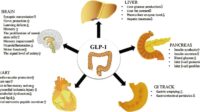
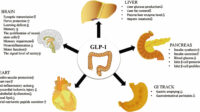
For years, GLP-1 has been discussed through the prism of glucose control—an elegant hormone with a tidy résumé in metabolism. Yet bone is not a passive backdrop. It is a living, responsive organ, constantly negotiating with muscle, immune signals, and endocrine cues. Then comes vitamin D, a molecule often treated like a mere “calcium helper.” What if, instead, vitamin D is more like a backstage conductor—tuning the cellular choreography that determines whether GLP-1’s metabolic benefits can ripple into healthier bones? Once you start thinking this way, the story becomes harder to dismiss and more intriguing to follow.
Reframing GLP-1: From Metabolic Messenger to Bone-Signaling Actor
GLP-1 (glucagon-like peptide-1) is widely known for its ability to enhance insulin secretion, suppress glucagon, and improve glycemic stability. But hormones rarely wear single-purpose costumes. The same signaling pathways that regulate energy availability can also influence osteoblast activity, osteoclast behavior, and the inflammatory milieu that shapes bone remodeling. Bone doesn’t just respond to “nutrients.” It responds to instructions—molecular directives delivered through receptors, second messengers, and transcriptional programs.
When GLP-1 exerts effects beyond the pancreas, it begins to resemble a cross-talk mediator. Picture bone cells as diplomats who interpret multiple languages at once: mechanical load, inflammatory cytokines, micronutrient status, and endocrine whispers. GLP-1 enters that multilingual conversation. The surprising part is not that it communicates—it’s that the quality of the conversation can depend on whether vitamin D is present in a supportive form.
Vitamin D as a Cellular Interpreter: Beyond Calcium
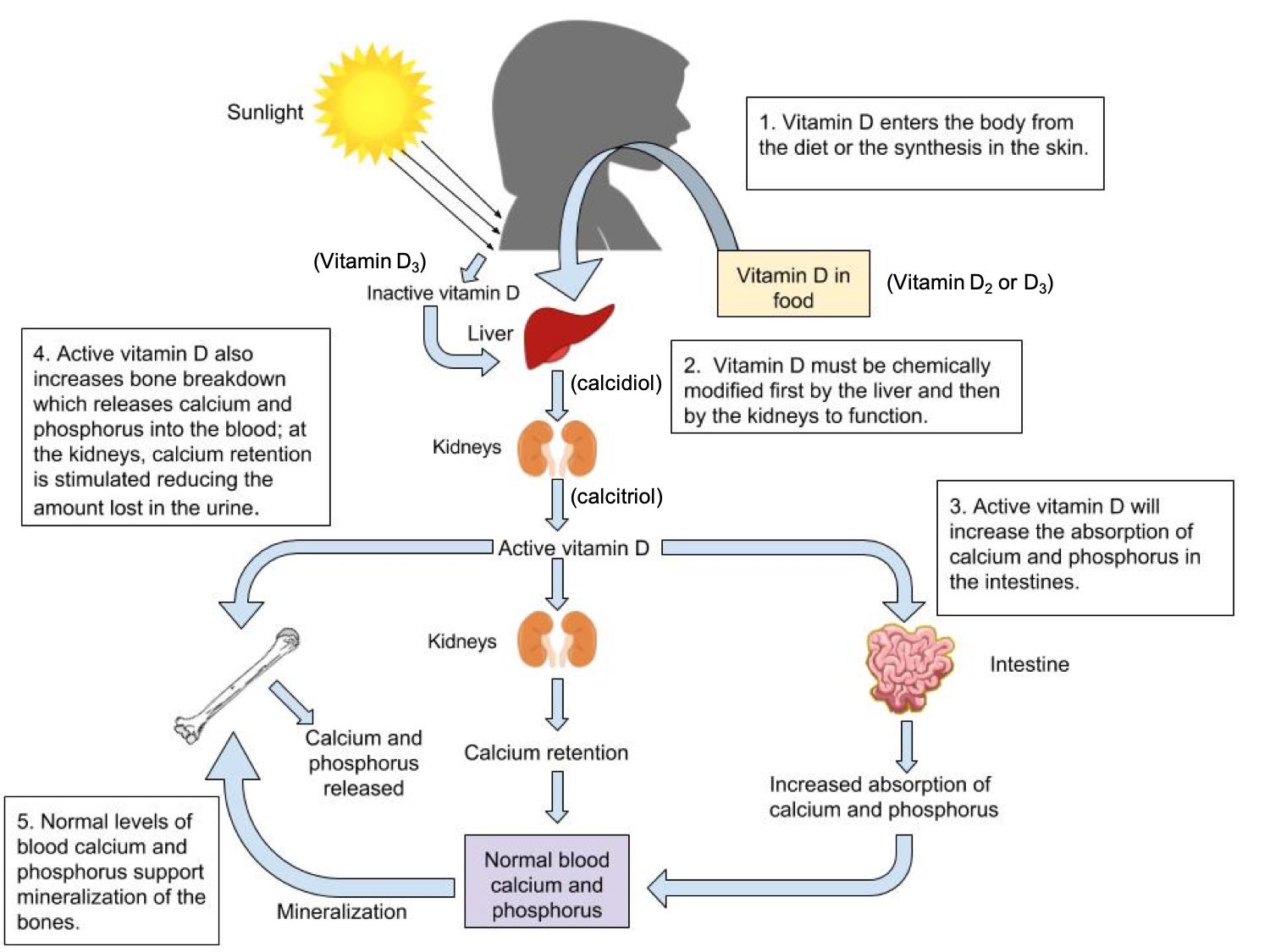
Vitamin D is often reduced to a single function: helping the body absorb calcium. That simplification is convenient, but it misses the broader, more fascinating reality. The active form of vitamin D—calcitriol—acts like a transcriptional regulator. It influences gene expression across many tissues, including those involved in musculoskeletal health. Bone remodeling is not a random sequence of breakdown and rebuilding; it’s a regulated cycle. Vitamin D helps determine the “tone” of that cycle by shaping differentiation signals and supporting a favorable endocrine environment.
In other words, vitamin D doesn’t merely supply building materials. It may influence whether bone-forming cells receive the right cues to mature efficiently, and whether bone-resorbing signals remain restrained. This matters because GLP-1’s broader impacts may require a receptive cellular landscape.
The Bone–Muscle–Immune Triangle: Where GLP-1 Finds Leverage
Bone health rarely depends on bone alone. Muscle contraction releases myokines; immune cells secrete inflammatory mediators; bone responds by altering remodeling rates. Vitamin D is deeply embedded in this triad. It can modulate immune tone, influence cytokine patterns, and support muscle function—each pathway potentially affecting the skeleton.
Now introduce GLP-1. Beyond metabolic effects, GLP-1 signaling can influence inflammatory pathways and alter how tissues communicate. If vitamin D reduces pro-inflammatory signals and improves functional muscle output, GLP-1 may find a smoother route to beneficial downstream effects in bone. The result could be a more harmonious remodeling balance—less collateral inflammation, more orderly repair.
GLP-1 and Bone Remodeling: Osteoblasts, Osteoclasts, and the Balance Question
Bone is maintained by a delicate equation: osteoblast-mediated formation versus osteoclast-mediated resorption. Disruptions in endocrine signaling can tilt this equation. If GLP-1 helps create a favorable signaling environment, it may encourage osteoblast activity and restrain osteoclast overactivation. But this is where vitamin D becomes unexpectedly pivotal. Vitamin D status may determine whether osteoblast precursors mature appropriately and whether osteoclast-related pathways respond with moderation rather than escalation.
Think of it like this: GLP-1 may provide the “goal” (a systemic shift toward healthier physiology), while vitamin D may help define the “terrain” on which bone cells operate. When vitamin D signaling is adequate, bone cells may be better equipped to interpret GLP-1-associated cues, enabling more coherent changes in remodeling.
Receptor Signaling and Intracellular Messaging: How Synergy Could Be Engineered
At the cellular level, endocrine effects are not magic; they are relay systems. GLP-1 exerts actions through receptor-mediated signaling that can trigger cascades influencing cell survival, inflammation, and differentiation. Vitamin D acts through its own receptor framework to regulate transcription and pathway responsiveness. When both signals converge—directly or indirectly—the combined effect could be more than additive.
Synergy may arise through shared pathway nodes: inflammation-related signaling networks, differentiation regulators, and gene expression programs that affect skeletal integrity. In such a scenario, vitamin D may enhance the stability of GLP-1 downstream signals, leading to a stronger functional outcome: healthier bone structure, reduced resorption pressure, and improved microenvironmental conditions for rebuilding.
Inflammation as a Hidden Architect: The Curiosity-Point
Here is a thought that changes the way the whole narrative feels: chronic low-grade inflammation is not simply “background noise.” It can alter bone remodeling by affecting both osteoblast and osteoclast systems. GLP-1 is often discussed in metabolic terms, but metabolic imbalance frequently travels with inflammatory signaling. Vitamin D, meanwhile, can influence immune modulation, potentially dampening inflammatory drivers.
If GLP-1 shifts metabolic signaling and vitamin D shifts immune tone, the bone microenvironment may become less hostile. Less hostility usually means better capacity for reconstruction. This is why the question becomes compelling: not whether GLP-1 affects bone, but whether vitamin D presence makes the effect more consistent, more resilient, and more biologically “usable.”
Muscle Function: The Indirect Path That Feels Like a Shortcut
Bones adapt to forces. When muscle weakens, mechanical loading changes, and bone loses some of the stimuli that encourage maintenance. Vitamin D supports muscle performance and neuromuscular function. That matters because GLP-1 therapies may influence weight, energy balance, and metabolic health—factors that indirectly shape muscle and activity patterns.
When vitamin D helps maintain muscle function, the organism can translate metabolic improvements into physical activity and mechanical benefit. In such a setting, GLP-1’s systemic effects may “stick” better because the body can actually use them—through movement, load-bearing, and functional recovery.
Practical Implications: A Shift from Correction to Optimization
For many people, vitamin D enters the conversation only after a lab result flags deficiency. But a more progressive viewpoint is emerging: rather than waiting for deficiency to appear, optimizing vitamin D status might support broader musculoskeletal and endocrine resilience. GLP-1’s benefits may be influenced by baseline nutritional signaling quality—especially in tissues where vitamin D acts as a regulator rather than merely a nutrient.
This does not mean vitamin D is a standalone solution. It suggests a framework: consider vitamin D as a contextual amplifier for skeletal benefits when GLP-1 pathways are being engaged therapeutically. The most promising outcomes often occur when multiple systems—metabolic, inflammatory, and musculoskeletal—align.
What Still Invites Wonder: Measuring Outcomes Beyond the Usual Metrics
Bone health is multifaceted. Conventional markers can miss subtle remodeling shifts that ultimately affect fracture risk and structural integrity. A future-facing approach would look at how vitamin D status modifies GLP-1-related changes in bone turnover, microarchitecture, and inflammatory profiles. It’s one thing to observe improved glucose control. It’s another to confirm that bone tissue experiences meaningful, sustained advantages.
Curiosity belongs here: not merely whether vitamin D and GLP-1 interact, but how consistently, through which pathways, and in which populations. Individual biology—baseline vitamin D stores, inflammatory burden, activity level, and hormonal context—could determine whether the synergy is modest or transformative.
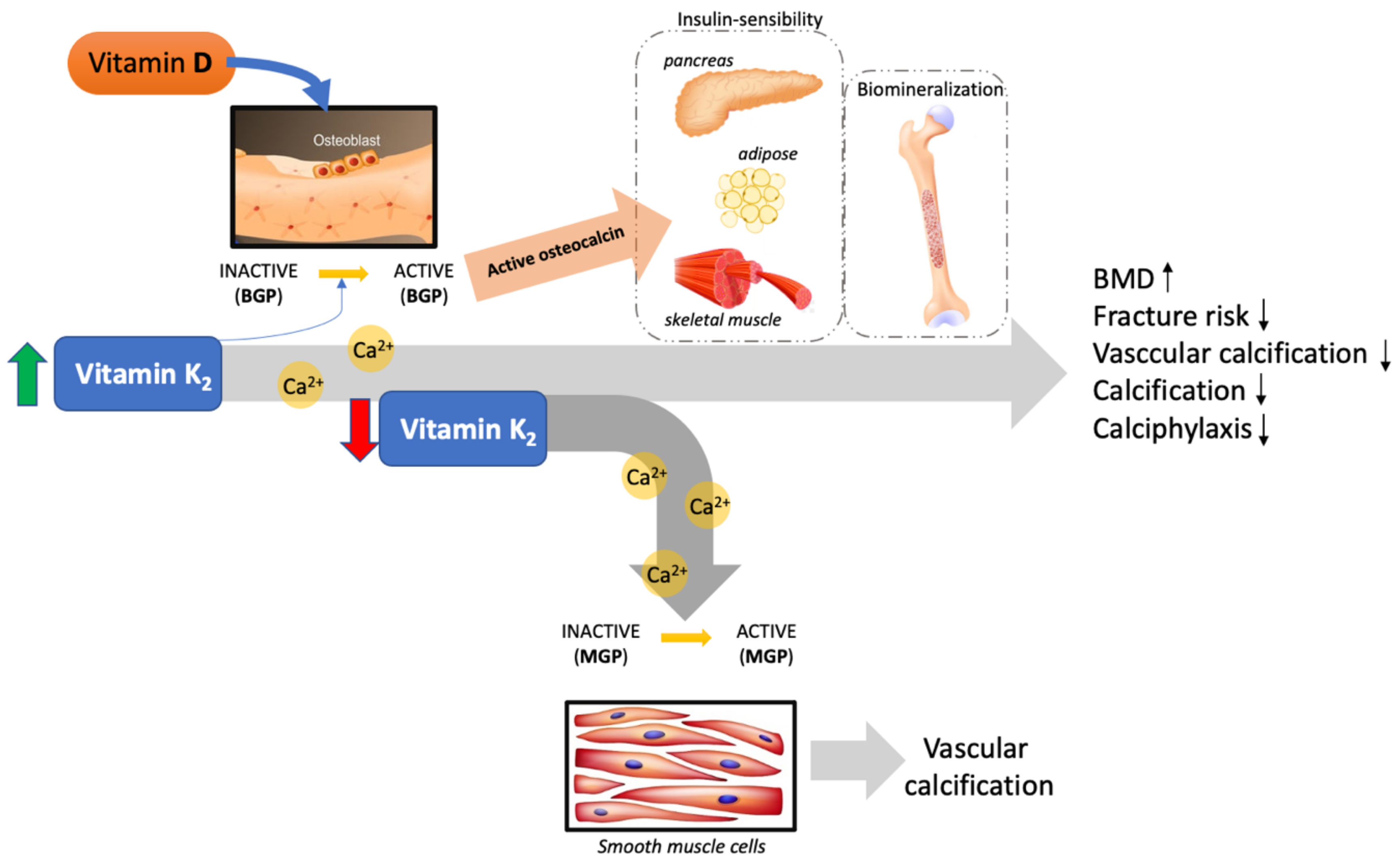
Closing Perspective: The Skeleton as an Endocrine Receiver
Think of the skeleton as an endocrine receiver rather than an inert scaffold. GLP-1 speaks to the body’s metabolic state, but bone interprets those signals through the lens of local and systemic regulators—including vitamin D. When vitamin D is present at supportive levels, GLP-1’s downstream communications may land more effectively: remodeling may become more balanced, inflammation may be less disruptive, and muscle-supported loading may reinforce skeletal stability.
In the end, the most compelling shift is not just scientific. It’s philosophical. We stop asking only, “What does GLP-1 do?” and start asking, “In what physiological context does GLP-1 perform best?” Vitamin D may be one of the key contexts—turning bone from a bystander into an informed participant in metabolic recovery.