What if two seemingly unrelated allies—vitamin D and GLP-1—could coordinate like a well-rehearsed ensemble to nudge type 2 diabetes toward remission? Imagine the metabolic orchestra: one instrument tunes the immune and endocrine “room acoustics,” while the other conducts insulin dynamics with a rhythmic precision. Now, here’s the playful snag in the plot—what happens when the body’s rhythms are out of sync, or when the available “keys” (vitamin D status, receptor sensitivity, adherence, and tolerability) don’t quite match the music?
Setting the Stage: Why Remission Feels Like a Cinematic Twist
Diabetes remission isn’t a single event; it’s an evolving state. Clinically, it often refers to the ability to maintain near-normal glycemia without the usual diabetes medications for a sustained period. This is not mere luck—it’s metabolic restructuring. Long-standing insulin resistance, β-cell stress, inflammatory signaling, and dysregulated appetite pathways can all act like chain links. Break one link and the chain loosens; break several and the whole mechanism can change.
Vitamin D enters the narrative through its immunomodulatory and endocrine roles. GLP-1 (and GLP-1 receptor agonists) enters through appetite regulation, gastric emptying modulation, and insulin secretion support. Together, they suggest a synergy: one may lower the “background static,” while the other optimizes the “signal-to-noise ratio” of glucose control.
But the challenge remains: synergy is rarely automatic. The body is a complex system, and each “character” has constraints—baseline vitamin D levels, variability in response to GLP-1 therapies, and the practical realities of lifestyle adherence.
Vitamin D Beyond Bone Health: The Endocrine, Immunologic, and Metabolic Angle
Vitamin D is often introduced as a skeletal caretaker, yet its receptors are active across multiple tissues. In metabolic contexts, vitamin D participates in immune regulation and may influence insulin sensitivity. It can affect inflammatory pathways—important because chronic, low-grade inflammation is a recurring antagonist in diabetes.
There’s also a conceptual bridge between vitamin D and insulin signaling: when vitamin D status is insufficient, cellular communication can become less efficient. Imagine insulin as a key and the cellular door as the receptor system; vitamin D may help polish the lock so the key fits more smoothly. When levels are low, the “keyholes” may function less gracefully.
Another intriguing dimension is adipose tissue behavior. Fat cells are not passive storage units; they can secrete cytokines that nudge the inflammatory tone. Vitamin D may help shift that tone, potentially reducing pro-inflammatory signaling that worsens insulin resistance.
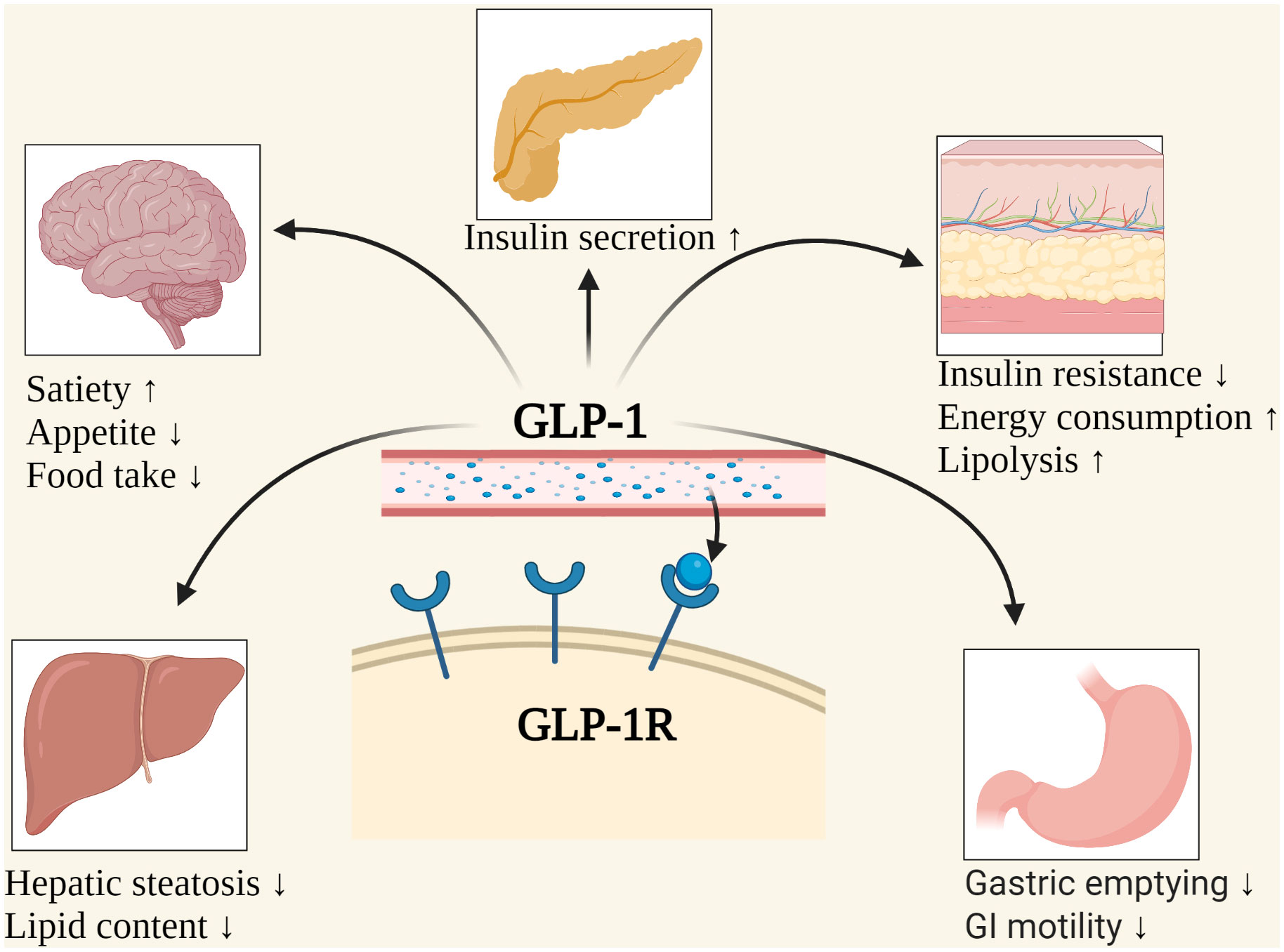
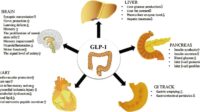
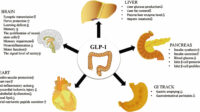
GLP-1 and the Metabolic “Conducting Baton”: More Than Just Insulin
GLP-1 receptor agonists are frequently described as incretin-based therapies. That’s true, but it’s also partial. GLP-1 signaling improves glucose regulation through multiple routes: it enhances glucose-dependent insulin secretion, suppresses glucagon when glucose is elevated, and slows gastric emptying—reducing post-meal glucose excursions.
There’s a behavioral component too. GLP-1 pathways can diminish appetite and improve satiety. This matters because weight reduction often improves insulin sensitivity. In practical terms, GLP-1 therapy may help patients create a metabolic environment in which remission becomes more feasible, especially when diabetes is relatively recent or when β-cells still retain some functional reserve.
One potential challenge is heterogeneity in response. Some individuals experience robust glycemic and weight benefits; others see a more modest shift. Tolerability—especially gastrointestinal side effects—can influence persistence and dose optimization. If the therapy is discontinued prematurely, the “conducting baton” loses its tempo.
Where the Synergy Might Live: Inflammation, Insulin Sensitivity, and Appetite Circuits
Synergy implies overlapping mechanisms that reinforce each other. Vitamin D may dampen inflammatory signaling and support insulin sensitivity. GLP-1 therapy may improve insulin dynamics and reduce appetite-driven glucose volatility. Together, they could reduce both the “inflammatory weather” and the “sugar surges” that typically reinforce diabetes progression.
Consider the downstream consequence: improved insulin sensitivity lowers the demand placed on β-cells. GLP-1’s insulin-supportive effects can further preserve β-cell function. When stress drops and signaling becomes more efficient, the metabolic system may stabilize at healthier glycemic set points.
Now the playful question resurfaces: what if vitamin D status is low and appetite improvements are incomplete? In that case, GLP-1 may still help, but the inflammatory background might not be fully recalibrated. Conversely, what if vitamin D levels are optimized but GLP-1 adherence is inconsistent? Then the appetite and glucose-physiology “rhythms” may remain irregular.
Possible Pathways: From Adipose Signaling to Glucose Stability
Synergy may also involve adipose tissue physiology. Weight loss, improved insulin sensitivity, and altered cytokine patterns can create a favorable loop. GLP-1’s weight effects can reduce adipose-driven inflammatory signaling. Vitamin D may support immune regulation, potentially amplifying the anti-inflammatory benefits of metabolic improvement.
Additionally, both pathways may interact with cellular signaling cascades that affect insulin responsiveness. Even when the exact molecular choreography varies between individuals, the clinical proposition remains: multiple levers—metabolic, inflammatory, and behavioral—can be pulled at once to increase the probability of remission.

Remission Feasibility: Who Might Benefit Most?
Remission is often more attainable when diabetes is detected earlier, when β-cell function is not deeply exhausted, and when metabolic stressors are addressed promptly. GLP-1 therapy tends to be particularly relevant in patients who struggle with appetite regulation and weight-related insulin resistance.
Vitamin D relevance may be greater in those with deficiency or insufficiency. Low vitamin D status is not merely a lab anomaly; it may reflect limited sunlight exposure, dietary patterns, darker skin pigmentation in certain contexts, or absorption issues. Correcting deficiency can be part of a broader “metabolic hygiene” plan.
However, “more intervention” is not automatically “better outcomes.” A key challenge is personalization. The same combination can play out differently depending on baseline A1C, duration of diabetes, kidney function, concurrent medications, and lifestyle consistency.
A Practical Strategy: Timing, Testing, and Thoughtful Integration
In a synergy-minded approach, vitamin D adequacy is assessed and addressed—typically through blood testing of 25-hydroxyvitamin D—followed by individualized supplementation guidance. Meanwhile, GLP-1 therapy is titrated to optimize glycemic response while minimizing adverse effects. Smooth titration matters. Sudden escalation can amplify gastrointestinal symptoms, which can derail adherence.
Then comes the lifestyle “glue”: meal composition, fiber intake, physical activity, and sleep quality. GLP-1 may reduce appetite, but nutrition quality determines whether weight loss is accompanied by stable energy levels and minimal micronutrient deficits. Vitamin D support can be less effective if sun exposure patterns, diet, and supplementation are inconsistent.
In other words, the synergy isn’t only pharmacologic. It’s also behavioral synchronization—turning intermittent effort into a reliable cadence.
Potential Challenges and Misconceptions: Where the Story Can Go Off-Road
One challenge is assuming a guaranteed remission outcome. Remission is possible, but it is probabilistic. Diabetes biology can be relentless, especially when insulin deficiency becomes prominent or when comorbidities accumulate.
Another challenge is dosing logic. Vitamin D supplementation should not be blind. Excess vitamin D can be harmful, and clinical targets should be interpreted with context. GLP-1 dosing also requires caution, particularly for patients with risk factors for pancreatitis, gallbladder disease, or severe gastrointestinal intolerance.
There’s also the misconception that vitamin D “replaces” diabetes management. It doesn’t. It may support metabolic resilience, but it is not a substitute for evidence-based diabetes therapies. The synergy concept is additive and supportive—not a magical reversal switch.

Monitoring Progress: Looking Beyond A1C
Tracking remission readiness may involve more than A1C. Weight trajectory, fasting glucose patterns, post-meal glucose responses, and markers of inflammation can provide clues. Medication adjustments should be guided by clinicians using standardized criteria, including sustained glycemic thresholds off therapy when appropriate.
It’s also wise to monitor vitamin D status and calcium-related parameters when supplementation is used. The goal is balance: enough to support biological signaling, not so much that it creates a new risk profile.
Conclusion: A Hopeful, Nuanced Partnership
Vitamin D and GLP-1 can be thought of as partners in a broader remission narrative—one potentially reducing inflammatory friction and supporting insulin sensitivity, the other improving glucose regulation and appetite-driven metabolic stability. The synergy hypothesis is compelling because it targets multiple nodes at once.
Yet the plot remains conditional. The body must receive the right inputs at the right intensity, and the patient must be supported through tolerability challenges, lifestyle synchronization, and appropriate monitoring. If those conditions align, remission may become less of a rare miracle and more of an attainable trajectory—like a story that finally clicks into its intended ending.