Have you ever noticed how some seasons feel like a revolving door for sniffles—no sooner does one cold fade, another one arrives? The mind often reaches for the obvious culprits: crowded transit, sleepless nights, stress, the seasonal “mood” of viruses. But what if the more subtle story is happening underneath—within the immune system’s quiet machinery—where one nutrient, surprisingly, can quietly tip the balance? Low vitamin D may be that overlooked tipping point. And the most intriguing part is that the connection isn’t just about getting sick; it’s about how your body orchestrates readiness before exposure even happens.
Vitamin D: More Than Bone Nutrition
Vitamin D has a reputation—sometimes deservedly, sometimes reductionistly—confined to bones. Yet in reality, it functions like a molecular coordinator. It influences immune cells, modulates inflammatory signaling, and helps determine whether the body’s early defenses respond with alacrity or hesitation.
Think of your immune system as a stage crew. Viruses are the actors who show up and demand attention. But vitamin D is part of the crew that checks the lights, tightens the ropes, and keeps the performance from collapsing. When vitamin D is low, that backstage work may run sluggishly.
This is why the link between low vitamin D and frequent colds can feel counterintuitive. You’re not “caught” because of a lack of willpower or hygiene alone. Instead, your internal conditions may be less prepared, more reactive, and less capable of swift, calibrated responses.
The Immune System’s “Readiness Mode”
Frequent colds often involve a cycle: exposure, viral entry, and then the body’s attempt to contain the threat. If the early immune response is delayed or underpowered, viruses can gain a foothold. Vitamin D appears to play a role in how effectively certain immune defenses activate and coordinate.
There are two ways this can manifest. First, you may get sick more often. Second, the colds may linger longer, with symptoms that feel stubborn or relentless. The pattern isn’t always dramatic—sometimes it’s subtle: “Why do I always end up with something in winter?”
It’s not that vitamin D acts as a shield that blocks every cold. Rather, it may help shift your immune response into a more efficient, less chaotic rhythm.
Why Winter Makes the Problem More Likely
Winter doesn’t only bring more viral circulation. It also changes your vitamin D landscape. Less daylight means less skin production. Cloud cover and shorter days can reduce the opportunity for vitamin D synthesis, especially for people who spend most time indoors.
Then there’s the layering effect: people dress warmer and spend more time indoors, which can further reduce sunlight exposure. Add lifestyle variability—different work hours, geographic latitude, seasonal routines—and vitamin D deficiency can quietly become an annual guest.
That’s where curiosity turns into relevance. If you’ve noticed an uptick in colds when the weather turns, low vitamin D could be one of the unseen threads tying together multiple seasonal variables.
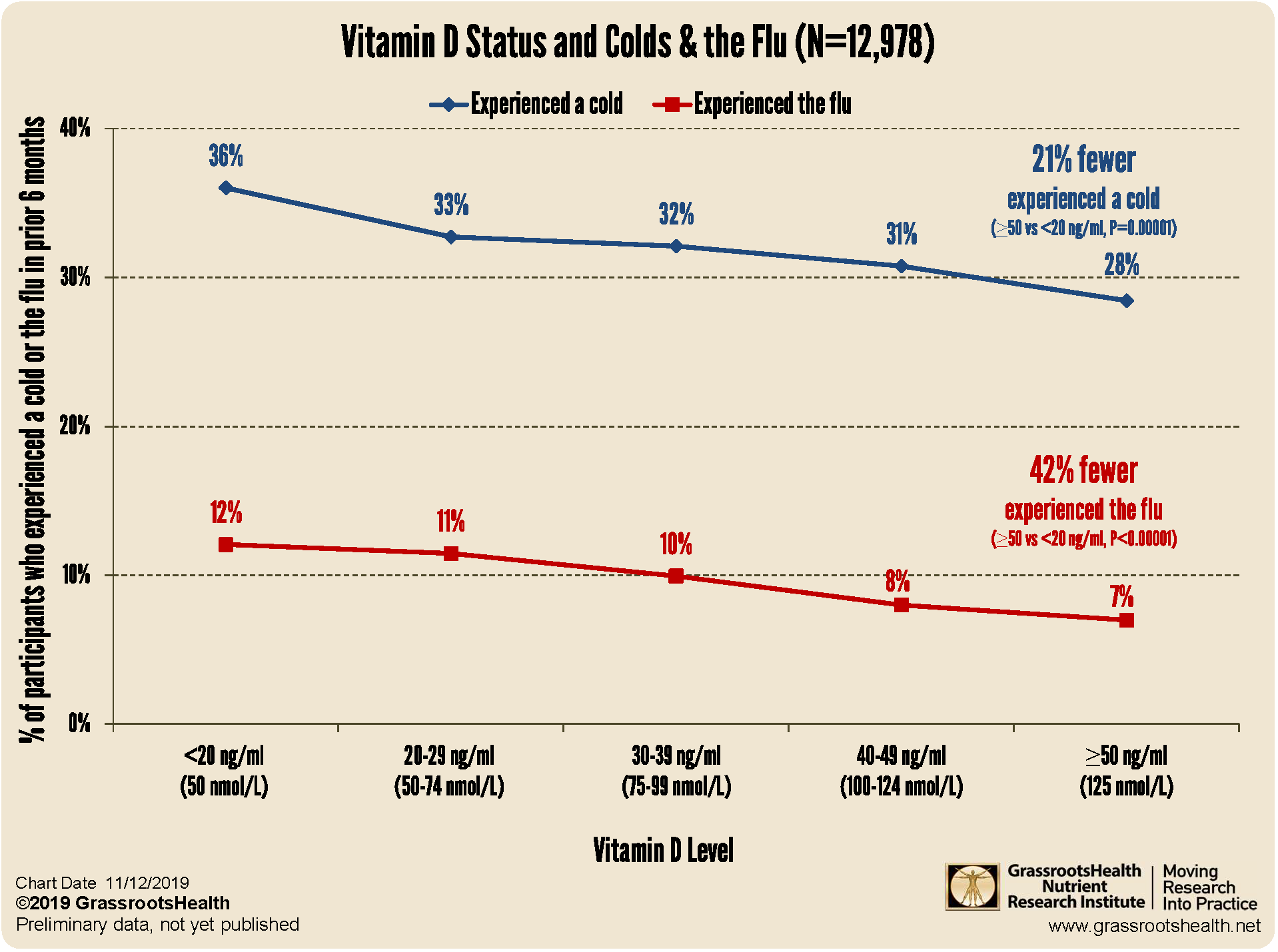
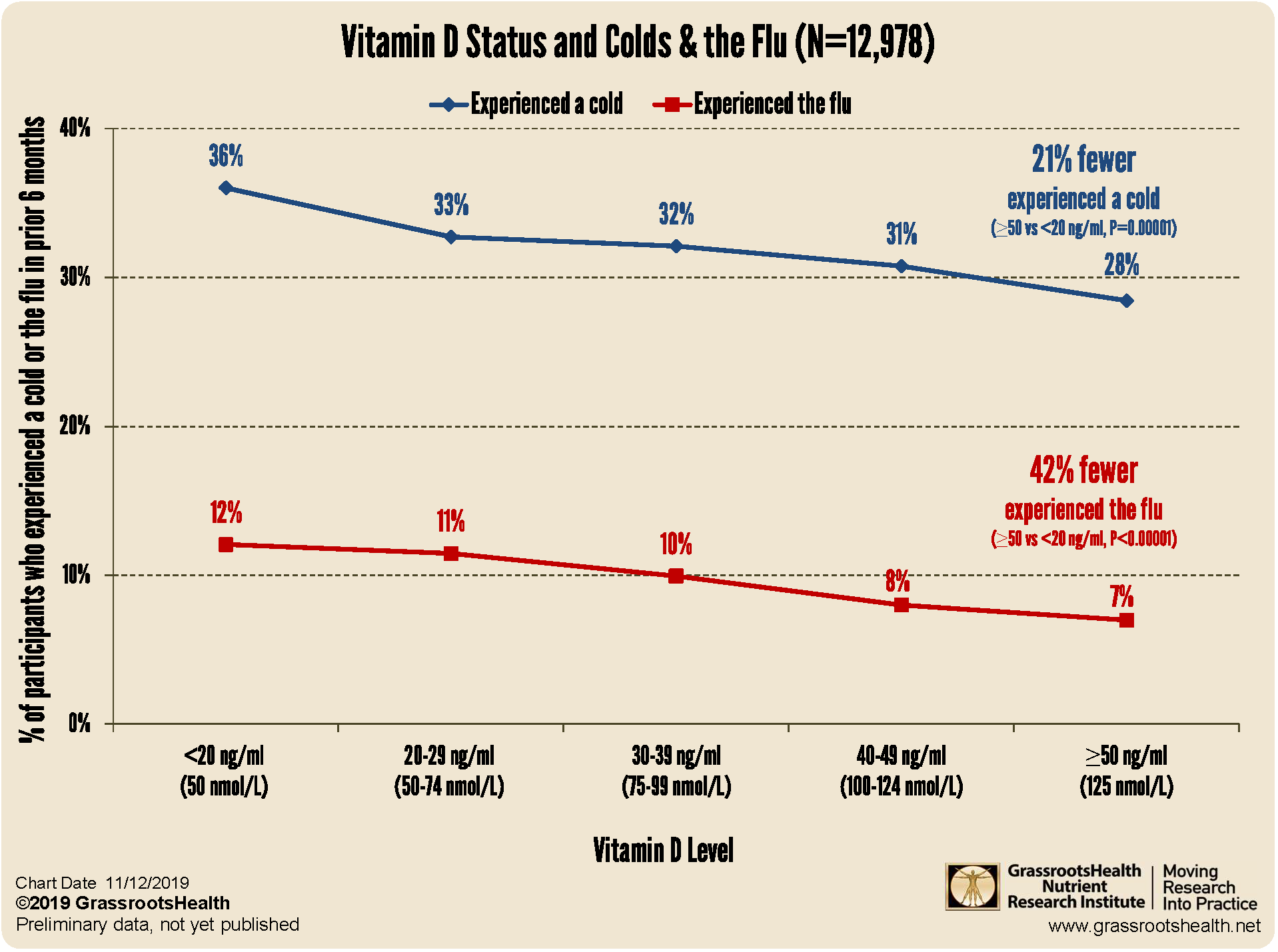
Low Vitamin D and Frequent Colds: What the Pattern Suggests
The association between low vitamin D levels and increased respiratory infections has been reported repeatedly, and it’s not hard to see why people find the idea compelling. It offers a plausible biological pathway and doesn’t require a dramatic leap of faith.
If vitamin D helps orchestrate immune readiness, then consistently low levels could contribute to a higher probability of infection and perhaps a less resilient recovery. It’s like running a car with slightly underinflated tires: nothing immediately catastrophic happens, but performance and stability quietly degrade over time.
Of course, correlation isn’t destiny. Frequent colds can come from many sources. Yet the vitamin D connection remains notable because it’s actionable. You can measure it, adjust it, and re-evaluate.
Symptoms and Signs: When Deficiency Feels Like More Than Tiredness
Vitamin D deficiency doesn’t always announce itself with a single, obvious signal. Some people feel fatigue. Others notice muscle weakness or vague aches. Mood can also shift—sometimes into a flat, low-spark feeling that seems “seasonal” but lasts longer than weather should justify.
And yes, you might also notice an immune pattern: repeated minor illnesses, longer durations, or a frequent “one after another” sensation. This combination—general sluggishness paired with recurrent infections—can be a hint worth investigating.
While these signs aren’t exclusive to vitamin D deficiency, they can provide a narrative thread. A body doesn’t always speak in one language. It often mixes dialects: fatigue, discomfort, and immune turbulence.
Who Is Most at Risk of Low Vitamin D?
Certain groups are more likely to have lower vitamin D levels. People who rarely get sun exposure—due to indoor lifestyles, sunscreen use without adequate sun time, or living in areas with limited sunlight—are commonly affected.
Skin pigmentation can influence how much vitamin D is produced from sunlight. Seasonality also matters, as do body weight and dietary patterns. Additionally, some medical conditions can reduce absorption or alter vitamin D metabolism.
If you recognize yourself in several of these categories, it’s not a reason for alarm. It’s a reason for attention. The surprising link between low vitamin D and frequent colds becomes more meaningful when deficiency risk is elevated—because it turns a vague possibility into a testable hypothesis.
How to Check: The Case for Measuring Instead of Guessing
Instead of relying on hunches, consider measuring. A blood test can evaluate your vitamin D status, often using a marker known as 25-hydroxyvitamin D. This approach transforms the narrative from “maybe” to “known.”
Once you have results, you can talk with a clinician about an individualized plan. That plan might include dietary strategies, sensible sunlight exposure, and supplementation.
Measuring isn’t just clinical—it’s psychological. It replaces swirling uncertainty with clarity. And clarity tends to reduce the frantic sense of “Why am I always getting sick?”
Supplementation: A Shift from Hope to Strategy
For many people, supplementation is the most direct route to improve vitamin D status, particularly during winter months. But the key word is strategy, not “shotgunning” random doses.
Vitamin D supplementation should be tailored. Factors like baseline levels, diet, absorption, and overall health can influence what’s appropriate. Some individuals require higher repletion; others need maintenance.
It can feel strangely comforting to approach winter with a plan rather than a prayer. You’re not simply waiting for viruses to arrive. You’re adjusting internal conditions to support resilience.
Beyond Vitamin D: The Support Network That Matters
Vitamin D is not a lone hero. If the immune system is a stage crew, then vitamin D is only one member of the crew—important, yes, but not the only one.
Sleep quality, stress management, balanced nutrition, hydration, and appropriate movement all interact with immune performance. Hygiene helps reduce exposure. Avoiding smoke exposure can reduce irritation to respiratory tissues. And adequate protein supports tissue maintenance, including immune cell function.
So the shift in perspective is this: vitamin D can be a foundational lever, but it works best alongside other health behaviors. The goal isn’t perfection. It’s synergy.
What Results Might Look Like If You Improve Vitamin D
Imagine this: instead of a winter calendar filled with recurring coughs, you experience fewer colds—or at least, fewer interruptions. Some people notice improved general well-being after correcting deficiency: more energy, fewer lingering aches, and a calmer sense of physical steadiness.
Immune changes can be gradual. Your body needs time to rebuild biochemical readiness. That’s why consistency matters more than dramatic short-term effects. Vitamin D isn’t an instant rescue remedy; it’s a tuning adjustment.
When you couple measured supplementation with ongoing healthy habits, the story can shift. The question becomes less “Why do I keep getting sick?” and more “What internal factors can I optimize?”
When to Talk to a Clinician (and Why It’s Worth It)
If you have a history of recurrent infections, chronic fatigue, malabsorption issues, kidney problems, or you’re taking medications that affect vitamin D metabolism, it’s especially important to seek medical guidance. The goal is not only to raise levels but to raise them safely and appropriately.
Also, avoid treating symptoms as proof. Low vitamin D can be one factor, not the only explanation. Clinical conversation helps separate overlapping causes and reduces the risk of incorrect dosing or missed underlying issues.
That professional check-in can also provide reassurance. It turns the process into an evidence-informed journey rather than a guessing game.
A New Winter Story: More Than Avoiding Germs
There’s a quieter, more hopeful way to think about winter health. Instead of seeing colds as a random punishment for being human, you can see them as events your immune system tries to prevent or limit. Low vitamin D may represent one modifiable condition that influences how well that prevention works.
So here’s the invitation: measure, adjust, and observe. If your colds have been unusually frequent, vitamin D could be part of the explanation—and part of the solution. When you change the inputs, the immune system can respond differently. And that shift in perspective—toward strategy rather than surrender—can be its own kind of resilience.