Picture vitamin D as a quiet architect. Each day, it sketches instructions for bones, immune signaling, and cellular rhythm—yet many people don’t realize the blueprint is incomplete until a blood test turns the invisible into measurable numbers. In the US, the question often isn’t “Do I need it?” but “What will it cost?”—especially when insurance enters the room like a gatekeeper with a complicated keyring. Whether you’re navigating the labyrinth of billing codes or weighing the convenience of home testing, understanding vitamin D blood test cost can feel like finding a compass before the fog rolls in.
Why Vitamin D Testing Can Feel Like Turning On a Light
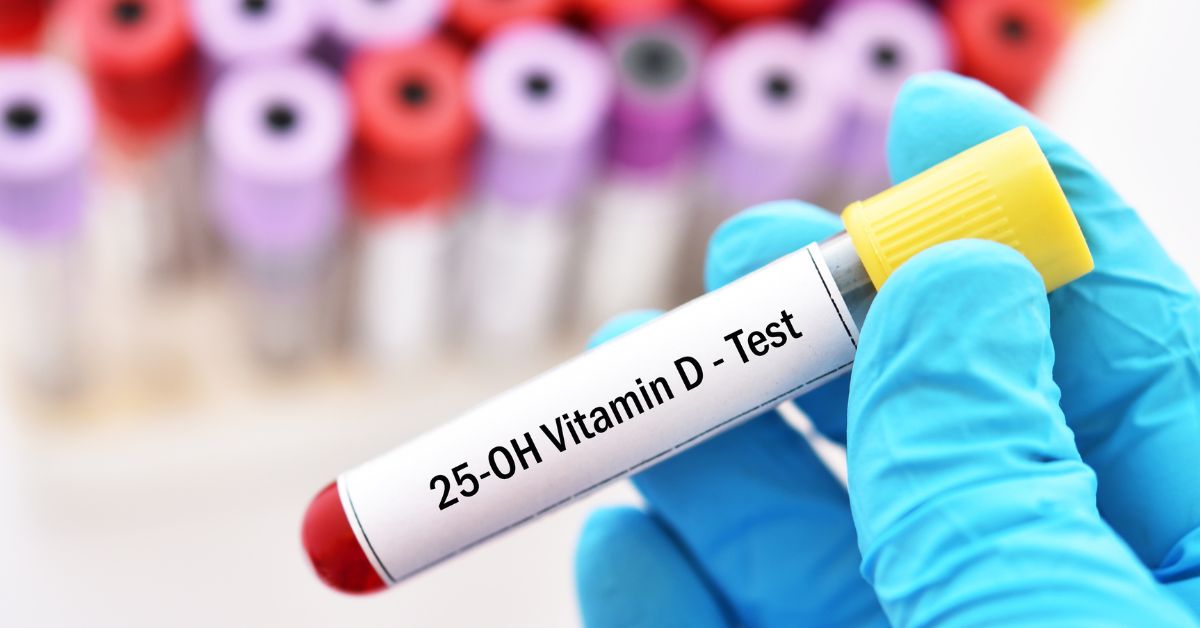
Vitamin D testing, typically measured as 25-hydroxyvitamin D (25(OH)D), is less about fashioning a guess and more about verifying physiology. It answers the question: is your body running on adequate stores, cruising on borderline supply, or operating in a low-battery state?
Cost depends on the setting—clinic draw, lab services, or a home kit—and also on the administrative choreography between provider, laboratory, and insurer. The price tag may be visible on some receipts, but the true cost often hides in the fine print: deductible status, copays, coinsurance, and whether the test is coded as routine, diagnostic, or part of a broader panel.
Some people seek testing because they’ve had fatigue, muscle aches, or minimal sun exposure. Others are nudged by risk factors such as darker skin tone, older age, malabsorption conditions, obesity, certain medications, or pregnancy. In these cases, testing can be an efficient detour from guesswork.
Typical Vitamin D Blood Test Costs in the US (No Insurance)
Without insurance, vitamin D testing can range from moderately accessible to surprisingly steep, depending on where the blood draw occurs and how the lab prices its analysis. When you pay out of pocket, you may encounter two separate components: the collection fee (for the blood draw) and the lab fee (for the measurement and reporting).
In many settings, the “all-in” price structure can look different from one provider to another. A standalone laboratory might list an itemized rate. A clinic may bundle collection with processing and reporting. Meanwhile, home testing can shift the economics—sometimes lowering the barrier to entry, sometimes increasing it through kit pricing and shipping.
Consider this a spectrum: on one end are concise lab-direct options; on the other are convenience-forward clinical visits with higher overhead. Either way, the key is to compare the final figure, not only the headline number.
What “With Insurance” Really Means for Your Final Bill
Insurance can reduce your out-of-pocket cost, but it rarely erases it entirely. The amount you pay usually hinges on whether the test is considered medically necessary and how your plan structures benefits.
Many US plans treat lab services differently than office visits. You might owe a copay for the visit, but coinsurance for the lab portion. Or, if you haven’t met your deductible, you might pay the contracted rate until the deductible threshold is reached.
In practical terms, “with insurance” often means you pay a smaller portion of a negotiated price. That negotiated price is typically lower than the sticker price you’d see without coverage. Still, the difference between “allowed amount” and “patient responsibility” can be hard to forecast without verifying benefits.
If your clinician orders testing due to symptoms, risk factors, or abnormal prior results, insurers are more likely to treat it as diagnostic rather than purely routine. That framing can influence coverage decisions.
Deductibles, Copays, Coinsurance: The Billing Triad
Think of your deductible, copay, and coinsurance as three gears in a billing machine. If your deductible is still intact, you may feel the full initial cost. Once you’ve met it, the gears shift and your share may become a flatter copay or a smaller coinsurance percentage.
Here’s the important nuance: vitamin D testing can happen within a larger visit ecosystem. You might have an appointment where a clinician orders labs; you might also have an office charge even if the test itself is billed separately. The office visit fee can sometimes be the “unexpected” portion that makes your final bill feel larger than anticipated.
Ask for two numbers when possible: the provider or lab’s estimated charge and the insured allowed amount (or a benefit estimate). It’s like checking both the weather forecast and the storm warning, rather than trusting only one.
Clinic Draw vs. Lab Direct vs. Home Kits: Cost in Different Outfits
Choosing a testing route is like choosing a travel mode. You can take the scheduled comfort of a clinic draw, go direct with lab services, or opt for the compact independence of a home kit.
Clinic draw: Often involves a visit, collection by a professional, and lab processing. It can be convenient if you want clinician support or if your test is tied to a broader evaluation.
Lab direct: You may schedule a blood draw at a collection site, then the lab processes the results. This can sometimes streamline pricing, especially if you focus on the test itself.
Home kits: You receive the kit, perform collection (often via fingerstick or guided method), and send it to the lab. Costs can be competitive, and the appeal is speed, privacy, and scheduling flexibility. However, it’s essential to confirm test accuracy standards, lab reporting practices, and whether the results integrate smoothly with your clinician’s plan.
When comparing, evaluate not only the price but also the reporting format: reference ranges, interpretation notes, and whether the results are presented in a way your doctor can quickly use.

How to Estimate Your Out-of-Pocket Cost Before You Pay
Before committing, treat cost estimation like risk management. Start by asking your provider which test they ordered (25(OH)D) and whether any related tests are bundled. Then call your insurance and request a benefits estimate. Many insurers can provide the expected copay or coinsurance once they know the lab and procedure code.
Next, ask the collection site or lab for an estimate, especially if paying without insurance. Request itemization—collection fee, lab fee, and shipping or handling where applicable. Short questions can prevent long surprises.
If you’re comparing home versus in-clinic options, ask whether the lab that processes the kit is accredited and what turnaround time is offered. Time can change value. A faster result can help you adjust supplementation sooner, which can be practical if you’re addressing deficiency risks.
Additional Costs to Consider: Appointments, Follow-Ups, and Panels
The vitamin D test itself may be only part of the fiscal story. If your provider reviews results and adjusts supplementation, there may be an office follow-up. Sometimes vitamin D testing is paired with other labs such as calcium, parathyroid hormone, or magnesium—especially when symptoms or complex risk factors exist.
Even without those add-ons, repeated testing can occur. Many clinicians recheck levels after a supplementation plan to verify response. That follow-up can be financially significant if done out of pocket.
Think of it like measuring a thermostat. One test tells you the current temperature. Rechecking tells you whether the adjustment worked. If you’re paying multiple times, your total cost becomes the headline number, not just the first result.

When Vitamin D Testing Is Most Likely Worth the Cost
Testing tends to be most compelling when it clarifies a decision—start supplementation, adjust dosage, investigate malabsorption, or evaluate persistent symptoms. It’s also useful if you’ve already been taking vitamin D and want to avoid both underdosing and excessive dosing.
Consider testing if you experience muscle weakness, bone discomfort, frequent falls, chronic fatigue, unexplained low energy, or if you’re in a group with higher deficiency risk. If you have conditions affecting absorption—such as celiac disease, inflammatory bowel disease, bariatric surgery history, or chronic kidney issues—testing becomes a more direct bridge between treatment and evidence.
In these scenarios, cost is not merely expense. It’s information that can redirect care.
How to Choose the Best Option for Your Budget
If you’re uninsured, you’ll likely prioritize the lowest total price with acceptable turnaround and reporting quality. Look for clear itemization and transparent lab processing. If you’re insured, prioritize understanding your deductible status and whether the test is considered diagnostic.
A surprisingly effective approach is to request a short pre-check: the expected patient responsibility for the lab and any associated visit. Even brief verification can reduce uncertainty.
Ultimately, the best choice is the one that fits your circumstances—your risk profile, urgency, and ability to integrate results with a clinician’s plan.

Final Takeaway: Costs Vary, Clarity Doesn’t Have to
Vitamin D blood test cost in the US isn’t a single number—it’s a dynamic equation influenced by insurance status, deductible progress, clinic overhead, and whether you choose home collection or in-person draw. But the fog isn’t unavoidable. With the right questions and a clear comparison of total out-of-pocket responsibility, you can turn billing uncertainty into a measurable decision.
In the end, vitamin D testing is about more than lab results. It’s about restoring momentum—letting your body run its chemical orchestra with the right volume. And when you know what you’re paying, you can focus on what matters: building a plan that actually moves.