There is a peculiar moment most people recognize: the bathroom mirror suddenly feels less reliable, the hairline seems to drift backward, and the scalp begins to show itself with uncomfortable clarity. When the pattern is patchy rather than diffuse, the conversation often turns to alopecia areata—an autoimmune hair-loss condition that can appear with astonishing suddenness. In the midst of that confusion, one question repeats itself in clinics and kitchens alike: could vitamin D deficiency be part of the story?
It’s tempting to treat vitamin D like a simple “deficiency fix,” but biology rarely behaves so linearly. Vitamin D is not just a nutrient; it’s a signaling system. And alopecia areata isn’t merely hair shedding—it’s immune misdirection. The fascination lies in how these two narratives intersect: a deficiency that seems mundane can, under the right immunologic circumstances, become strangely consequential.
Understanding Alopecia Areata: When the Immune System Turns Its Attention Inward
Alopecia areata is often described as an autoimmune condition because the immune system attacks structures within the hair follicle. This does not mean the body is “infected” in the ordinary sense. Instead, immune cells interpret follicular cues incorrectly, leading to inflammation around the follicle and a shift into a resting phase. The result can be smooth, well-demarcated patches of hair loss, sometimes progressing to more extensive involvement.
It can feel disorienting—one season you’re brushing normally, and the next you’re observing scalp like it’s a map. Some people experience regrowth and then relapse, as if the biology is running a loop. That cyclical quality is a key reason researchers and clinicians linger on underlying drivers rather than focusing only on outward symptoms.
Vitamin D: More Than Sunshine, More Than Bone
Vitamin D is frequently associated with skeletal health, but its influence extends well beyond bones. Cells throughout the body—including immune cells—carry vitamin D receptors. These receptors respond to vitamin D in a way that can affect gene expression, immune regulation, and inflammatory signaling. In other words, vitamin D behaves like a conductor in an orchestra: it doesn’t play every note, but it shapes the overall tempo and balance.
When vitamin D levels are low, that regulatory choreography can falter. The immune system may become more reactive, less tolerant, or simply less able to maintain the delicate “don’t attack yourself” boundary. It’s not that vitamin D deficiency automatically causes alopecia areata. Rather, it may remove a protective layer—an immunologic airbag—making susceptibility more likely.
The Common Observation: Low Vitamin D Shows Up in Conversations About Hair Loss
One of the most common clinical patterns is deceptively simple: people with alopecia areata often find that their vitamin D levels are below optimal. This observation can spark hope, because deficiency is measurable and sometimes correctable. A blood test offers a kind of clarity in an otherwise ambiguous experience.
But here’s the deeper nuance: low vitamin D may be both a contributor and a marker. It can contribute by weakening immune regulation. It can also reflect lifestyle factors—sun exposure habits, indoor routines, skin coverage choices, and even cultural or geographic circumstances—that correlate with broader immunologic differences. The overlap invites a question that goes beyond “Is vitamin D involved?” and leans toward “Why does vitamin D become such a focal point in autoimmune contexts?”
The fascination, then, is partly pragmatic: vitamin D is accessible. Yet the fascination is also intellectual: immune pathways appear to be listening for vitamin D signals, and alopecia areata seems to be among the conditions where that listening matters.
Vitamin D Receptors and Immune Signaling: The Molecular Bridge
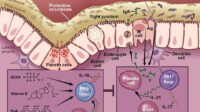
Vitamin D exerts its effects through vitamin D receptors, which are present on multiple cell types, including immune cells. When vitamin D binds to these receptors, it can influence processes such as cytokine production and immune cell differentiation. Cytokines are chemical messengers that help immune cells coordinate responses—some promote inflammation, others help dampen it.
Alopecia areata features immune-mediated inflammation in the vicinity of the hair follicle. If vitamin D signaling helps maintain immune balance, then insufficient vitamin D could tilt the system toward a more inflammatory posture. That tilt might not be the only factor, but it could be a relevant lever—especially in individuals with genetic predisposition or other autoimmune tendencies.
Why Deficiency Might Be So Sticky: Lifestyle, Genetics, and Autoimmune Predisposition
Vitamin D deficiency can be easy to understand—less sunlight, more time indoors, seasonal variation, higher latitudes, darker skin pigmentation, and limited dietary intake can all reduce vitamin D synthesis and absorption. Yet the autoimmune part adds another layer. Some people may be genetically primed to respond to immune cues more intensely. In such cases, a deficiency might function like kindling: the immune system is already susceptible, and vitamin D shortfall provides the spark or amplifies the flame.
This creates a practical paradox. Two people can have similar vitamin D levels, but only one develops noticeable autoimmune hair loss. That suggests multiple determinants are in play: genetic background, immune history, hormonal influences, stress physiology, skin barrier differences, and possibly microbial or environmental factors. Vitamin D may still matter, but it’s rarely the lone protagonist.
Signs and Symptoms: When Hair Loss Meets Systemic Context
Alopecia areata is primarily a hair-loss condition, but it often arrives within a broader context of immune dysregulation. Some individuals report associated nail changes (such as pitting or ridging), or experience atopic tendencies. While vitamin D deficiency can be silent, it may also associate with fatigue, generalized aches, or mood changes—symptoms that are nonspecific but can help raise suspicion.
Because these symptoms overlap with many conditions, a targeted approach is wise. Asking a clinician about vitamin D status can be reasonable, particularly when hair loss begins abruptly, becomes recurrent, or coexists with other autoimmune concerns.
Testing and Interpretation: What “Low” Really Means
Vitamin D status is commonly assessed via a blood test measuring 25-hydroxyvitamin D. Interpretation is not uniform across all guidelines, but most clinicians aim for levels that support immune and skeletal functions. Importantly, “borderline” results can still be relevant for some people, especially when an autoimmune condition is already present.
Another subtle point: vitamin D interacts with other nutrients and physiologic variables. Magnesium status, overall nutrition, liver function, kidney health, and body weight can all influence vitamin D metabolism. Therefore, deficiency correction is most effective when it’s approached as an ecosystem rather than a single number.
Correcting Deficiency: Supplementation, Safety, and Realistic Expectations
Correcting vitamin D deficiency often involves supplementation alongside lifestyle adjustments such as safe sun exposure and dietary improvements. Supplementation should be tailored to baseline levels and medical history, because excessive vitamin D can cause hypercalcemia and related complications. This is not meant to discourage treatment—it’s meant to underline responsible dosing.
As for alopecia areata, it’s important to set expectations with nuance. Restoring vitamin D might support immune regulation, potentially improving the internal environment for hair follicle recovery. However, alopecia areata can fluctuate naturally. Some individuals regrow hair even without correction; others need additional therapies. Vitamin D may enhance the odds, but it rarely substitutes for comprehensive dermatologic management.
Beyond Vitamin D: The Broader Immunologic Landscape of Alopecia Areata
To focus exclusively on vitamin D is to risk oversimplification. Alopecia areata involves a multifaceted immune landscape. Treatments often range from topical and injectable anti-inflammatory approaches to systemic therapies in more extensive cases. Emerging biologic therapies have reshaped expectations for some patients, especially when disease is persistent.
Vitamin D fits into this larger framework as a modulatory factor—an immune “volume knob” rather than a complete off-switch. That’s precisely why it captures attention: it offers a plausible mechanism that aligns with autoimmune behavior, yet it respects the complexity of the condition.
When to Seek Care: Timelines and Practical Next Steps
Patchy hair loss can be emotionally jarring. If you notice sudden, well-defined bald spots, rapid progression, or associated nail changes, dermatologic evaluation is a sensible next step. Early assessment helps confirm diagnosis and guides treatment planning. In the same conversation, vitamin D testing can be considered as part of a holistic autoimmune review.
Alopecia areata can be persistent, but it is not hopeless. Many people experience periods of regrowth. The goal is not only to chase hair, but to stabilize immune processes so regrowth has a better chance to endure.
A Deeper Fascination: Why This Link Feels Personal and Scientific at Once
The reason people keep returning to vitamin D in the context of alopecia areata is not just the availability of supplements or the simplicity of a blood test. It’s the convergence of two themes: a deficiency that seems external and ordinary, and an autoimmune condition that feels internal and disorienting. Vitamin D sits at the intersection, acting like a biological mediator that bridges environment, immune regulation, and follicular fate.
In that intersection lies a kind of quiet hope: not that vitamin D alone will solve everything, but that understanding immune “listening cues” can turn uncertainty into strategy. Hair loss may begin as a visible problem, but the most meaningful improvements often start deeper—where signaling, tolerance, and inflammation negotiate the future of each follicle.