It sounds counterintuitive at first: vitamin D—the so‑called sunshine vitamin—helps orchestrate immunity, bones, and cellular signaling. Yet in rare circumstances, an overload can become a medical plot twist. High-dose D is not a common cause of pancreatitis, but the possibility is real enough to warrant curiosity. Not fear—curiosity. The kind that asks what mechanisms could connect calcium metabolism, oxidative stress, and pancreatic inflammation, and how quickly subtle signals can escalate into something serious.
First, the premise: what “high-dose D” actually means
Vitamin D is fat-soluble, meaning it doesn’t behave like many water-soluble compounds that pass through the body and leave swiftly. Instead, it can accumulate. In most people, supplementation at sensible doses is well tolerated. But when dosing becomes excessive—whether through high-dose prescriptions, aggressive self-supplementation, or prolonged use without laboratory monitoring—serum calcium can climb.
This is the fulcrum of the story. Pancreatitis is not typically triggered by vitamin D directly; rather, it’s often the downstream biochemical commotion—hypercalcemia—that sets the stage. Hypercalcemia can be dramatic in the body’s chemistry. It influences nerve impulses, muscle contraction, kidney handling, and endocrine signaling. And the pancreas, being a tightly regulated organ, is vulnerable to metabolic turbulence.
The biochemical bridge: vitamin D, calcium, and pancreatic inflammation
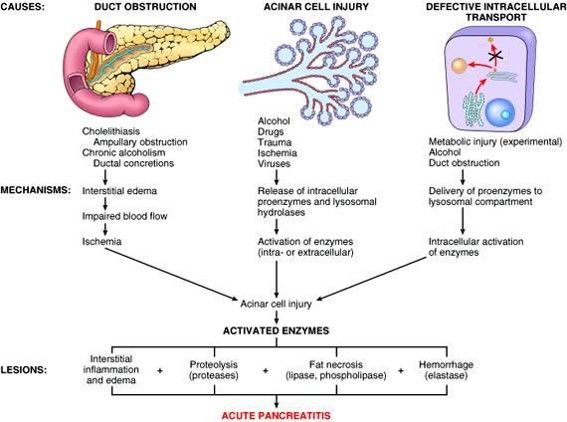
Vitamin D increases intestinal absorption of calcium and phosphate. Under ordinary circumstances, the body compensates with regulatory hormones. Under extreme intake, compensation can lag behind the surge. Calcium rises. When calcium becomes persistently elevated, pancreatic cells can experience stress—leading to premature activation of digestive enzymes inside the pancreas. Think of it as a controlled demolition system that accidentally flips early, detonating internally instead of in the gut.
Enzyme misfiring is one plausible pathway, but not the only one. High calcium can disrupt intracellular signaling and promote inflammatory cascades. It can also affect microcirculation, potentially contributing to ischemic strain. The result can look like classic acute pancreatitis: epigastric pain, nausea, vomiting, elevated pancreatic enzymes, and imaging changes in some cases.
In rare reports, the timing is striking: symptoms emerge after sustained high-dose exposure or after a sharp increase in intake. The body, in those moments, resembles a thermostat that can’t understand the meaning of “too much.”
Hypercalcemia: the clinical fingerprint that changes everything
If vitamin D excess is the match, hypercalcemia is the flame that catches quickly. Clinically, hypercalcemia can produce symptoms that might initially seem unrelated—constipation, dehydration, fatigue, confusion, excessive thirst and urination. Those symptoms can obscure the pancreas at first, especially when abdominal pain is mistaken for “indigestion” or “stomach irritation.”
When pancreatitis occurs in the context of high calcium, clinicians often look for the calcium signal as a clue. This matters because treatment priorities shift. You don’t only treat the pancreatitis. You also correct the metabolic imbalance that helped spark it. That means addressing calcium levels promptly and reassessing the vitamin D strategy.
In this sense, the “link” is not a casual association; it’s a mechanistic relay—vitamin D elevates calcium, calcium destabilizes pancreatic physiology, and inflammation follows.
Rarity, but not insignificance: why this happens so rarely
Most people never approach the serum vitamin D levels associated with toxicity. Even when someone takes supplements, many doses are modest and nutrition varies. Moreover, the body has buffers—binding proteins, metabolic conversion pathways, and renal excretion mechanisms. These buffers are not infinite, though. Exceed them and the chemistry can overshoot.
Risk increases when certain factors stack together: preexisting disorders affecting calcium metabolism, reduced kidney function, concurrent use of medications that raise calcium, or conditions that increase sensitivity to calcium. Genetic differences can also affect how individuals process vitamin D. There are people whose physiology behaves like a well-tuned instrument; and others whose same vitamin D dose becomes a siren song.
That’s why the connection is described as rare but serious. Rare doesn’t mean negligible. It means vigilance matters—especially when dosage decisions are made without lab support.
How pancreatitis presents when the cause is metabolic
Acute pancreatitis is often recognizable, but the context can blur the edges. Classic pain is typically severe and localized to the upper abdomen, often radiating to the back. Nausea and vomiting frequently arrive like an echo. But if hypercalcemia is present, dehydration and neurologic symptoms can complicate the picture. People may feel “washed out” before the pain becomes undeniable.
Laboratory findings commonly include elevated pancreatic enzymes—amylase and lipase. Imaging may confirm inflammation. If hypercalcemia is part of the narrative, calcium levels may be conspicuously high, sometimes alongside evidence of kidney stress.
The practical lesson is psychological: symptoms don’t always announce their origin in a straightforward way. Metabolic causes can disguise themselves behind general malaise.
Risk factors that quietly amplify the effect
High-dose D becomes more dangerous when multiple risk factors converge. Chronic kidney disease reduces calcium clearance. Malabsorption or fat absorption disorders can cause unpredictability in dosing. Some endocrine conditions heighten baseline calcium. Certain medications—particularly those that influence calcium balance—can create synergy. Even adherence behaviors matter; an “accidental” high dose maintained for weeks can be more consequential than a one-time overshoot.
Another underappreciated factor is the difference between “recommended” supplementation and “therapeutic megadoses.” The latter may be medically appropriate for select deficiencies under supervision, but it requires deliberate monitoring. Vitamin D toxicity is less about intention and more about exposure plus time.
When the body’s margin of error narrows, a dose that seems harmless on paper can become hazardous in practice.
Diagnosis: connecting the dots without tunnel vision
When pancreatitis appears, clinicians typically evaluate the common culprits first—gallstones, alcohol use, triglyceride elevations, certain medications, infections, and structural issues. But metabolic causes are part of the differential diagnosis. If the timeline includes high-dose vitamin D and calcium levels are elevated, the narrative becomes clearer.
Lab work is the investigative flashlight. Measuring serum calcium, vitamin D levels, renal function, and markers of pancreatic injury can help determine whether the vitamin D-calcim pathway is involved. Imaging—ultrasound, CT, or MRI—may assess severity and complications. The goal is not to assign blame prematurely. It is to identify the mechanism so the treatment is targeted.
In rare pancreatitis cases, this step prevents a harmful loop—stopping the pancreas from inflaming while simultaneously correcting the biochemical imbalance that triggered the cascade.
Treatment principles: stabilize, correct calcium, and reassess supplementation
Treatment for acute pancreatitis often begins with supportive care: pain control, hydration, and close monitoring. But when hypercalcemia is present, calcium correction becomes a parallel priority. Clinicians may use strategies to lower calcium levels and address dehydration and electrolyte disruptions. If vitamin D excess is implicated, it is generally halted. Reintroduction—if ever considered—should be cautious, data-driven, and tailored.
Some cases improve quickly once calcium levels normalize and inflammation settles. Others may be more complicated, especially if kidney function is affected or if the pancreatitis is severe. That’s why early recognition is valuable. The earlier the metabolic trigger is identified, the easier it is to interrupt the chain reaction.
Prevention: the quiet art of dosing with boundaries
The most effective prevention is not dramatic. It is careful. If vitamin D is being supplemented, dose selection should match individual risk, baseline levels, and clinical context. Laboratory monitoring turns uncertainty into clarity. It prevents the slow drift toward excess—what resembles “more is better,” but is actually “more is risk.”
For people using high-dose regimens, the question shouldn’t be only “How do I feel?” The better question is “What is happening in the numbers?” Serum 25-hydroxyvitamin D and calcium can reveal whether the body is in safe territory.
Equally important: avoid stacking multiple products—over-the-counter vitamin D, fortified foods, and prescription or high-dose therapy—without accounting for total intake. The body doesn’t care whether the vitamin D came from a pill, a drop, or a capsule. It cares about cumulative exposure.
When to seek urgent care: warning signs that shouldn’t be ignored
If someone develops severe upper abdominal pain with vomiting, it warrants prompt medical evaluation. If that person also has symptoms consistent with hypercalcemia—marked thirst, confusion, constipation, profound weakness—urgency increases. Dehydration can worsen quickly, and metabolic disturbances can escalate.
It’s not about panic. It’s about speed. Pancreatitis can progress over hours, and hypercalcemia can destabilize the body’s normal balance. Getting evaluation early gives clinicians the opportunity to intervene before inflammation intensifies.
Looking at the bigger picture: how perspective changes outcomes
The most useful perspective shift is this: vitamin D is powerful, not magical. When it stays within a physiologic range, it supports orderly biology. When it is pushed beyond safe boundaries, it can indirectly ignite harm—most notably through hypercalcemia in rare scenarios. The link between high-dose D and pancreatitis is uncommon, but it’s instructive because it highlights how endocrine and metabolic systems can collide with digestive organs.
Curiosity, then, becomes protection. It encourages monitoring, dosing humility, and timely recognition of symptoms. And it turns a rare medical possibility into a practical mindset: supplement thoughtfully, measure responsibly, and treat the body’s chemistry as a living system with limits.