Vitamin D has a reputation for being “safe” because it’s sold everywhere—from pharmacies to sleek wellness supplements. Yet when the dosage climbs into the high-dose territory, the story becomes more complicated. Your doctor may discuss deficiency and dosing ranges, but there’s a quieter conversation that many people never hear: what happens when high-dose vitamin D becomes a long-running habit, how different forms behave in the body, and why symptoms can masquerade as unrelated ailments. The goal isn’t fear. It’s discernment—so you can recognize when a supplement is helping versus quietly steering your physiology off-course.
Why “High-Dose” Isn’t a Single, Simple Thing
High-dose vitamin D can mean dramatically different regimens. Some people take 5,000 IU daily. Others use 50,000 IU weekly. Still others stack products—vitamin D plus a multivitamin plus “immune” blends—without realizing they’re effectively self-prescribing a cumulative dose.
Doctors often tailor recommendations to blood levels, body weight, comorbidities, and medication interactions. But the public sees only the bold numbers on labels. That creates a mismatch between marketing clarity and biological reality. Vitamin D isn’t merely a vitamin in the nutritional sense; it functions more like a hormone precursor with downstream effects on calcium handling, bone metabolism, immune signaling, and cellular differentiation.
There’s also timing. Vitamin D isn’t instant fuel; it accumulates. A dose that seems reasonable on day one may become excessive after weeks or months. This time-dependent buildup is one of the reasons high-dose regimens should be monitored rather than assumed.
The Forms Matter: D2 vs D3 and the Hidden Variables
Vitamin D comes in multiple chemical forms, most commonly D2 (ergocalciferol) and D3 (cholecalciferol). D3 is frequently preferred in clinical discussions because it tends to raise and sustain serum 25-hydroxyvitamin D more effectively for many people. Still, the “type” is only one variable.
Absorption can vary based on whether the supplement is taken with meals containing fats, the formulation (oil-based, emulsion, or tablet), and individual digestive efficiency. Some people have subtle malabsorption patterns—celiac disease, pancreatic insufficiency, inflammatory bowel conditions, or prior bariatric surgery—that make standard dosing behave unpredictably.
Even the packaging can mislead. A “high-dose” product might be intended as a short-term repletion strategy, yet used indefinitely. That’s where the risk profile begins to tilt from corrective to cumulative.
The Mechanism That Changes Everything: Calcium, Kidneys, and Hypercalcemia
The most consequential pathway tied to excessive vitamin D involves calcium. Vitamin D helps the gut absorb calcium and influences how the body balances calcium in bone and blood. When vitamin D levels become too high, calcium absorption can surge. The result may be hypercalcemia—elevated blood calcium—and, in some cases, hypercalciuria (excess calcium in urine).
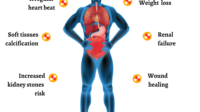
Hypercalcemia is not just a lab curiosity; it can create a constellation of symptoms that feel unrelated to vitamin D: fatigue, thirst, constipation, nausea, confusion, and muscle weakness. Long sentences can’t capture the full nuance here—your body may essentially “misread” the calcium signal as an instruction to behave differently.
Kidneys are particularly sensitive. Elevated calcium can contribute to kidney stones and, in more severe scenarios, impair renal function. This is why clinicians emphasize monitoring, especially for people with a history of kidney disease, kidney stones, or conditions that affect calcium metabolism.

Symptoms That Don’t Look Like a Vitamin Problem
A frequent complaint is: “Why does this feel like something else?” High-dose vitamin D excess can produce symptoms that resemble dehydration, gastrointestinal upset, or general malaise. Think of it like a smoke alarm that’s triggered by steam from a kitchen appliance—you still see the alarm, but the source isn’t what you expected.
Commonly reported signs can include persistent nausea, appetite changes, constipation, increased urination, excessive thirst, headaches, and lethargy. Some people describe mental fog. Others notice cramps or weakness. The pattern is often subtle at first, then becomes more obvious as calcium derangements worsen.
The danger of misattribution is real. If someone assumes symptoms are “detox” or “just stress,” they may continue high dosing—tightening the loop.
Who Should Be Extra Cautious Even With “Normal” Blood Levels?
Serum 25-hydroxyvitamin D is the standard marker for vitamin D status, but it doesn’t tell the entire story about toxicity risk. Certain individuals are more vulnerable even when levels aren’t dramatically abnormal. Risk increases with conditions that predispose to hypercalcemia or kidney complications.
People with granulomatous diseases (like sarcoidosis) may have altered vitamin D metabolism that can amplify calcium absorption. Those with primary hyperparathyroidism can have calcium regulation already tilted. Some disorders affecting phosphate or calcium balance also matter.
Medication interactions add another layer. Thiazide diuretics, for example, can raise calcium levels. Long-term use of certain drugs, coexisting supplements, and high dietary calcium can further intensify the risk environment.
In other words, the same dose doesn’t create the same biological outcome for every body.
How Doctors Often Reframe the Conversation: Deficiency vs. Optimization
In clinical settings, the conversation frequently starts with deficiency and correction. The aim is to restore adequate vitamin D and protect bone health. But online wellness culture often treats vitamin D as a performance enhancer for immunity and longevity—pushing the narrative toward “optimization.”
Optimization is not inherently wrong. Yet it can encourage indefinite dosing without periodic measurement. Vitamin D is not a vitamin you can “set and forget” at high doses. The body adapts. Serum levels rise. Calcium physiology responds. Eventually, the margin narrows.
A thoughtful medical approach tends to use a goal, a timeline, and a monitoring plan. Anything else is guesswork.
What Monitoring Should Look Like (and What to Ask For)
Monitoring is where confusion should end. If high-dose vitamin D is being used—especially beyond a short repletion phase—ask about which labs will be tracked. Typically, clinicians examine serum 25-hydroxyvitamin D and also assess calcium. Depending on the situation, they may also consider kidney function (such as serum creatinine) and sometimes urinary calcium if stone risk is suspected.
Short testing windows can miss what’s actually happening. Vitamin D takes time to equilibrate, so repeating labs too quickly may yield misleading results. Long sentences are useful here—because the timeline matters: dosing duration, baseline levels, and the time of the last dose can all influence outcomes.
Equally important is dose review. Many patients discover they’ve been stacking multiple sources. A good monitoring plan counts the entire regimen, not just the single “main” supplement.
Why Some People Feel Better on High Doses—Then Pay Later
It’s not unusual to hear that high-dose vitamin D made someone “feel great.” Early improvement can occur for several reasons: correcting a true deficiency, placebo effects, changes in routine, or simultaneous adjustments to sleep and diet. The body can benefit when deficiency is real and vitamin D is insufficient.
But the relief may arrive early, while toxicity risk builds more slowly. That’s the paradox: symptom improvement doesn’t guarantee physiologic safety. The labs may still be climbing. Calcium can begin to shift before symptoms become severe.
This is why “I felt better” is not a sufficient safety metric. The safest confirmation comes from objective monitoring and a sensible dosing ceiling guided by a clinician.
Formulating a Safer Strategy: Short Courses, Lower Maintenance, and Lifestyle Support
A safer path often looks like this: treat deficiency with a time-limited high-dose strategy (if clinically appropriate), then transition to a lower maintenance dose. Maintenance should align with measured levels and risk factors, not guesswork or trend-driven enthusiasm.
Lifestyle also plays a role. Sensible sun exposure—when safe for your skin—can support vitamin D. Diet contributes modestly through fatty fish, fortified foods, and eggs. But diet alone rarely replaces high-dose correction for deficiency. Still, it can help stabilize once levels are in a comfortable range.
Think of vitamin D as part of a system rather than a standalone commodity.
When to Stop and Seek Medical Advice
If you experience symptoms consistent with hypercalcemia—marked thirst, frequent urination, persistent constipation, nausea, weakness, confusion—or if you have a history of kidney stones or kidney disease, pause high-dose use and seek medical evaluation promptly. Waiting can be counterproductive.
Medical advice should include a complete review of supplements and medications. People often forget to mention calcium supplements, multivitamins, or “immune support” products. Bring labels. Provide dosages. Make the clinician’s job easier by making the full picture visible.

The Bottom Line: Knowledge Beats Guessing
High-dose vitamin D can be therapeutic when used correctly, but it can also become a stealth hazard when taken indefinitely, stacked unknowingly, or used without monitoring. The part many people don’t hear is not that vitamin D is “bad.” It’s that the biology is vigilant—and it responds to excess with calcium-focused consequences that can affect kidneys and overall well-being.
When dosing decisions are paired with lab work, a clear timeline, and a review of individual risk factors, vitamin D becomes a precision tool rather than a gamble. The smartest move is not to chase the highest number—it’s to land in the safe, steady range your body can tolerate.