After 40, the body’s quiet chemistry starts to change. Not dramatically—at first it’s more like a subtle reframing of priorities. Bones may lose mineral density at a gradual pace, muscles can become slightly less responsive, and the immune system often feels the strain of time. In this landscape, vitamin D and calcium act like essential collaborators: one helps unlock calcium’s usefulness, the other provides the structural materials. When the balance is right, strength feels less like a wager and more like a strategy.
Why 40 Marks a Shift in Calcium and Vitamin D Needs
Age doesn’t flip a switch. It edits the script. With time, the intestines can absorb calcium less efficiently, and the skin’s ability to synthesize vitamin D from sunlight may decline. Meanwhile, bone remodeling continues—old bone is removed and new bone is formed—but the equilibrium can tilt. Even if you’re active, this tilt may gradually reduce bone mineral density, increasing the risk of fragility fractures.
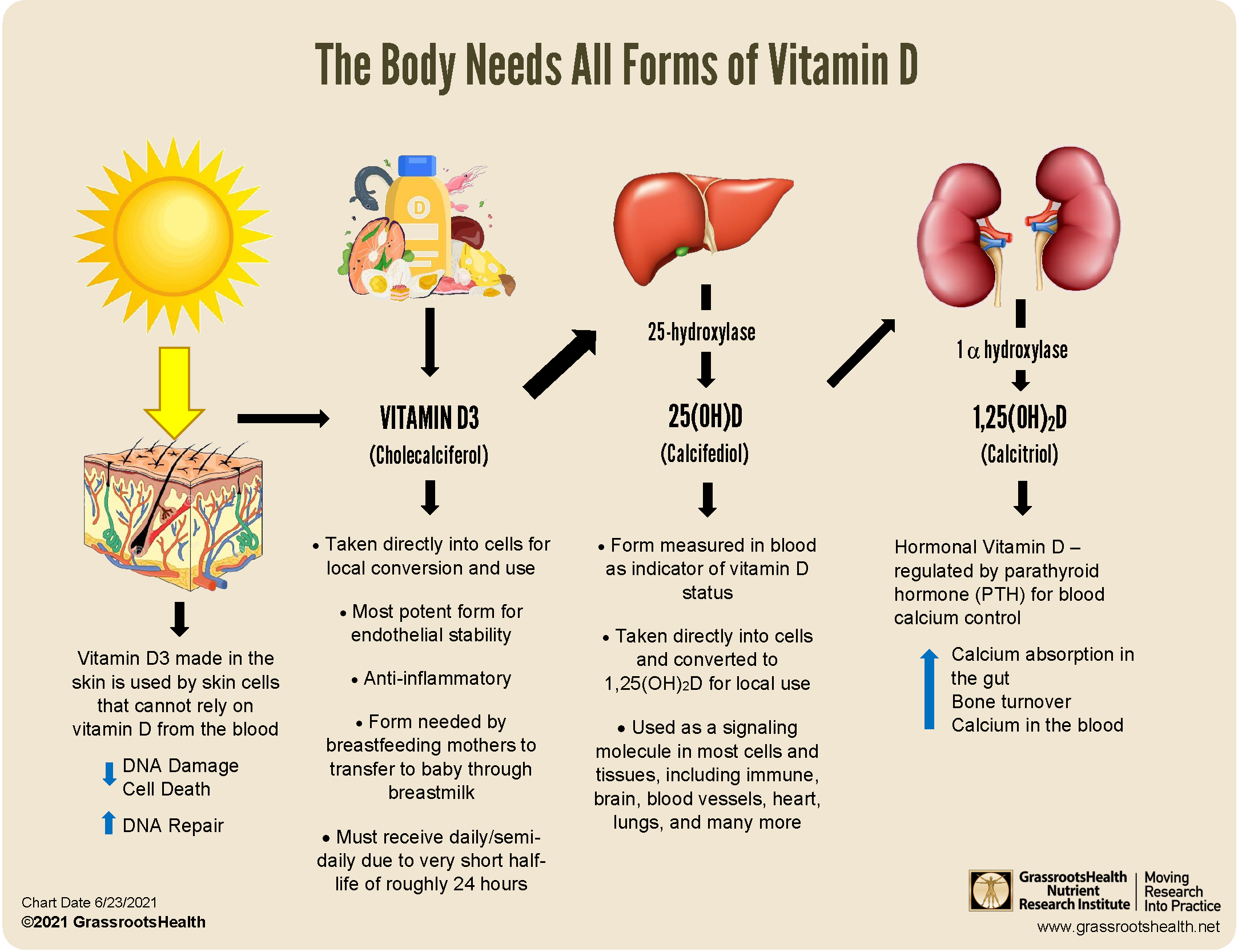
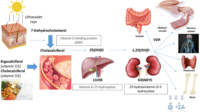
Vitamin D is the conductor in this scenario. It supports calcium absorption and helps regulate calcium and phosphate metabolism, which is crucial for skeletal integrity. Calcium, in turn, is the building material. Together they help maintain bone hardness and functional resilience, which is not only about preventing osteoporosis—it’s also about preserving mobility, posture, and the confidence to move without fear.
Understanding Calcium: The Mineral Blueprint for Strength
Calcium is more than “strong bones” in a single-line summary. It participates in muscle contraction, nerve signaling, and cellular communication. That means inadequate calcium intake doesn’t always announce itself with dramatic symptoms. Instead, it can erode long-term stability—sometimes quietly, sometimes through vague fatigue or a slower recovery after exertion.
Dietary calcium can come from dairy products (milk, yogurt, cheese), fortified plant milks, leafy greens like kale and bok choy, and calcium-set tofu. However, not all sources behave identically in the digestive system. Some foods contain compounds that influence absorption. Processed dairy tends to be bioavailable, and fortified options can meaningfully contribute if they’re consumed regularly.
For readers who prefer a practical approach, think in patterns: daily intake beats sporadic “catch-up.” The body uses calcium continuously, so consistency has a kind of understated power.
Vitamin D: The Gatekeeper of Absorption and Bone Metabolism
Vitamin D is often described as a vitamin, but its behavior is more hormone-like. It influences gene expression and orchestrates calcium absorption. When vitamin D levels are low, calcium absorption can drop, and bone can become a reservoir the body draws from to maintain blood calcium within a narrow, regulated range.
Vitamin D can be obtained through sunlight exposure, certain foods, and supplements. Sunlight is efficient but unpredictable depending on geography, season, skin pigmentation, clothing coverage, and sunscreen habits. Dietary vitamin D is less abundant than calcium, with fatty fish (salmon, sardines, mackerel) and fortified products being common contributors.
Some people experience vitamin D deficiency without any obvious warning. That’s why awareness matters: fatigue, muscle aches, or general low resilience can appear, but they’re not definitive. Testing offers clarity—particularly if you have limited sun exposure, darker skin, a history of bone issues, or dietary constraints.
The Right Balance: How Much Is Enough Without Overdoing It
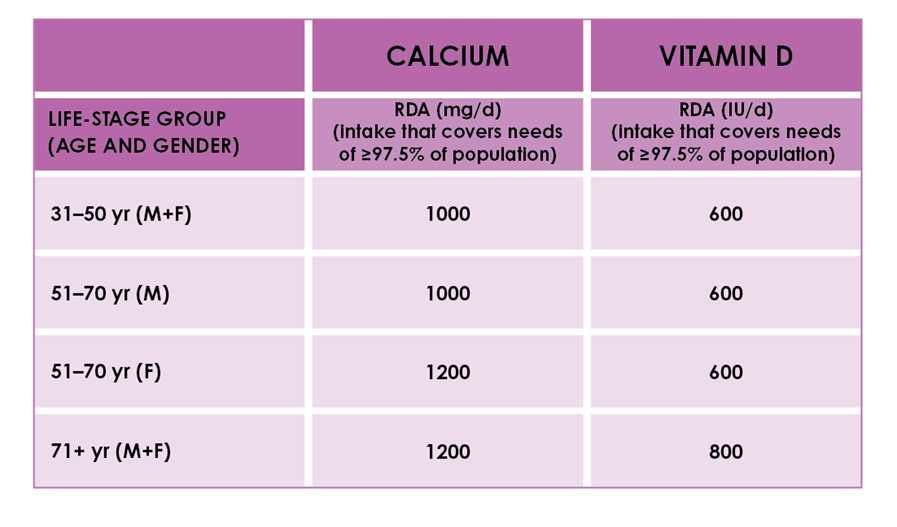
Balance isn’t just “more” versus “less.” It’s a calibrated approach that respects individual biology. Calcium and vitamin D requirements vary depending on sex, diet, activity level, health conditions, and the outcomes of blood tests.
Too little calcium can compromise bone integrity. Too much—especially from supplements—may introduce concerns such as kidney stone risk in susceptible individuals. Vitamin D excess can also be problematic, mainly through hypercalcemia (too much calcium in the bloodstream). That means supplementation should be thoughtful, not automatic.
A helpful lens is to start with food as the foundation, use supplements as a bridge when needed, and treat lab results as navigational instruments rather than inconveniences. If a healthcare professional recommends supplements, following the specified dose tends to be the safest route. In other words: precision beats optimism.
Food First: Building a Daily Menu of Calcium and Vitamin D
When readers want “what do I actually eat?” the conversation becomes more human. Calcium-rich meals can be woven into the day in small, repeatable ways. A yogurt bowl for breakfast, a portion of cheese or fortified dairy alternative at lunch, and leafy greens at dinner can create a steady rhythm.
Vitamin D can be more challenging through food alone, but it’s doable. Regular intake of fatty fish a few times per week can help. Fortified milk, fortified plant beverages, and fortified cereals also contribute, though the label matters—fortification levels vary.
Pairing can be surprisingly effective. Having calcium-containing foods alongside vitamin D sources supports the absorption pathway. This is not magic; it’s physiology working efficiently. And when meals include overall nutrients—protein, magnesium, vitamin K—bone health becomes less of a single-ingredient goal and more of a coordinated ecosystem.

Supplements: When They Help, How They Should Be Chosen
Supplements can be beneficial for people who struggle to reach targets through diet, who have malabsorption concerns, who avoid key food groups, or who have lab-confirmed vitamin D insufficiency. The crucial point is selection: not all supplements behave the same way.
Calcium supplements often come as calcium carbonate or calcium citrate. Calcium carbonate may work best when taken with meals, while calcium citrate is sometimes preferred when stomach acid is lower or tolerance is an issue. Vitamin D supplements typically come as vitamin D3 (cholecalciferol) or vitamin D2 (ergocalciferol). Many clinicians favor D3 due to its consistent performance, though both can raise levels.
Reading labels with intention matters. Look at elemental calcium (the actual calcium amount) rather than just the compound name. Also consider dosing strategy: splitting doses can improve absorption and reduce gastrointestinal side effects for some people.
A thoughtful supplement plan typically aligns with a goal: raise levels into an adequate range, then maintain. Supplements aren’t meant to replace healthy habits; they’re meant to complete the picture.
Testing and Timing: Knowing Your Baseline
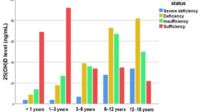
If you’re serious about “the right balance,” testing provides a baseline that diet alone can’t guarantee. A commonly discussed marker is 25-hydroxyvitamin D, which reflects vitamin D status. Calcium levels may also be evaluated, especially if there are symptoms or risk factors. Sometimes additional labs—such as kidney function or markers of bone turnover—may be considered in broader clinical contexts.
Timing matters too. If supplementation begins after a deficiency is discovered, rechecking levels may be recommended to confirm response. Seasonality can affect vitamin D: levels may dip in winter in many climates. Planning ahead reduces guesswork.
For readers who prefer structure, think of it as a cycle: assess, adjust, observe. The body tends to reward this kind of deliberate stewardship.
Beyond Bones: Muscles, Immunity, and Everyday Function
Calcium and vitamin D don’t only support the skeleton. Calcium is essential for muscle contraction and nerve signaling, which means it helps explain why adequate intake can influence strength, coordination, and the ability to recover after activity. Vitamin D, meanwhile, has immune-modulatory roles and may influence inflammation pathways.
This doesn’t mean supplements prevent every illness. But it does mean that bone health and overall vitality are linked. When readers feel steadier and more capable—when balance improves and aches lessen—that’s often the result of multiple factors aligning, with vitamin D and calcium playing supporting roles.
Daily movement strengthens the whole system. Weight-bearing exercises and resistance training provide mechanical signals that bones interpret as “construction required.” Nutrition supplies the materials. Together they form a feedback loop of resilience.
Common Pitfalls After 40: Myths, Mistakes, and Misconceptions
One common mistake is relying on supplements alone while under-eating calcium-rich foods. Another is assuming sunlight is automatically sufficient. Many people get indirect or insufficient exposure, particularly during winter months or when indoor work dominates the day.
There’s also a myth that “more is always better.” The body is precise. If calcium and vitamin D are taken in excess, the downstream effects can include elevated blood calcium or unwanted stress on organs like the kidneys in susceptible individuals. Another pitfall is inconsistent intake—taking supplements sporadically can lead to unstable vitamin D status.
Finally, readers sometimes ignore medication interactions. Certain drugs can influence calcium absorption or vitamin D metabolism. If you take long-term medication, discussing your plan with a healthcare professional is a quiet but important step.
A Practical Roadmap: Creating Your Personal Balance Plan
Start with three pillars: food foundation, sensible supplementation, and verification. Choose calcium-rich meals you can sustain. Add vitamin D through fortified foods and safe, realistic sunlight exposure when possible. If supplements are needed, select appropriate types and doses, then reassess when recommended.
Keep your routine cohesive. Pair nutrient timing with your meals. Maintain consistency. And remember that balance isn’t a single decision—it’s an evolving practice shaped by labs, lifestyle, and how your body responds over time.
After 40, the goal isn’t just to avoid a problem. It’s to cultivate momentum. When vitamin D and calcium are aligned, your bones don’t merely endure—they participate in the life you want to keep moving toward.