There’s a quiet irony in modern weight loss: drugs can help shrink the body’s measurements, yet they may unintentionally tug at the scaffolding that holds it up. Bone density—the mineralized architecture behind strength—doesn’t get its due attention in most conversations. But step back for a moment. What if the same biochemical pathways that influence appetite, energy balance, and fat metabolism also touch the bone remodeling cycle? And what role does vitamin D play in this story, especially when weight-loss medications enter the scene?
Weight Loss Drugs and the “Hidden Metabolism” of Bones
Weight loss isn’t merely a reduction in body mass. It is a renegotiation of hormones, inflammation patterns, nutrient availability, and mechanical loading. Bones are not inert; they’re living tissue undergoing constant remodeling. Osteoclasts resorb, osteoblasts rebuild, and the balance between these processes determines bone density.
Some weight loss medications alter pathways related to appetite and glucose homeostasis. Others influence gastric emptying or signaling molecules that can echo through the skeleton indirectly. The result can be subtle: a drift in vitamin and mineral status, changes in inflammatory tone, or shifts in how the body handles calcium absorption.
Here’s the perspective shift that invites curiosity: even when fat mass declines, the body may still be “resource-constrained.” Bones require a dependable supply of calcium and the biochemical signals that help calcium become usable. Without those signals, the remodeling cycle can start to wobble.
Bone Density 101: The Remodeling Rhythm You Can’t See
Bone density reflects more than strength—it mirrors the quality and organization of mineral deposits. Think of it like a city’s construction schedule. You can’t judge the city by its skyline alone; you need to understand what’s happening underground: the ongoing demolition and rebuilding.
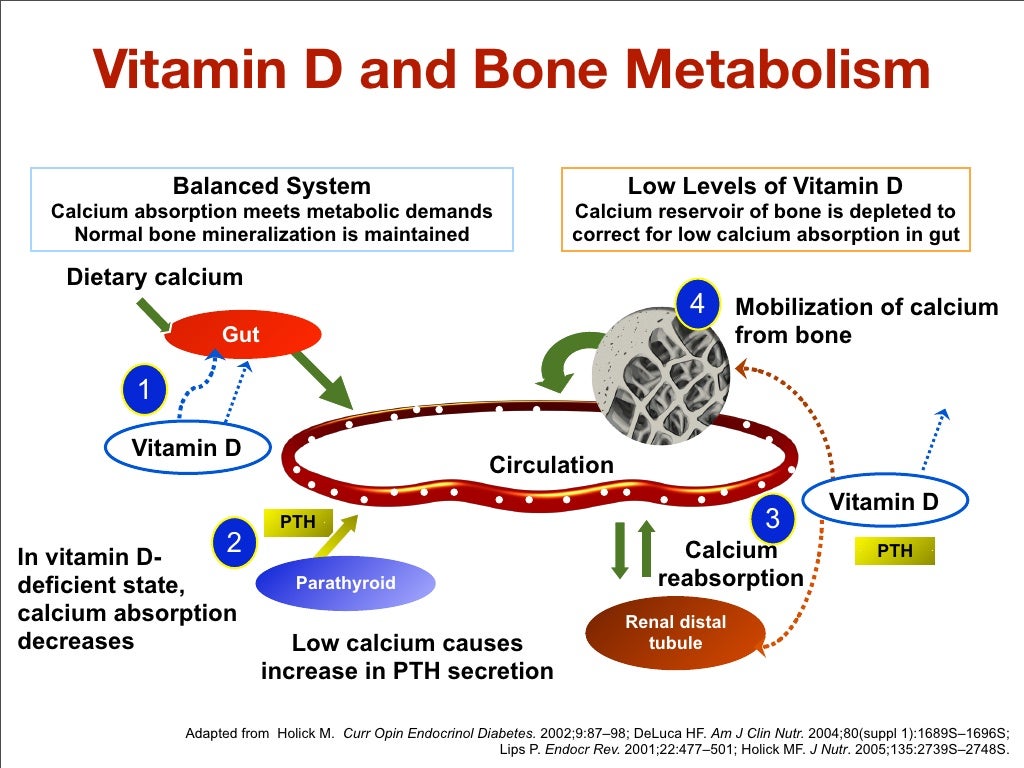
Vitamin D becomes central in this municipal metaphor. It supports intestinal absorption of calcium and helps regulate serum calcium and phosphate. When vitamin D is insufficient, calcium absorption can drop. That doesn’t always cause immediate symptoms. Sometimes it shows up later, as bone mineral density declines over time.
Then comes the twist: weight loss medications may prompt changes in diet, appetite, or gastrointestinal function. Even small reductions in nutrient intake, repeated consistently, can compound. Over months, bones may receive fewer building blocks than they need.
Why Vitamin D Is the Keystone: Beyond “Sunshine Vitamin” Lore
Vitamin D is often treated like a wellness buzzword, but its role is biochemical and precise. When vitamin D levels are adequate, calcium absorption rises, and mineralization proceeds more efficiently. When levels are low, the body compensates—sometimes by increasing parathyroid hormone activity—steering calcium away from bone formation and toward maintaining blood calcium levels.
That compensation might be invisible at first. A person may feel fine, yet their skeleton might be slowly losing mineral density. Bone is slow to change, which makes early prevention more valuable than rescue.
If weight loss is the headline, vitamin D is the backstage crew: it doesn’t always get attention, but it makes the performance possible.
Calcium, Vitamin D, and the “Completeness” of Bone Nutrition
Vitamin D doesn’t operate alone. Calcium is the raw mineral used to strengthen bone. But pairing matters. Calcium intake without adequate vitamin D can blunt absorption. Vitamin D without calcium can also fail to achieve optimal mineralization. The body needs both the ingredient and the delivery system.
During weight loss, many people unintentionally reduce portions of dairy, fortified foods, legumes, or other calcium-rich options. Even when protein is prioritized, calcium can be overlooked. This is where a shift in perspective helps: weight loss plans often focus on calories; bones need minerals.
Consider this as a practical curiosity: ask not only, “Am I losing weight?” but also, “Am I supplying my bones with the minerals required to stay structurally confident?”
How Reduced Intake Can Ripple Through the Skeleton
When appetite changes—whether from medication, behavioral adaptation, or dietary changes—total nutrient intake can decline. The body may receive fewer calories, but also fewer micronutrients. Vitamin D status is particularly vulnerable because it depends on dietary sources and sunlight exposure, and it is not typically “guaranteed” by food alone.
Even if vitamin D intake seems reasonable, absorption and metabolism matter. Gastrointestinal effects from certain weight loss drugs may alter how efficiently nutrients are utilized. Less efficient absorption can turn borderline vitamin D levels into a clinically meaningful deficiency.
Long sentences sometimes hide the truth; short ones make it sharper: bones cannot borrow calcium and vitamin D from thin air.
Mechanisms That Invite Concern—and Questions
Bone health during pharmacologic weight loss can be influenced by multiple overlapping mechanisms. Mechanical loading changes as body weight decreases, and that can reduce the stimuli that encourage bone maintenance. Hormonal shifts—such as changes in insulin sensitivity and inflammatory markers—may also influence bone remodeling dynamics.
There’s also the question of adipokines: molecules produced by fat tissue that can affect inflammation and metabolism. As adipose mass shrinks, signaling patterns shift. Bones respond to the biochemical climate, not just the number on a scale.
This is why a curiosity-driven approach is useful. Instead of assuming weight loss is automatically bone-friendly or bone-harming, it’s more accurate to ask: “What is happening to nutrient availability, remodeling balance, and mineralization efficiency?”
Signs, Symptoms, and the Problem of Silent Deficiency
Low vitamin D can be remarkably silent. Some people experience generalized aches, muscle weakness, or fatigue. But others have no obvious clues. Bone density loss is gradual; by the time it’s measurable, years of remodeling imbalance may have accumulated.
That’s a crucial psychological detail: waiting for symptoms can mean arriving late. Preventive strategies—especially for people starting weight loss medication—can shift outcomes before declines become irreversible.
Impatience is understandable when weight loss feels urgent. Yet bone health rewards foresight.
Testing and Monitoring: Turning Uncertainty into Clarity
The most confident action usually begins with measurement. Clinicians may evaluate vitamin D status through blood tests and assess relevant markers related to calcium balance. Bone density testing can be considered for individuals at higher risk—such as those with prior fractures, prolonged low vitamin D levels, or certain medical conditions.
Monitoring isn’t about fear; it’s about precision. Weight loss plans can be adjusted based on how the body responds, and bone health can be treated as a dynamic parameter rather than a distant afterthought.
Curiosity becomes strategy when data replaces guesswork.
Supplementation: When Vitamin D Becomes a Plan, Not a Wish
Vitamin D supplementation is not one-size-fits-all. Dosage and duration depend on baseline levels, dietary intake, sun exposure, and individual risk factors. The goal is to reach and maintain an adequate vitamin D range that supports calcium absorption and bone mineralization.
Supplement plans are often paired with attention to calcium intake. Dietary calcium sources—fortified beverages, yogurt, cheese, leafy greens, legumes, and certain fish—can complement supplements when appropriate.
There’s a quiet lesson here: supplementation is a tool. Used wisely, it can reinforce the body’s remodeling rhythm while weight loss medications do their job.
Exercise as the Bone’s Feedback Loop During Weight Loss
Weight loss changes body composition, but bones prefer stimuli. Resistance training, weight-bearing activities, and balance-focused movement can support bone maintenance by applying mechanical loading. This is not merely fitness; it’s communication with the skeleton.
Think of exercise as a metronome. It provides regular signals that encourage rebuilding and help counteract remodeling imbalance. Even if fat mass decreases, the skeleton can still receive the mechanical “permission” to stay strong.
Short sessions done consistently can matter. The bone responds more to repetition than to intensity in many cases, especially for maintaining density.
Who Should Be Extra Mindful?
Certain groups may need more careful bone-focused planning: older adults, people with history of fractures, individuals with malabsorption syndromes, those with kidney or parathyroid disorders, and anyone with documented vitamin D deficiency. Also, consider the duration of medication use—longer exposure heightens the value of proactive monitoring.
If weight loss is medically supervised, bone health discussions should be part of the same care pathway. The body is not separate compartments; it’s a coordinated system.
Ask the important questions early, not after a year has passed.
Bringing It Together: A New Perspective on “Healthy Weight”
Healthy weight loss isn’t only about reaching a target number. It’s about preserving the infrastructure that supports movement, posture, independence, and resilience. Bone density is one of the most literal forms of long-term health: it determines how safely the body can withstand the years ahead.
Vitamin D is the pivot point in this narrative. It supports calcium absorption, helps regulate mineral balance, and underwrites the mineralization process. When vitamin D is neglected during pharmacologic weight loss—especially alongside reduced intake or lifestyle changes—bone density may quietly pay the price.
But the story doesn’t have to end with risk. With monitoring, adequate vitamin D and calcium support, and bone-friendly exercise, weight loss can become a transformation that strengthens rather than compromises. The scale changes; the skeleton can, too—staying ready for life’s next chapter.