Have you ever wondered whether your morning routine is quietly leaving you “vitamin D deficient” even when you’re trying your best? For seniors over 65, that question isn’t just quirky—it can be consequential. Vitamin D is the backstage crew of the body: it helps regulate calcium, supports musculoskeletal strength, and influences immune function. Yet as we age, the body’s ability to synthesize vitamin D through sunlight can become less efficient, and dietary intake may also lag. The result? A surprisingly common nutritional bottleneck that can creep in with no obvious drama—until bones, muscles, and overall resilience start to feel the effects.
Why Vitamin D Becomes Tricky After Age 65
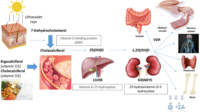
Vitamin D production is a bit like baking bread: you need the right ingredients and the right heat. In younger adults, sunlight provides “heat” and the skin converts it into usable vitamin D precursors. After 65, that conversion rate can decline. Combine that with factors such as reduced outdoor time, more sunscreen coverage, darker skin pigmentation, and changes in diet or absorption—and the odds of low vitamin D rise.
There’s also the issue of physiology. Vitamin D is fat-soluble, and it travels through the body via lipid pathways. Seniors may experience changes in body composition, gastrointestinal function, or chronic conditions that can affect absorption. Add certain medications—like some anticonvulsants or glucocorticoids—and the challenge becomes multifaceted.
So the playful question becomes sharper: If the body is “less efficient at baking,” how do we ensure enough vitamin D is still delivered?
How Much Vitamin D Do Seniors Over 65 Need? (General Targets)
For most adults older than 65, common guideline targets for daily intake are 800 IU (20 micrograms) per day. This serves as a practical baseline for routine maintenance when sunlight exposure is limited and diet alone may not fully cover needs.
Think of 800 IU as a steady “drip” rather than a one-time megadose. For many seniors, that consistent baseline helps maintain adequate blood levels—especially when combined with calcium intake and healthy mobility.
However, needs are not always one-size-fits-all. Baseline intake can be sufficient for some people, while others require higher supplementation to correct deficiency. That’s why blood testing matters when symptoms, risk factors, or prior results suggest low status.
Daily Dosage Ranges: Maintenance vs. Correction
Vitamin D dosing often falls into two broad categories: maintenance and correction.
Maintenance commonly centers around 800–1,000 IU/day for seniors, though some clinicians recommend amounts slightly above this depending on dietary intake and sun exposure.
Correction typically involves higher doses, frequently 1,000–2,000 IU/day (and sometimes more under medical supervision) for a limited period. Correction aims to raise serum 25-hydroxyvitamin D—the main circulating marker—into a desirable range.
One important caution: high-dose therapy should not be improvised. Vitamin D can be stored, and excessive intake may increase the risk of hypercalcemia (too much calcium in the blood), which can lead to nausea, constipation, weakness, confusion, and in severe cases kidney problems.
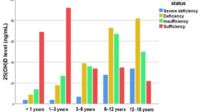
What Blood Levels Mean (And Why Testing Can Save You)
If dosage feels like guesswork, testing is the antidote. Clinicians usually measure 25-hydroxyvitamin D because it reflects overall vitamin D status more reliably than other forms.
Many healthcare teams aim for an adequate range that supports bone health and muscle function. When levels are low—especially when deficiency is confirmed—supplementation plans can be tailored with more precision. Testing also helps adjust the dose over time, avoiding both under-supplementation and overzealous dosing.
For seniors, testing can be particularly useful when there’s a history of falls, osteoporosis, fractures, kidney disease, malabsorption, or symptoms consistent with low vitamin D or calcium imbalance.
Vitamin D and Calcium: The Bone-Team Synergy
Vitamin D and calcium behave like co-stars. Vitamin D increases intestinal calcium absorption, while calcium provides the structural raw material for bone mineralization. Without adequate vitamin D, calcium intake may not be used as effectively.
Dietary calcium is still important. Seniors can often benefit from calcium sources such as dairy products, fortified plant milks, leafy greens, and calcium-set tofu. Yet many people struggle to reach their calcium targets through diet alone, and supplements may be considered.
When calcium and vitamin D are paired thoughtfully, bone remodeling can be supported and muscle function may improve—especially in people who are prone to weakness or reduced mobility.
Sunlight: The “Free” Source With Hidden Limitations
Sunlight sounds easy—until it isn’t. Seniors may spend more time indoors. Weather, latitude, season, and skin coverage all affect vitamin D production. Even with outdoor time, the amount of vitamin D generated can vary dramatically.
There’s also a balancing act. Too much sun increases skin cancer risk, and many seniors use sunscreen regularly. While sunscreen is a wise protective measure, it can reduce vitamin D synthesis.
In practice, many seniors treat sunlight as a bonus rather than a reliable strategy. Supplementation becomes the dependable backbone.

Choosing the Right Supplement Form: D2 vs. D3, and Practical Tips
Vitamin D comes in different forms, most notably D2 (ergocalciferol) and D3 (cholecalciferol). Many health professionals favor D3 for supplementation because it tends to be well utilized by the body.
Capsules, softgels, drops, and gummies exist, each with different convenience levels. For seniors, ease of use matters. A daily routine—after breakfast, with a main meal, or at a consistent time—can improve adherence.
Because vitamin D is fat-soluble, taking it with food that includes some fat may enhance absorption. That’s a small logistical detail, but it can make the dose work more efficiently.
Special Considerations: Weight, Medication, and Medical Conditions
Body weight can influence vitamin D status. People with higher body mass may require higher doses to reach and maintain adequate levels, since vitamin D can be sequestered in fatty tissue.
Medications matter, too. Long-term corticosteroid therapy can reduce vitamin D effectiveness and impair calcium balance. Some weight-loss medications and anti-seizure drugs can also alter vitamin D absorption or metabolism.
Kidney disease is another critical checkpoint. In such cases, vitamin D metabolism may change, and the active form may be needed rather than standard supplementation. This is not a “trial-and-error” situation.
If there’s a history of kidney stones or elevated calcium, dosing should be discussed with a clinician before increasing intake.
How to Decide Your Dosage: A Sensible, Safe Approach
Start by answering three questions: How much sunlight do you reliably get? How much vitamin D do you get from food? And what do your labs show, if you’ve tested?
For many seniors over 65, a reasonable starting point is 800 IU/day, especially when diet and sunlight are limited. If bloodwork confirms low levels—or risk factors are substantial—a clinician may recommend 1,000–2,000 IU/day for a period, followed by rechecking levels and adjusting.
Keep an eye on your overall strategy. Supplementing without addressing calcium intake, mobility, and fall prevention is like tightening a single bolt while ignoring the engine. Vitamin D works best as part of a comprehensive resilience plan.
Playful Reframing: Can a Small Dose Change a Big Outcome?
Here’s the twist: vitamin D isn’t dramatic in the moment. You don’t feel it like you might feel a quick burst of caffeine. But over months, adequacy can support muscle strength, help preserve bone integrity, and reduce the probability of deficiency-related decline.
So the question shifts again. Instead of “How much vitamin D should I take?” it becomes, “What does staying steady look like for my body?” A modest, consistent dose—guided by risk and possibly bloodwork—can be one of the quiet moves that keeps seniors stronger, steadier, and more confident.
When to Seek Medical Guidance (Don’t DIY These Situations)
Consider contacting a healthcare professional if there’s known kidney disease, history of hypercalcemia or kidney stones, malabsorption conditions, or if you’re currently on medications that interfere with vitamin D metabolism. Also seek guidance if you’ve had recent fractures, frequent falls, or unexplained muscle weakness.
And if you’re taking higher-than-usual doses, especially above 2,000 IU/day without monitoring, it’s wise to verify vitamin D and calcium levels. Safety is the unglamorous hero of longevity.
Practical Next Steps: A Simple Plan for Seniors Over 65
Take inventory: average sun exposure, diet sources (fortified milk, yogurt, fish), current supplements, and any relevant medical history. If vitamin D status is uncertain, ask about a 25-hydroxyvitamin D test. From there, dosing can be tailored rather than guessed.
Meanwhile, build a supportive routine: pair vitamin D with a meal, ensure calcium intake is adequate, and maintain gentle strength training or balance activities as recommended. Vitamin D can help your body do the work—movement helps your body use the support.
Small steps, consistently applied, can quietly shift outcomes. That’s the real magic of vitamin D for seniors—less spotlight, more substance.