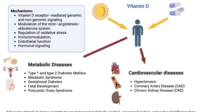
For many people, Vitamin D3 + K2 supplements arrive like a quiet reassurance: better calcium utilization, stronger bones, and a “cleaner” path toward long-term health. The marketing language feels almost serene. Yet beneath the glow of that promise lies a less discussed reality—the dark side. Not the headline-grabbing kind. The rare side effects kind. The slow-acting, often-misunderstood kind. And when you learn how these supplements can tip the body’s chemistry off balance, your perspective shifts. Suddenly, “more” is no longer automatically “better.”
Why D3 + K2 Can Feel Safe—Until It Isn’t
D3 and K2 are frequently paired because they appear to work in tandem. Vitamin D3 helps increase calcium absorption, while K2 is often described as guiding calcium toward where it belongs. In an ideal world, the calcium handling system behaves like a well-trained orchestra—precise, coordinated, and efficient.
But bodies are not static machines. They’re ecosystems. Genetics, existing diet, sun exposure, kidney function, and medication history can all change the outcome. When the balance is nudged too far in one direction, the body may respond with symptoms that don’t immediately scream “supplement reaction.” They can masquerade as fatigue, digestive disruption, or “just stress.”
The Hidden Trigger: Excessive D3 and Calcium Overdrive
The most common rarity is not “instant danger,” but biochemical drift. Vitamin D3, especially in higher doses or when combined with fortified foods, can accumulate. Over time, excess vitamin D can raise calcium levels. This state is not merely uncomfortable—it can be physiologically disruptive.
Calcium overdrive may show up as constipation, nausea, increased thirst, frequent urination, or a persistent lethargy that feels out of proportion. Some people experience muscle weakness or a metallic fatigue that makes simple tasks feel oddly heavy.
Here’s the unsettling twist: many individuals interpret these effects as unrelated issues. They might reduce water intake, change their diet, or add other supplements—unwittingly making the calcium situation worse.

K2’s Role Isn’t a Superpower: It Has Limits
K2 is often marketed like a traffic controller—directing calcium away from soft tissues. In theory, it helps prevent unwanted mineral deposition. In practice, K2 isn’t a universal shield. Its effectiveness depends on the individual’s baseline status, the dose, and the form used.
Furthermore, the body’s calcium “destinations” are influenced by more than K2. Phosphate levels, magnesium availability, vitamin A balance, thyroid signaling, and kidney health all participate in the mineral puzzle. If the puzzle pieces don’t fit, K2 cannot fully compensate.
Consider it like building a dam with the correct blueprint but different soil conditions. The concept holds. The outcome may still vary.
Rare Side Effects That Don’t Get Enough Attention
Some side effects appear rarely enough that people dismiss them as coincidence. Yet they matter because they can cluster in vulnerable individuals. Rare reactions can include headaches, unusual heart palpitations, or a “wired but tired” sensation. Others report skin changes or sensory disturbances—tingling sensations, odd pressure feelings, or transient dizziness.
Digestive symptoms can also occur: stomach discomfort, bloating, or a shift in appetite. This is especially plausible if supplements are taken on an empty stomach or with meals that alter fat absorption. Vitamin D3 is fat-soluble, and fat intake acts like a delivery system.
While these outcomes aren’t guaranteed, their existence is a reminder: even “natural” micronutrients can behave unpredictably when doses meet certain physiological conditions.
The Medication Trap: Vitamin K2 and Blood Thinners
There’s a particular shadow that follows K2 in clinical conversations: interactions with anticoagulant medications. People taking warfarin, for example, may face meaningful risk if vitamin K intake changes suddenly or drastically. This is not a subtle issue—it can affect blood clotting dynamics.
The real danger is timing and consistency. A supplement may be “consistent” on paper but inconsistent in effect across brands, dosages, or individual absorption. If blood-thinning therapy is part of your life, K2 should never be treated as a casual wellness add-on.
Instead, it requires careful coordination with healthcare guidance—because the safest strategy is informed, not hopeful.
Kidneys: The Quiet Gatekeepers of Mineral Balance
Kidneys handle more than waste. They regulate minerals, manage acid-base balance, and influence how the body copes with calcium fluctuations. When kidney function is compromised—or merely borderline—supplements that increase calcium availability can become problematic.
Symptoms may include persistent fatigue, changes in urination patterns, or discomfort that feels more internal than muscular. In some cases, elevated mineral levels may raise the risk of kidney stones, a painful reminder that mineral chemistry doesn’t stay politely in the bloodstream.
This is where “rare side effects” become conditional. The rarity is not a guarantee—it’s a probability shaped by vulnerability.

How Long Does It Take for Problems to Show Up?
Many supplement side effects operate on different timelines. Some occur soon—within hours to days—suggesting sensitivity to absorption or formulation. Others unfold gradually, reflecting cumulative vitamin D levels building over time.
This delayed onset is deceptive. You may feel “fine” at first. Then the body starts signaling that internal equilibrium has shifted. At that point, it can be difficult to connect the dots. People may stop exercising as much, sleep less well, or become irritable, assuming the cause is life stress rather than mineral imbalance.
It’s not that the body is ignoring you. It’s that the conversation is happening indirectly.
Dose Isn’t Just a Number: It’s a Strategy
One of the most overlooked elements is dosing strategy. Many supplements provide high daily amounts that may be reasonable for certain deficiency profiles—but excessive for people without them. Also, “stacking” is common: users combine D3 from multiple sources—multivitamins, separate D3 capsules, fortified drinks—without realizing the total.
In effect, the supplement becomes less an intervention and more a slow infusion. The dark side is rarely a single pill. It’s the aggregate.
For curiosity’s sake, ask yourself: Are you dosing based on labs and symptoms? Or based on assumptions and online optimism?
Formulation Matters: What’s Inside Can Change Everything
Not all D3 and K2 products are created equal. The form of K2 (often MK-7 or MK-4), the presence of cofactors, and the bioavailability of each ingredient influence outcomes. Some formulas include additional ingredients like magnesium—helpful in theory—while others are barebones, increasing the chance of an imbalance if magnesium intake is low.
Even the vehicle matters. Softgels, tablets, and liquid forms can differ in absorption. A supplement that works smoothly for one person may produce irritation or digestive discomfort for another.
Rare side effects don’t always mean rare mechanisms. Sometimes they mean rare combinations.
A Shift in Perspective: The Real Goal Is Precision
The healthiest mindset isn’t “avoid supplements forever.” It’s precision. D3 + K2 should not be treated as a universal upgrade. They’re tools. Tools require calibration. And the most compelling reason to pay attention to the dark side is that it reveals what “good supplementation” truly looks like: targeted, monitored, and respectful of biology.
If you’re considering D3 + K2, start with humility. Check your current intake. Review medications. Consider lab work such as vitamin D levels and calcium when appropriate. Then, choose a dose that fits your actual physiology rather than a generalized promise.
That’s the shift. The glow fades, but your understanding sharpens. And in a world full of claims, clarity is the most underrated benefit of all.