There’s a quiet pattern many people recognize without being able to name it: persistent fatigue that refuses to fully lift, restless nights, and a sense that the body is “working harder” than it should. It’s easy to blame modern life—stress, late schedules, inconsistent meals. Yet beneath the familiar noise, there may be a more specific culprit: magnesium. Not as a trendy supplement, but as a foundational mineral the body uses for hundreds of biochemical reactions, including the activation of vitamin D. And that’s where the hidden epidemic begins—because when magnesium is chronically insufficient, the vitamin D you might be absorbing (or even supplementing) can become functionally underutilized.
Magnesium: the overlooked conductor of cellular chemistry
Magnesium is often treated like an afterthought. People search for answers in single vitamins or quick fixes, but magnesium operates more like a conductor than a soloist. It helps regulate nerve impulses, muscle relaxation, energy metabolism, and electrolyte balance. It also influences enzyme activity across the day-to-day molecular orchestra of the body.
When magnesium is low, the system doesn’t always announce itself with dramatic symptoms. Instead, it behaves like a subtle underclocking: the body still runs, but with diminished efficiency. Sleep can become lighter. Recovery may feel incomplete. Mood and concentration can wobble. Some individuals describe it as a persistent background hum—never catastrophic, yet impossible to ignore.
The 80% reality: deficiency as a pervasive, unglamorous problem
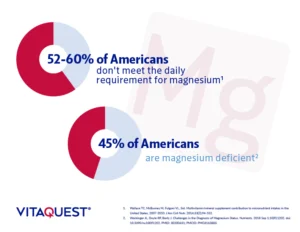
“80% of Americans lack magnesium for adequate D activation” isn’t simply a statistic; it’s a cultural mirror. Magnesium inadequacy doesn’t usually arrive with a single cause. It accumulates through everyday choices and systemic habits: diets that skew low in magnesium-rich foods, refined grains that replace whole sources, and meals that are convenient rather than nutritionally dense.
Then there’s the modern metabolism problem. Many people are more sedentary than they realize, consume higher amounts of processed foods, and experience chronic stress. Stress doesn’t merely feel emotional. It changes physiology—often increasing magnesium utilization and altering how the body handles minerals.
The result is a widespread pattern of insufficient magnesium status. Not everyone will feel symptoms immediately, but the biochemical consequences can still unfold quietly. And one of the most important—often missed—is vitamin D activation.
Vitamin D isn’t enough: why “having D” doesn’t guarantee “using D”
Vitamin D has a reputation for being empowering. People understand that sunlight and supplementation can raise vitamin D levels. But the story rarely ends with measurement. Vitamin D must be converted and activated in a stepwise process, and magnesium is involved along that pathway.
Imagine vitamin D as an unfinished letter that can’t be properly delivered. The message might exist—present in the bloodstream—but the final steps require specific molecular “keys.” Magnesium helps provide those keys. Without it, the conversion and functional availability of vitamin D can be impaired, leaving cells without adequate signaling.
This is why some individuals can have decent vitamin D lab numbers yet still feel the downstream effects of deficiency: low vitality, occasional aches, and an immune resilience that doesn’t feel robust.
Why magnesium deficiency hides in plain sight
Magnesium depletion can be disguised by overlapping symptoms. Fatigue, muscle tension, headaches, and sleep disruption are common complaints. They can also be blamed on stress, caffeine, poor sleep hygiene, or screen exposure. Even clinicians can chase patterns that are real but not causal.
In practice, magnesium deficiency is often a “background condition.” It may intensify other issues—like dysregulated glucose handling or heightened inflammatory tone—making it harder to isolate. Short-term adjustments might help temporarily, but if magnesium remains low, the body keeps returning to the same friction points.
Another stealth factor is that magnesium is not always measured in routine screenings. Blood magnesium can look normal even when intracellular stores are low. So the absence of alarms on a lab report doesn’t always mean the problem isn’t there.
Common observations that point to a deeper mineral imbalance
You don’t need to be a medical detective to suspect magnesium inadequacy. There are patterns many people recognize: frequent nighttime awakenings, tight calves or jaw tension, irregular energy dips that don’t match food timing, and a tendency to feel “wired but tired.”
Some people notice that dietary attempts—more greens, more water—improve things but don’t fully resolve them. Others find that supplementation helps, but only when magnesium is paired with consistent sleep and adequate nutrition.
These experiences hint at a deeper mechanism: magnesium supports relaxation pathways and energy production. When it’s scarce, the body may struggle to switch into recovery mode. That can create the sensation that even rest doesn’t feel restorative.
Deeper reasons for fascination: magnesium’s web of interactions
Magnesium is rarely a lone actor. It interfaces with vitamin D, calcium balance, potassium handling, and nervous system regulation. It also participates in cellular energy transactions through ATP stabilization—meaning it’s tied to the body’s ability to convert nutrients into usable power.
This interconnectedness can be fascinating and frustrating at the same time. It suggests that magnesium deficiency may not be a single “missing nutrient” problem, but a systems issue: how your diet, stress load, digestive environment, and mineral transport mechanisms converge.
That’s why some people experience improvements that seem broader than expected. When magnesium supports D activation and cellular signaling, downstream processes—immunity modulation, muscle function, and mood stability—can appear to shift together.
Hidden dietary corridors: where magnesium quietly disappears
Magnesium is abundant in certain foods: leafy greens, legumes, nuts, seeds, and whole grains. Yet many modern eating patterns don’t consistently include these in meaningful quantities. Refined grains, sugary snacks, and a diet heavy on convenience meals can crowd out magnesium-rich options.
Portion size matters. Even people who “eat healthy” sometimes underestimate magnesium-dense servings. A handful of nuts here, a side of spinach there, but not enough to rebuild stores if depletion has been long-standing.
Cooking methods and food choices also influence mineral retention. Some preparation styles can reduce mineral availability, while overly processed foods contribute less magnesium and more inhibitors to overall balance.
Physiology under stress: why the body can consume magnesium faster
Stress is not only psychological; it’s biochemical. During chronic stress, cortisol signaling and sympathetic activation can affect mineral turnover. Physical exertion, especially endurance training without sufficient recovery nutrition, can also increase magnesium needs.
Caffeine and alcohol may further complicate the landscape by influencing mineral excretion and sleep quality. Poor sleep, in turn, can worsen metabolic efficiency—creating a feedback loop that leaves the body more vulnerable to inadequate micronutrients.
In this way, magnesium deficiency becomes a narrative of modern life: demanding schedules, overstimulation, and nutrition that often fails to keep pace with physiological demand.
Signs to watch: subtle cues that deserve attention
Not every magnesium deficit presents identically. But common cues include muscle cramps, twitching, persistent tension, and frequent “low-grade” exhaustion. Sleep disturbances—especially difficulty staying asleep—can be a clue.
Some individuals report migraines, constipation, or restless legs. Others experience a kind of mental fog that feels out of proportion to their workload. If these patterns cluster, magnesium adequacy becomes worth considering, particularly in the context of vitamin D.
While symptoms are not diagnostic, they are directional. The deeper question is: are you building the mineral substrate your body requires for activation and utilization?
How to think about supplementation and “D activation” support
If magnesium is implicated in D activation, then a sensible approach is to address magnesium adequacy rather than treating vitamin D as a standalone solution. Supplement forms vary in absorption and tolerability, so it’s often wise to choose a formulation that aligns with individual digestion and comfort.
Consistency matters. Magnesium is not a one-day rescue mineral. The goal is to support sustained physiological availability so that vitamin D processes can proceed efficiently.
It’s also smart to consider that magnesium works best in a broader plan: balanced meals, adequate hydration, and sleep rhythms that help the body shift from activation into repair.
When testing helps: clarity without false comfort
Some people benefit from lab work, especially if symptoms persist. Yet understanding magnesium testing is important. Blood magnesium can be misleadingly normal. Still, vitamin D measurements can be a helpful starting point—particularly when interpreted alongside diet quality, symptom patterns, and overall mineral balance.
If vitamin D appears adequate but symptoms linger, that disconnect can be a signal to look for supporting cofactors, including magnesium. This is where biochemical logic becomes practical: activation and utilization are not guaranteed by a number alone.
The takeaway: treat magnesium as the ignition key
Magnesium deficiency is not a dramatic headline; it’s a slow-moving shift in the body’s capacity. When magnesium stores are low, vitamin D may not activate properly, leaving tissues without the signaling they need. The “hidden epidemic” isn’t just about low mineral levels. It’s about lost coordination—an unglamorous breakdown in the body’s ability to translate inputs into outcomes.
If fatigue, sleep disruption, or low resilience feel familiar, consider the possibility that you’re not missing vitamin D alone. You might be missing the ignition key that helps your body use it. Restoring magnesium adequacy can be a strategic, foundational step—one that supports both mineral harmony and the deeper biochemical choreography behind vitality.