After 40, your body becomes less forgiving. Bone remodeling still happens, but the balance often tilts—slower formation, comparatively faster resorption, and a quieter decline in calcium absorption. In that delicate window, vitamin D steps in as a silent conductor. It helps your gut absorb calcium, supports mineralization, and influences muscle function that protects your skeletal frame. But the question many readers ask is deceptively simple: which vitamin D is “best”—D3 or D2? The most useful answer isn’t about a universal winner. It’s about selecting the form that fits your physiology, your routines, and your long-term bone health strategy.
Why Vitamin D Becomes a Bone-Health Priority After 40
Bone health isn’t only about bones. It’s also about the biochemical choreography around them. Vitamin D contributes to a cascade of events: it supports calcium uptake in the intestine, helps maintain adequate serum calcium and phosphate levels, and provides a foundation for proper mineral deposition in bone matrix.
With age, several factors can conspire. Skin synthesis of vitamin D declines, dietary patterns may change, and time spent outdoors can reduce sunlight-driven vitamin D production. Additionally, some people experience reduced intestinal efficiency, meaning even when vitamin D is present, the downstream absorption signals may not be as robust.
This is where vitamin D supplementation—or better-targeted forms of vitamin D—can matter. Bone-related concerns can feel remote early on, but they become increasingly tangible after midlife, especially for those with low sun exposure, dietary gaps, or a family history of osteoporosis.
D3 vs D2: The Chemistry Behind the Choice
Vitamin D comes in two common forms: vitamin D2 (ergocalciferol) and vitamin D3 (cholecalciferol). They sound similar, but the body processes them differently.
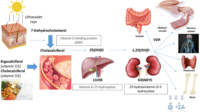
D3 is naturally produced in the skin under ultraviolet light and is structurally aligned with the form your body evolved to generate. D2, in contrast, is typically derived from plant or fungal sources. Both can raise circulating vitamin D levels, yet many clinicians prefer D3 for consistency and biological affinity with human pathways.
Think of D3 as the more familiar “key” to the same lock your body uses. D2 can still open doors, but the fit may be less seamless for some people.
How Each Form Works: Absorption, Conversion, and Activity
When you ingest vitamin D, your liver converts it into a storage form, and then the kidneys (and other tissues) help convert it into the active hormone-like compound that drives calcium handling and musculoskeletal function.
Both D2 and D3 travel through the same general metabolic lanes. However, differences in persistence—how long vitamin D levels remain elevated—and in potency across individuals can influence which form performs better in real-life conditions. Some people notice steadier improvement with one form; others respond similarly. That variation is often shaped by baseline deficiency, body composition, adherence, and metabolic factors.
After 40, these differences can feel sharper because vitamin D sufficiency is harder to maintain. Your starting point matters. If levels are low, the “best” choice becomes the form that elevates and sustains status most reliably for your body.
Bone Health Outcomes: What Readers Should Pay Attention To
Vitamin D is not a stand-alone bone treatment. Bone outcomes depend on a matrix of nutrients and behaviors—calcium intake, protein sufficiency, resistance training, and adequate vitamin K status are key supporting players.
Still, vitamin D plays a measurable role in fracture risk reduction pathways indirectly. It strengthens the substrate for calcium incorporation, helps preserve muscle strength and coordination, and may reduce fall risk by improving functional performance. And fewer falls means fewer bone injuries—an outcome that often resonates more with real life than laboratory numbers.
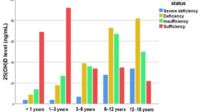
When evaluating vitamin D forms, focus on markers like 25-hydroxyvitamin D levels, but also on how you’re functioning: stamina, grip strength, balance confidence, and reduced muscle “fuzziness” that can come from deficiency.
Which Is “Best” for Most People: D3 Often Leads
For many adults over 40, vitamin D3 is commonly favored because it tends to be more effective at maintaining adequate vitamin D status. That matters, since bone remodeling is not a sprint; it’s a long, slow process measured in months and years.
In practical terms, a reliable maintenance strategy can be more valuable than occasional “catch-up” dosing. When vitamin D levels stay in a comfortable range, calcium handling becomes more consistent, and the body can allocate more resources to stable mineralization rather than compensatory adjustments.
Still, “most people” is not “everyone.” Some readers may do very well with D2, especially if they’ve used it consistently and their levels remain appropriate. The best choice is the one that keeps you sufficient with good adherence and minimal side effects.
When D2 Might Still Make Sense
D2 isn’t automatically inferior in every context. People who prefer plant-derived options, those using specific prescription regimens, or individuals who already have stable lab results on D2 may find it perfectly workable.
Another scenario is supply-driven practicality: some markets and product lines stock D2 more widely. If your clinician recommends D2 and your vitamin D levels remain adequate over time, there’s no reason to abandon a regimen that’s doing its job.
However, the key phrase is “remain adequate.” With D2, some people may experience faster declines between doses, which can necessitate more careful monitoring. If you choose D2, it’s wise to be vigilant about follow-up labs and consistency.
Dosing Patterns: Daily, Weekly, or Intermittent
Bone health does not care only about form—it cares about pattern. Daily dosing can be gentler, helping maintain steadier blood levels. Weekly dosing may offer convenience without sacrificing stability for many people.
Intermittent or high-dose approaches can be appropriate in certain deficiency-correction plans, but they require careful medical guidance. Too much—too soon—or dosing that doesn’t match metabolism can create volatility in blood levels, which is less ideal for long-term maintenance.
Regardless of whether you choose D3 or D2, the best strategy usually aligns dosing frequency with your lifestyle and your ability to stick to the routine. Consistency is the quiet superpower of supplementation.
Absorption Allies: How to Make Vitamin D Work Harder
Vitamin D is fat-soluble, so it often performs better when taken with meals that contain some dietary fat. Readers who take supplements on an empty stomach may find effectiveness inconsistent—particularly if their overall diet includes limited fat.
Magnesium and vitamin K are frequently discussed in bone-health circles because they participate in calcium transport and bone metabolism pathways. While vitamin D sets the stage for absorption, the supporting cast helps ensure the absorbed calcium is properly utilized.
In everyday language: a strong vitamin D plan is easier to sustain when it’s integrated into a balanced routine, not treated as an isolated pill detached from food and lifestyle.
Who Should Be Extra Careful After 40
Some people should treat vitamin D decisions as a clinician-guided project. Those with kidney disease, a history of kidney stones, granulomatous disorders (like sarcoidosis), hyperparathyroidism, or certain medication regimens may require tailored dosing and monitoring.
Also, individuals with malabsorption conditions—celiac disease, inflammatory bowel disease, or bariatric surgery history—may need higher or differently structured supplementation strategies. In these cases, the form may matter, but monitoring matters even more.
If you’ve ever experienced unusual calcium levels, bone density changes, or persistent fatigue, it’s reasonable to connect supplementation to a broader health assessment rather than guessing.
What Content Readers Can Expect From a Smart Plan
Beyond the form comparison, a strong bone-health article should include practical checkpoints. Readers benefit from content that covers lab interpretation basics, dietary context, and lifestyle levers like strength training. Some readers prefer a narrative style—why the transition after 40 feels harder, what happens internally, and how to rebuild confidence through small consistent actions.
Others want a decision framework: quick comparisons of D3 vs D2, dosing pattern options, and “when to re-test” suggestions. A third group appreciates scenario-based guidance—vegans, low-sun lifestyles, people with recurrent deficiency, and those focusing on fall prevention.
In a complete resource, even the less glamorous topics like adherence, meal timing, and monitoring intervals deserve attention. Bone health is built from habits, not headlines.
Realistic Next Steps: Choosing D3 or D2 With Confidence
If you’re building a bone-health routine after 40, consider starting with assessment: know your baseline vitamin D status through blood testing when possible. From there, choose the form that aligns with your preferences and your response pattern. For many adults, D3 is the intuitive choice for sustained sufficiency, while D2 can work well when it keeps levels in the right range.
Then, anchor the plan in behavior: take the supplement with a meal that includes fat, pair it with adequate calcium and protein, and support it with weight-bearing and resistance training. Your bones don’t respond to supplements alone—they respond to mechanical signals and nutritional readiness.

Bottom Line: The Best Vitamin D Form Is the One That Keeps You Sufficient
D3 vs D2 is ultimately a question of effectiveness, stability, and fit. For many people over 40, vitamin D3 tends to be the more reliable workhorse for maintaining adequate levels, supporting calcium absorption and bone mineralization over time. D2 can still be a valid option—especially when it’s tolerated well and maintains appropriate blood levels.
Ultimately, the “best” form is not a trophy winner. It’s a dependable partner in your long-term bone strategy—one that supports consistent sufficiency, integrates smoothly into daily life, and is reinforced by labs, nutrition, and movement.