There’s a particular kind of myth that follows vitamin D—one that sounds almost soothing: “If it comes from the sun, it must work naturally, without needing the body to do anything complicated.” But the story is more nuanced. Vitamin D arrives in your cells like a message that must be decoded, routed, and ultimately processed. The real question isn’t simply whether sunlight provides it. The deeper question is whether sunshine depends on fat absorption to become useful in the body.
Hold that thought for a moment. Imagine your skin as a solar panel, yes—but also as a loading dock. Light triggers the first act, while biology determines the final performance. And when fat enters the narrative, it’s less about “absorption” in the simplistic sense and more about the physiology of how vitamin D travels, transforms, and persists.
Sunlight’s Beginning: From Skin Chemistry to Vitamin D’s Precursor
When ultraviolet B (UVB) radiation strikes the skin, it initiates a chemical conversion. You don’t “eat” vitamin D from the sun. Instead, your skin manufactures a precursor that later becomes biologically active. This early stage feels almost elegant in its efficiency: light arrives, chemistry responds.
What’s easy to miss is that the first conversion is only a preface. The body still needs to convert that precursor into more functional forms. These transformations involve enzymes, transport proteins, and specific organ pathways. Even if sunlight is the spark, the furnace is internal.
To visualize the journey from one form to another, consider the broader chain of vitamin D forms and how each step can influence how the body ultimately uses vitamin D.
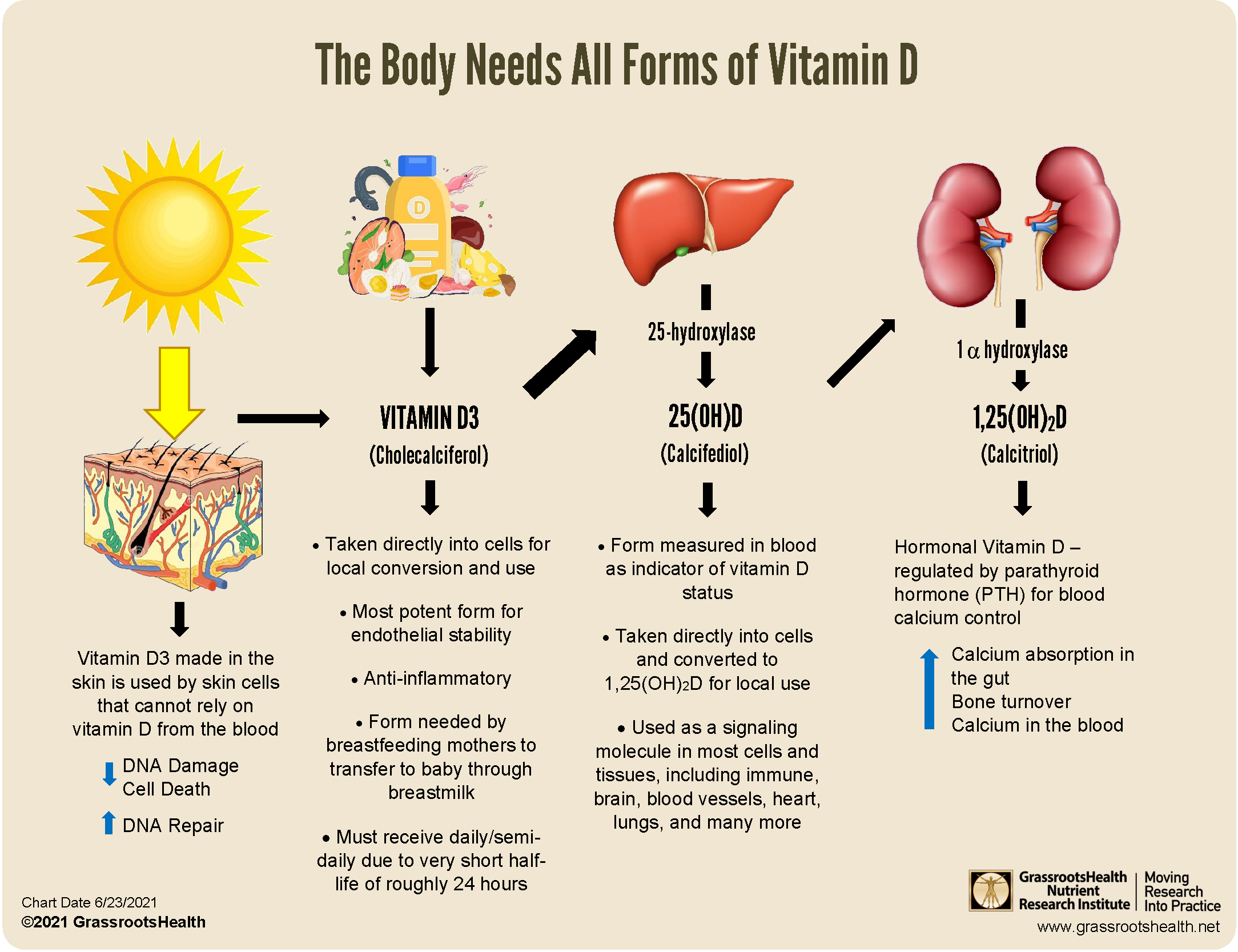
The “Fat Absorption” Question: What Actually Needs Dietary Fat?
Here’s the shift in perspective that changes everything: vitamin D from sunlight does not originate in the digestive tract. That means it doesn’t begin its lifecycle as a nutrient that must be micellized in the gut.
However, “not requiring absorption” can be misinterpreted. Yes, sunlight-derived vitamin D is not absorbed the way a fat-based supplement is. But vitamin D is still a fat-soluble molecule. That fat-soluble nature affects how it circulates in the bloodstream and how it is stored, transported, and handled by tissues.
In other words, sunlight may bypass the stomach-and-intestine hurdle. Yet the body still uses fat-compatible transport strategies once vitamin D is produced. Think of it like this: the door you don’t use (intestinal absorption) isn’t the same as the highway the molecule still travels (blood transport and storage in lipid compartments).
Fat-Soluble by Nature: Why Transport and Storage Still Matter
Vitamin D belongs to the club of fat-soluble vitamins. That label describes behavior: vitamin D tends to associate with lipid environments and circulatory transport systems. Once made in skin, it enters the bloodstream bound to transport proteins. From there, it journeys to the liver and kidneys for conversion into the hormonal forms your body can employ.
This is where curiosity pays off. If vitamin D is fat-soluble, could low-fat conditions reduce its effectiveness? The most accurate answer is conditional: insufficient dietary fat can influence absorption of supplemental vitamin D and may indirectly affect vitamin D status in some people. But for people relying primarily on sunlight exposure, the initial step is different.
Still, a diet extremely low in fat can be a broader physiological stressor. It may alter bile availability, lipid metabolism, and the body’s overall handling of fat-soluble compounds—potentially affecting circulating vitamin D even if it began as sun-produced.
The Liver and Kidney Conversions: A Detour That Isn’t About Digestion
After skin synthesis, vitamin D is converted in stages. The liver transforms it into a circulating storage/transport form, and the kidneys further refine it into the active form that can signal across the body. These steps are biochemical gatekeeping processes, not digestive chores.
This is a crucial distinction. If the body’s conversion machinery is functioning well, vitamin D can be processed regardless of whether you “absorbed” it from food. That said, organ health, metabolic conditions, and certain medications can influence vitamin D metabolism—complicating any simplistic narrative.
So rather than asking only “Does it require fat absorption?” you can ask more informative questions: How efficiently does the body convert vitamin D? How effectively does it circulate and maintain adequate levels over time? Those answers may matter more than the gut-based framing.
Sunlight vs. Supplements: Different Entry Points, Different Rules
Supplements often come as fat-based formulations, which means they commonly rely on the digestive tract’s capacity to absorb lipids. Many people have heard that vitamin D “needs fat,” and the statement tends to be most accurate in the context of oral supplements—especially those absorbed without adequate dietary lipid support.
Sunlight-derived vitamin D, by contrast, begins with cutaneous production. No digestion is required for the initial creation. Yet the molecule still ends up in a physiological system that is lipid-friendly and protein-bound. The overlap can make it feel like “fat is required” in every scenario, but it’s not the same kind of requirement.
Think of two pipelines. Supplements enter through a digestive checkpoint that may demand dietary fat for efficient absorption. Sunlight enters through skin chemistry and then routes to conversion organs. Both pipelines eventually meet at the same biochemical crossroads where transport and storage mechanisms matter.
What the Evidence Suggests: Plausible Scenarios Where Fat Still Becomes Relevant
Vitamin D from sun exposure may not depend on gut absorption, but fat status and fat handling can still become relevant in real life. Here are plausible scenarios where the “fat requirement” reappears as a practical concern:
First, people with very low dietary fat intake might have altered bile flow and lipid metabolism. While this primarily affects absorption of nutrients in the gut, it can also influence lipid transport systems that vitamin D uses after it circulates.
Second, malabsorption syndromes—conditions affecting how fats are processed—may reduce overall lipid handling and potentially influence vitamin D status over time, even if a portion is produced in skin. The body is an interconnected system. When one pathway stumbles, another can be indirectly impacted.
Third, obesity can complicate vitamin D dynamics. Vitamin D may become sequestered in adipose tissue, changing how much remains circulating. In such cases, sunlight exposure might still produce vitamin D, but the relationship between exposure and blood levels can become less straightforward.
These scenarios don’t overturn the core idea—sunlight can supply vitamin D without digestive absorption. They refine it. The body’s lipid economy still participates in the story.
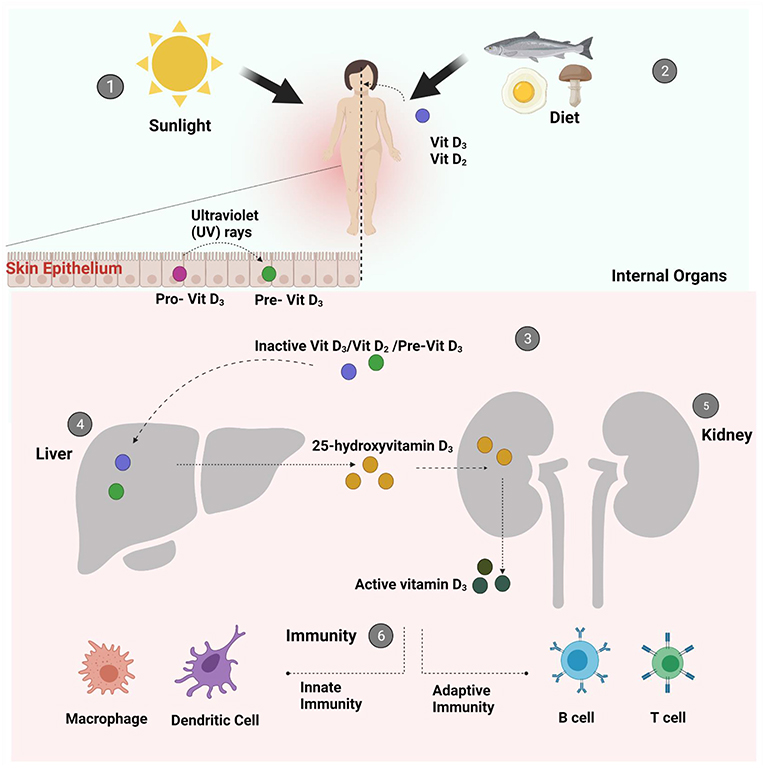
Curiosity Pathway: How Much Sun Is Needed for Meaningful Vitamin D?
Here’s another perspective shift: sunlight is not a single, fixed “dose.” It varies by season, latitude, time of day, cloud cover, skin pigmentation, age, and even clothing habits. The same exposure can yield different outcomes across individuals.
If vitamin D production is inconsistent, blood levels may drift downward, and people then search for a backup strategy—often supplements. That’s when fat absorption becomes more central. Not because sunlight suddenly requires fat, but because consistent vitamin D input is harder to guarantee.
Curiosity naturally follows: what happens if sun exposure is minimal? In that situation, dietary sources and supplements become more influential. The body then relies more on intestinal absorption pathways—where fat compatibility matters more.
Practical Takeaways: A Balanced, Less-Mythical View
So, does vitamin D from the sun require fat absorption? The clean answer is: not in the same way oral supplements do. Sunlight-driven vitamin D production originates in the skin and then moves through conversion pathways that are not dependent on intestinal micellization.
Yet the nuanced answer is: fat still influences vitamin D physiology because vitamin D is fat-soluble and uses lipid-friendly transport and storage routes. Extremely low-fat diets, malabsorption conditions, obesity-related distribution, and broader metabolic factors can make vitamin D status more variable.
In the end, the most empowering approach is to treat vitamin D like a system, not a trick. Sunlight supplies the raw starting material. Your organs refine it. Transport and storage govern how it persists. And diet may matter more for the supplement pathway, while still shaping the environment vitamin D travels through.
To keep the message grounded, remember this: sunlight can generate vitamin D without digestive fat absorption, but your body still runs a choreography that includes lipid handling.











