Weight loss medications can feel like a quiet lever inside the body—subtle at first, then unmistakable. Ozempic and Wegovy (both in the GLP-1 family) often reshape appetite, slow gastric passage, and encourage steadier energy decisions. Yet even the most brilliant “machine” needs the right fuel and scaffolding. Vitamin D is one of those scaffolds—often overlooked—more like the anchor-stone than the headline. For women navigating weight loss drugs, ensuring adequate vitamin D can support bones, mood, immunity, and overall momentum. Think of it as the sun’s backstage crew: unseen, indispensable, and deeply influential when the spotlight is on weight change.
Why Vitamin D Matters During Weight Loss Drug Therapy
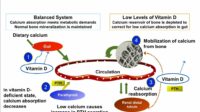
Vitamin D is not merely a vitamin. It is a hormone-like regulator that guides calcium absorption, helps bone mineralization, and interacts with immune signaling. When weight loss is deliberate—sometimes rapid—your body may draw on stored reserves to maintain function. If vitamin D levels are insufficient, the “calcium choreography” can stumble: less efficient absorption in the gut, more strain on bones, and a greater likelihood of lingering fatigue.
On GLP-1-based therapies, many women notice changes in food intake. Less intake can unintentionally reduce dietary vitamin D and calcium sources, especially if appetite suppression limits dairy, fortified foods, or fatty fish. The result can be a subtle mismatch: the medication shifts hunger and intake, but vitamin needs do not automatically adjust in perfect synchrony. Vitamin D becomes a balancing act—one that can be managed, monitored, and optimized.
Ozempic vs. Wegovy: Does Vitamin D Need to Change?
Ozempic and Wegovy share a family resemblance, but their dosing contexts differ. Regardless of which GLP-1 medication is used, the downstream realities for many women can be similar: appetite modulation, altered meal patterns, and potential reduction in intake of certain micronutrient sources.
Vitamin D strategy is therefore less about the brand name and more about your biology and habits. Your baseline vitamin D level matters. Your exposure to sunlight matters. Your dietary pattern matters. Your muscle mass, activity level, and bone health history matter. In short: the need for vitamin D is less “medication-specific” and more “life-specific,” because the body’s demand is shaped by more than the prescription alone.
The Bone & Muscle Connection: A Hidden Plotline
Weight loss medications can help many women lose fat while preserving lean tissue—especially when paired with protein intake and strength training. Still, the body’s structural system is busy. Bones are living architecture: they remodel continuously, and vitamin D supports the mineral deposition needed to keep that structure resilient.
If vitamin D is low, you may feel it indirectly: aches that seem nonspecific, a reluctance to bounce back after exercise, or a persistent sense of low-grade fatigue. Those symptoms are not diagnostic on their own, but they can be clues—like fingerprints at a scene.
Muscles also rely on vitamin D-related pathways for proper function. Adequate levels may support strength, balance, and neuromuscular coordination—quiet capabilities that matter when you’re building a routine around workouts, walking goals, or physical therapy movements.
Testing Like a Detective: What to Check and Why
Instead of guessing, consider testing—because vitamin D is one of those nutrients where “feeling fine” does not always mean “status optimal.” The most useful lab is typically 25-hydroxyvitamin D, often written as 25(OH)D. This reflects vitamin D stored in the body and correlates better with vitamin D status than shorter-lived measures.
Many women on weight loss drugs may not think to test unless symptoms appear. But prevention is a smarter narrative. A baseline measurement can guide dosing decisions, track changes over time, and reduce the odds of both deficiency and unnecessary excess.
While interpreting results, it helps to remember that “optimal” can vary by individual circumstances. Seasonal factors influence levels. Skin tone influences synthesis. Geographic latitude influences sunlight availability. Lifestyle influences exposure. Your lab value is one chapter, not the entire book.
Dietary Sources: The Small Choices That Accumulate
Dietary vitamin D can be a steady companion to supplementation. Fortified foods—such as certain dairy products, plant milks, and breakfast cereals—often provide meaningful amounts. Fatty fish (salmon, sardines, mackerel) can be rich sources. Egg yolks contribute too, though usually in smaller quantities.
GLP-1 therapy can reshape appetite, making it harder to consistently eat foods that require planning. But there’s a workaround: build “low-friction vitamin D options” into meals. Think of vitamin D as a seasoning that should remain easy to add even when appetite is unpredictable. A fortified yogurt, a glass of fortified milk alternative, a canned salmon salad, or a nutrient-minded breakfast can turn vitamin D from a sporadic event into a daily ritual.
Supplementation: How to Consider Dose, Timing, and Safety
For many women, supplementation becomes the practical route—especially in seasons with limited sunlight. Vitamin D is fat-soluble, meaning it’s often absorbed better when taken with a meal that contains some fat. Many people tolerate it well, and it’s available in common forms such as vitamin D3 (cholecalciferol) and vitamin D2 (ergocalciferol). D3 is frequently used in everyday supplementation.
But “more” isn’t automatically “better.” Too much vitamin D over time can raise calcium levels and trigger complications. That’s why dosing should ideally be guided by testing and clinician input, particularly if you have a history of kidney stones, sarcoidosis, hyperparathyroidism, or other conditions affecting calcium metabolism.
Timing can also matter. Some women prefer taking vitamin D in the morning with breakfast; others choose evening. The best schedule is the one that aligns with your routine—because consistency turns supplementing into a rhythm rather than a reminder.
Vitamin D and Calcium: The Duo That Works in Tandem
Vitamin D and calcium often travel as a pair. Vitamin D helps your body absorb calcium efficiently; calcium supports bone strength and mineralization. If vitamin D improves but calcium intake remains low, you may not realize the full benefit. Conversely, adequate calcium without vitamin D may also limit absorption.
For women on weight loss drugs, appetite changes can alter calcium intake. It’s common to reduce portions of dairy or skip calcium-rich snacks. That’s why it helps to evaluate both nutrients as part of a single system. If you’re avoiding dairy, fortified alternatives and calcium-rich foods become especially important.
The goal is not perfection. It’s adequate coverage—enough to support bones while your body recalibrates weight and metabolism.
Energy, Mood, and Immunity: Beyond the Bones
Vitamin D’s influence extends into broader wellness pathways. Some women associate low vitamin D with low mood, seasonal lethargy, or a general sense of heaviness. It’s not a universal experience, but it’s a plausible mechanism: vitamin D interacts with immune regulation and may affect neurotransmitter pathways.
GLP-1 therapies can indirectly influence mood and energy too—through appetite shifts, changes in sleep patterns, or the emotional experience of body transformation. When vitamin D is optimized, it can act like a stabilizing chord in the background music of your routine. Not an instant “glow,” but a supportive steadying force.
Think of it as an internal thermostat. Your weight loss efforts change your environment; vitamin D helps keep internal signaling from overheating or underperforming.
Common Pitfalls: What to Watch For
One pitfall is “supplement fatigue”—taking multiple products without monitoring results. Another is assuming all vitamin D is the same regardless of dose strength or form. A third pitfall is ignoring calcium intake while focusing only on vitamin D. A fourth is not considering medication-related intake changes: reduced food volume can reduce nutrient density.
Also, remember that absorption can vary. Taking vitamin D with a meal that includes dietary fat may improve uptake. If you’re experiencing gastrointestinal sensitivity on GLP-1 therapy, choose a dosing plan that your body tolerates comfortably—often with a meal.
Creating a Practical Plan: A Simple Roadmap
A cohesive plan can be beautifully unromantic: test, target, supplement if needed, and reassess. Start with lab testing (25(OH)D). Pair it with consideration of calcium intake and overall dietary pattern. Choose supplementation thoughtfully, ideally with clinician guidance, and take it consistently with meals. Add strength training and protein-forward meals where appropriate, because vitamin D supports bone and muscle best within a broader lifestyle framework.
As weeks pass and body weight changes, your nutritional needs can shift slightly. Rechecking labs after a reasonable interval can help ensure the strategy remains aligned with your current physiology. In this way, vitamin D becomes not an afterthought but a companion to your weight loss narrative—quiet, reliable, and quietly powerful.

Weight loss drugs can be a compass, but vitamin D can be a map—showing you where the body’s needs are likely to run thin. When sunlight is limited and appetite is redirected, vitamin D can help keep your internal structures strong, your energy steadier, and your progress grounded. The most compelling transformations are rarely singular. They are composite stories—medication, movement, food, and micronutrients working together like a well-rehearsed ensemble.