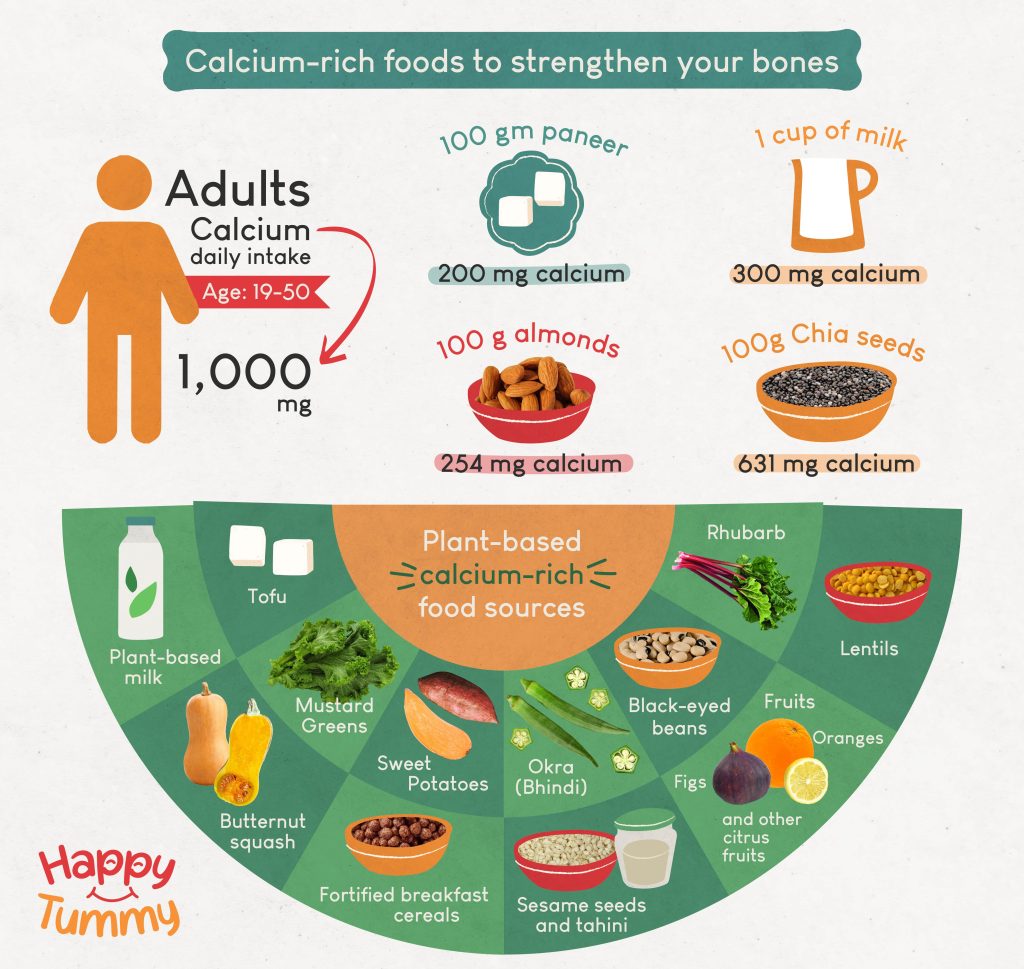
Supplements are helpful, but they’re not the only architects in the building. A calcium-rich diet—dairy, fortified alternatives, leafy greens—can provide a baseline that reduces dependence on supplements. Meanwhile, vitamin D can come from fortified foods and sensible sun exposure, though many individuals still require supplementation.
Eating patterns can also influence digestion comfort. If reflux is part of the picture, choosing meals that are less likely to trigger symptoms may make it easier to take supplements consistently.
In other words: food is the environment. Supplements are the guests. A well-prepared environment allows good guests to do their best work.
Intriguing Takeaway: Make the Stomach Your Timing Partner
The “stomach acid factor” isn’t about fear—it’s about alignment. When calcium and vitamin D meet your meal, they arrive with the right biochemical weather. Acid becomes not an antagonist, but a facilitator. Time becomes not a detail, but a variable you can control.
So the narrative is simple yet potent: coordinate the moment, choose the right form, consider how your body reacts, and let your digestion do what it was designed to do. When your stomach is part of the plan, supplements stop feeling like separate acts—and begin to feel like chapters in the same story.