The sun feels generous—almost like it’s offering a warm, effortless dose of health. Vitamin D is often the headline ingredient in that story. But once you start thinking about dosing, safety can’t be ignored. A question hangs in the air: can you overdose on vitamin D from the sun? The answer is nuanced, surprisingly reassuring, and—if you’re willing to slow down for a moment—more interesting than it first appears.
Yes, Vitamin D Can Become Too Much—But Sunlight Has a Built-In Brake
Overdose sounds like a simple math problem. Yet with vitamin D, reality behaves like a careful craftsman: it allows production, then quietly reins it in. When ultraviolet B (UVB) rays hit your skin, they trigger vitamin D synthesis. The process is real, measurable, and influenced by skin tone, latitude, season, and time outdoors.
However, the body is not a passive recipient. Vitamin D production from sunlight has a photochemical feedback mechanism. As vitamin D levels rise, the skin converts the excess precursor forms into inactive compounds rather than continuing to escalate unchecked. In plain terms: the sun doesn’t just “turn on” vitamin D production and walk away. Your skin handles the off-switch.
This is why vitamin D toxicity from sun exposure is considered rare. It’s not impossible, but it’s uncommon enough that most people do not need to live in a state of vigilant suspicion.
What “Overdose” Actually Means: Toxicity Is About Blood Levels
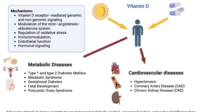
The phrase “overdose” isn’t about feeling too sunny or getting a little too much color. Vitamin D toxicity is about measurable biochemical consequences—especially elevated blood calcium levels (hypercalcemia). When vitamin D becomes excessive, the intestine absorbs more calcium than the body can manage. That calcium surplus may begin to interfere with kidney function and can affect bones, muscles, and the cardiovascular system.
Symptoms, when they occur, are often indirect and irritatingly non-specific. People might experience nausea, constipation, excessive thirst, frequent urination, weakness, confusion, or fatigue. These aren’t the kinds of clues that scream “vitamin D” to the average observer. They’re the sort of breadcrumbs that only a clinician would know how to follow.
So the real question isn’t “Can sunlight overfeed vitamin D?” It’s “Can sunlight push your vitamin D-calcium axis beyond safe territory?” For most individuals, sunlight alone doesn’t reach that territory.
Sunlight vs. Supplements: Two Different Risk Profiles
Sunlight is “adaptive” vitamin D delivery. Supplements are “dose-determined” vitamin D delivery. That distinction matters.
Vitamin D supplements—especially high-dose products taken daily or weekly without monitoring—can raise blood levels much more predictably than casual sun exposure. A capsule can deliver an amount that your skin would never generate during normal outdoor life, particularly because skin synthesis is limited by the aforementioned photochemical brake.
In other words, the highest-risk scenario is often not the beach day. It’s the stacking effect: supplements combined with fortified foods, plus occasional large “therapeutic” doses recommended by someone who hasn’t reviewed existing lab values.
If you’re thinking about vitamin D intake, let your bloodwork—not your optimism—be the guide.
Who Might Be More Vulnerable to Excess Vitamin D?
Although sun-induced toxicity is rare, certain circumstances can shift the odds. People with disorders that increase vitamin D sensitivity or calcium regulation may be at higher risk even at lower intakes. Examples can include specific granulomatous diseases (where the body produces active vitamin D forms differently) or certain genetic conditions that affect calcium balance.
Also consider behavior patterns: extremely prolonged, unprotected exposure to intense UV—think tanning booths, high UV index environments, and long outdoor sessions without shade or sunscreen. While sunscreen doesn’t eliminate vitamin D production entirely, it does reduce UVB exposure, which can decrease the chance of excessive synthesis.
Finally, medication interactions can matter. Some drugs influence calcium or vitamin D metabolism. Risk becomes more complex when your body is working under pharmacological constraints.
Vulnerability isn’t a label; it’s a context. When context changes, caution becomes smarter.
Skin Tone, Latitude, and Season: The “Same Sun” Isn’t the Same Dose
Vitamin D production is not uniform. Skin pigmentation influences how much UVB penetrates to trigger the synthesis pathway. Darker skin tones generally require more UV exposure to produce the same vitamin D amount as lighter skin. That’s why two people—standing side by side in identical sunlight—can walk away with different vitamin D outcomes.
Geography plays its part too. At higher latitudes, UVB availability changes dramatically across the seasons. During winter months, sunlight may be too weak for meaningful vitamin D synthesis, which can lead people to compensate by supplementing more aggressively.
Another factor is time and intensity. Midday sun in a high UV index region is a different experience from late afternoon exposure. Even the angle of the sun affects how much UVB reaches the skin surface.
So rather than asking, “How long do I need?” it’s wiser to ask, “What’s my likely net UVB exposure, and what does my body show on lab tests?”
Signs You Should Pause: Symptoms and When to Seek Testing
If you’re worried about vitamin D excess, your body may hint at imbalance—though it won’t always do so politely. Common warning signals associated with high calcium can include persistent nausea, constipation, reduced appetite, or a strange sense of mental fog. Some people also report increased thirst and urination.
Muscle weakness and unusual fatigue may appear. In severe cases, kidney-related symptoms can become prominent. But again: symptoms are not a diagnosis. They are a prompt to investigate.
Testing usually includes serum 25-hydroxyvitamin D (the standard vitamin D status marker) and calcium levels. A clinician may add kidney function tests and other relevant labs based on your history. Think of it as checking the thermostat rather than guessing whether the room is too hot.
How to Get Vitamin D Safely From Sun Without Anxiety
Safety doesn’t require fear. It requires intention.
Start with moderation and consistency. Short, regular exposure—during times when UVB is available—can help maintain adequate status for some people. The goal is not to “maximize” sun at all costs; the goal is to balance vitamin D needs with skin cancer risk reduction.
Use protective strategies thoughtfully. Sunscreen reduces UVB, but it can be part of a responsible routine, especially when exposure is longer than necessary. Clothing and shade aren’t enemies; they are tools. They help prevent sunburn, which is one of the most visible and immediate risks.
Because individual needs vary, the most grounded approach is periodic bloodwork—particularly if you supplement or if you live in a low-UV environment.
The Bottom Line: Sun Overdose Is Uncommon, Supplements Are the Bigger Concern
Can you overdose on vitamin D from the sun? For most people, the answer is: it’s unlikely. Your skin has adaptive defenses that limit runaway vitamin D production. The risk becomes more plausible with extreme, sustained UV exposure and certain medical contexts, but even then, it remains comparatively rare.
The more frequent path to vitamin D excess is supplement-based—especially high-dose regimens taken without monitoring or combined with fortified sources. If you’re taking vitamin D (or considering it), labs are the lantern in the fog.
In the end, the sun is a powerful ally, not a vending machine. Treat it with respect, not suspicion, and let your body’s measurements tell you whether you’re thriving or tipping into excess.