It starts innocently—irritability that feels out of proportion, sudden fatigue that arrives like a weather front, a mood that flips with very little warning. You tell yourself you’re just stressed. Yet after the day ends, the emotional static remains. This is where a quiet possibility enters the conversation: a vitamin D deficiency. Not the kind of deficiency that only shows up on a lab report, but the kind that can subtly rewire how your brain regulates calm, motivation, and resilience.
When “Stress” Isn’t the Whole Story
Stress has a way of becoming the default explanation. It’s convenient, too. It gives a simple narrative: something happened, therefore you reacted. But mood is rarely single-cause. Sometimes the “stress” feeling is actually your nervous system sounding an alarm because its biochemical foundation is off.
Vitamin D is often discussed in terms of bones and sunshine, but its influence is wider. Receptors for vitamin D are present in many tissues, including areas involved in mood regulation. When vitamin D levels run low, the brain’s signaling landscape can become less stable. That instability can manifest as emotional lability—those rapid shifts from composed to overwhelmed that feel oddly disproportionate.
Here’s the perspective shift: you’re not merely enduring stress. You may be living with a shortage of the neurochemical scaffolding that helps your body respond to stress with steadier emotional timing.
Mood Swings and Emotional “Latency”
Think of mood regulation like a finely tuned instrument. You don’t notice it when it’s playing smoothly. But when it’s slightly out of tune, everything sounds “off.” Vitamin D deficiency may contribute to a delay—or miscalibration—in how quickly the body returns to equilibrium after stimulation.
Some people describe it as emotional latency: you react strongly, then it takes longer than it should to recover. Others notice a short fuse combined with a heavy aftertaste—sadness, agitation, or a drained sense of patience. These patterns can appear alongside other changes, such as sleep disruption or persistent tiredness.
Now curiosity takes the lead. Could a nutrient deficiency be the reason your internal thermostat overshoots?
Inflammation, the Brain, and the “Low-Grade Flame” Effect
One of the more intriguing mechanisms is the relationship between vitamin D status and inflammation. Inflammation doesn’t always arrive as an obvious fever. Often it’s a low-grade flame—quiet, persistent, and capable of affecting how you feel.
When inflammatory processes rise, the brain can interpret it as an ongoing stressor. That interpretation can alter neurotransmitter dynamics and influence how you experience energy, reward, and emotional clarity. The result can be a mood that feels both restless and heavy—like your mind is running on overdrive, but your spirit can’t fully ignite.
Short and sharp mood swings may be your body’s way of signaling: something isn’t balanced beneath the surface. Not dramatic enough to be dismissed as “just hormones,” but subtle enough to be overlooked as “just life.”
Serotonin: The Unexpected Bridge Between Sunlight and Feelings
People commonly hear about serotonin as the “happy chemical,” but the story is more nuanced. Serotonin participates in mood, sleep, appetite regulation, and emotional processing. Vitamin D appears to interact with pathways connected to serotonin function, and insufficient vitamin D may contribute to reduced effectiveness of these mood-supporting systems.
When serotonin-related pathways wobble, symptoms can look like irritability, low motivation, and emotional heaviness. Sometimes it’s not sadness in the classic sense. It’s more like a muted spectrum—everything feels dull, and your reactions feel too intense for the moment.
Here’s the thought-provoking angle: your mood might not be “broken.” It might be under-supported.
Energy, Motivation, and the Link to Emotional Volatility
Mood swings rarely appear alone. They often arrive alongside energy changes that make emotional control harder. Vitamin D deficiency is frequently associated with fatigue, reduced vitality, and a sense that tasks require more effort than they used to.
When your energy reserves feel depleted, your emotional system becomes less forgiving. Imagine trying to navigate a busy day with low fuel. Small frustrations become large events. Delays feel personal. Silence feels sharper. This doesn’t mean you’re exaggerating—it means your nervous system has less capacity to regulate.
Long sentence, short summary: low vitamin D may create a double burden—less energy and less emotional buffering.
Sleep Disruption: The Nighttime Domino
Sleep influences everything: mood stability, cognitive control, stress tolerance, and even how quickly your body recovers from emotional challenges. If vitamin D deficiency is present, sleep can become less restorative. You may fall asleep, but you don’t truly sink into recovery.
The next day follows with cognitive fog and heightened reactivity. Even a minor comment can feel like a gust of wind that knocks you off balance. Over time, inconsistent sleep can intensify mood swings into a cycle—sleep suffers, emotional regulation weakens, stress perception grows.
Curiosity can be protective here. Instead of only asking, “Why am I so moody?” ask, “What’s my body doing at night that might be shaping my emotions by morning?”
Common Clues That Often Travel With Low Vitamin D
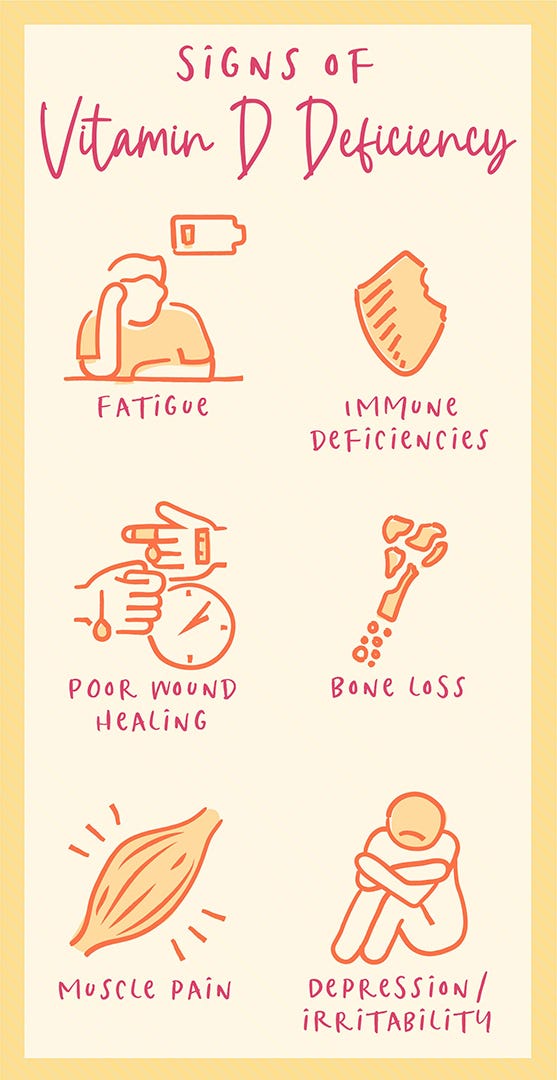
Vitamin D deficiency is notorious for being stealthy. It can show up as a constellation of clues rather than one dramatic symptom. Some people experience muscle weakness or aches, recurring feelings of tiredness, and low resilience. Others notice changes in mood, concentration, or overall mental steadiness.
Because these symptoms overlap with many other conditions, the best approach is pattern recognition. Are your mood shifts paired with fatigue? Do you feel emotionally “frayed” alongside physical low-grade discomfort? Is there a seasonal trend—worse in winter, improved after sunlight exposure?
To sharpen the lens, consider how often your emotional state tracks with your sunlight, diet, and daily routines.
Risk Factors: Who Might Be Most Susceptible
Certain lifestyles and circumstances increase the likelihood of low vitamin D. Limited sun exposure is an obvious one, but there are others that deserve attention: darker skin pigmentation, older age, living far from the equator, frequent use of sunscreen without compensatory dietary intake, and time spent indoors.
Diet can also play a role. If your intake of vitamin D-rich foods is minimal, deficiency becomes more plausible. Additionally, some medical conditions affect absorption, making “eating enough” insufficient.
The curiosity move: instead of asking whether you personally “should” have low vitamin D, ask whether your environment makes it harder to maintain healthy levels.
Testing and Interpretation: Turning Fog Into Clarity
Here is where many people get stuck: they try to guess. Guessing can be emotionally exhausting—especially when mood is involved. A more grounded approach is to seek testing and interpret results with a clinician.
Lab testing helps convert uncertainty into data. Then the conversation shifts from speculation to strategy. It’s not about chasing a single culprit. It’s about checking whether vitamin D insufficiency could be part of your mood landscape.
Even if low vitamin D isn’t the only factor, knowing its status can reduce the sense of helplessness. Clarity breeds control.
What “Addressing It” Can Look Like
If vitamin D deficiency is identified, the path forward often includes supplementation and lifestyle adjustments—usually paired with dietary changes and more safe sunlight exposure when feasible. The goal is not to chase extremes. It’s to restore steadiness.
Consistency matters. Your body doesn’t flip mood chemistry like a switch. Improvements, when they occur, tend to be gradual, intertwined with better sleep, improved energy, and a more stable emotional baseline.
Short thought to keep in mind: correcting a deficiency can feel like rebuilding a thermostat rather than forcing a mood.

A Sustainable Perspective: Mood Stability as a System
When mood swings feel random, it’s tempting to treat them like personal failure. But emotional regulation is systemic. It involves neurotransmitters, inflammation balance, sleep architecture, energy availability, and stress response calibration. Vitamin D sits near several of these systems.
So the promise—quiet but real—is a shift in perspective. Instead of only asking, “What’s wrong with me?” consider, “What might my body be signaling?” This question invites investigation rather than self-judgment.
If mood swings have been persistent, consider a holistic evaluation. Check vitamin D status. Review sleep quality. Explore stress patterns. Then assemble a plan that supports both physiology and psychology.
Your next emotional chapter doesn’t have to be defined by volatility. With clarity and consistency, you may find your baseline moving toward calm—one steady step at a time.
:max_bytes(150000):strip_icc()/VWH-JulieBang-VitaminDDeficiency-txt-4000x2700-25d3aac6e3914cf98d08db2ba4d87be2.png)