Have you ever noticed how your legs can feel perfectly fine in the afternoon—then, as evening settles in, a dull ache blooms beneath the skin? It can feel stubborn, sometimes rhythmic, sometimes oddly restless. You might stretch, sip water, change positions, and still the discomfort finds a way back. Now imagine the possibility that what you’re attributing to “just getting older” may be signaling something more subtle—something biochemical, systemic, and often overlooked. In this story, we’ll explore why leg pain at night can sometimes travel with low vitamin D, and why a shift in perspective can be more illuminating than any quick fix.
Nighttime Leg Ache: A Pattern With a Hidden Logic
Leg pain that intensifies at night rarely behaves like a simple strain. It often arrives when you’re still—when movement slows and muscles relax into a familiar posture. That detail matters. It suggests the discomfort isn’t merely mechanical; it may be neuromuscular and metabolic, hovering at the boundary between sensation and regulation.
Some people describe it as deep soreness. Others call it burning, tingling, throbbing, or an “electric” restlessness. The terminology varies, but the timing is strikingly consistent. When symptoms cluster around bedtime, the body’s daily rhythms become a key character in the narrative. Hormones shift. Inflammation fluctuates. Oxygen demand changes. And vitamin D—known for roles in calcium balance and immune modulation—may indirectly influence how muscles and nerves behave.

Vitamin D: More Than a Sunlight Supplement
Vitamin D is often reduced to a single idea—“get more sun.” But vitamin D is also a molecular communicator. It acts like a backstage director, influencing gene expression and supporting the scaffolding of calcium metabolism. Calcium, in turn, is essential for proper muscle contraction and nerve signaling.
When vitamin D is insufficient, the body may struggle to maintain an efficient calcium equilibrium. That can translate into muscle tenderness, weakness, or spasmodic sensations—especially when your system is already winding down for sleep. The night becomes the stage where minor imbalances become easier to notice.
Think of vitamin D as an orchestrator. Without it, the symphony doesn’t stop—it just plays with more friction, more discord, and a subtle sense of effort.
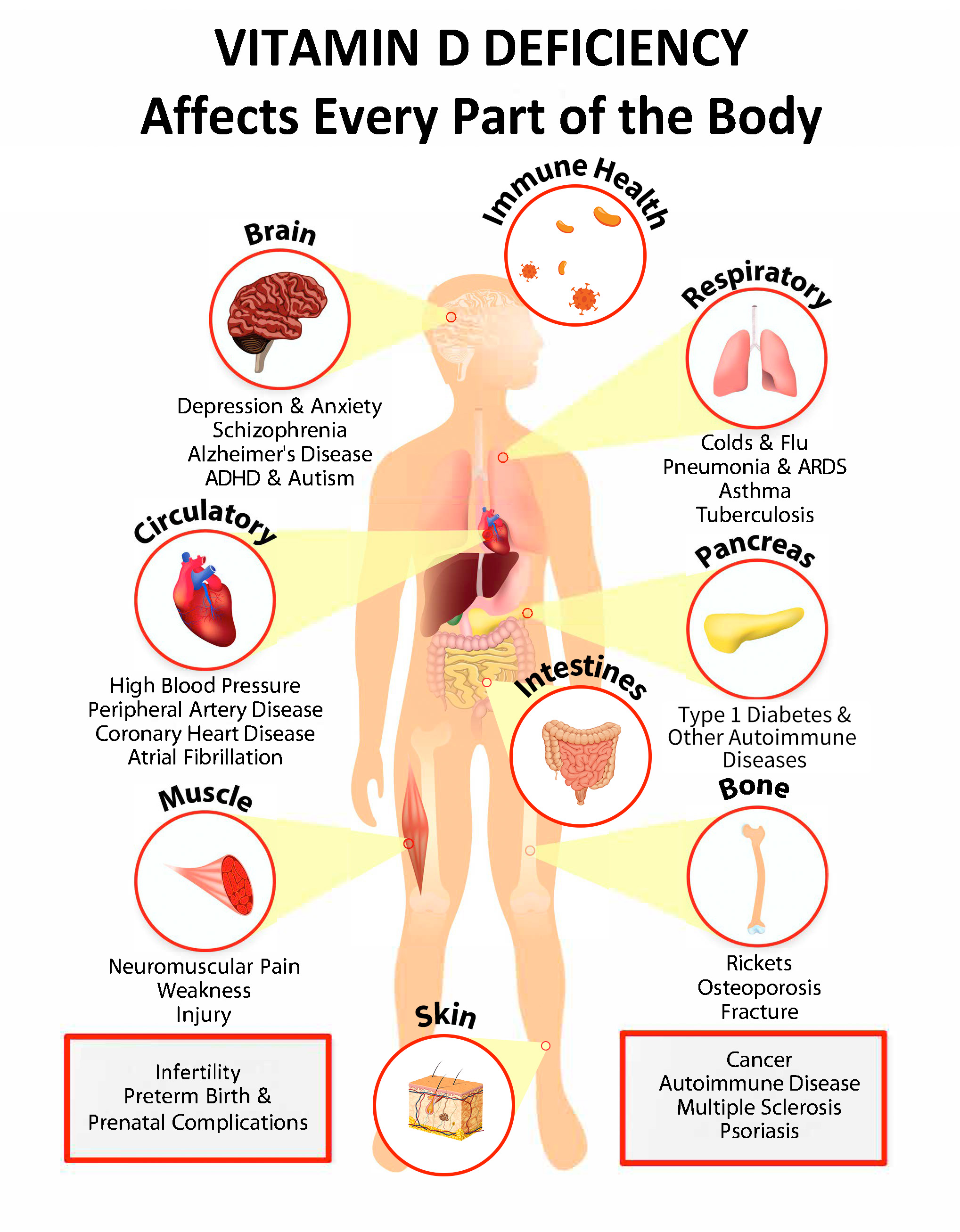
How Low Vitamin D Can Translate Into Leg Discomfort
Muscles and nerves are not isolated organs. They are part of a web of signaling pathways. Vitamin D’s involvement in these pathways is one reason a deficiency can appear in unexpected places.
When vitamin D is low, the body can become more prone to muscular aches. Calcium handling may become less predictable. That unpredictability can contribute to cramps, soreness, and restless sensations—particularly in the legs, where circulation and muscle activity are prominent during daily movement and may reveal symptoms when rest begins.
There’s also the immune dimension. Vitamin D is intertwined with inflammatory signaling. If inflammation subtly increases, muscles may feel more sensitive. A night of stillness can then amplify the perception of discomfort.
In short: vitamin D deficiency doesn’t always announce itself as “bone pain.” Sometimes it whispers through your legs at bedtime.
The “Invisible Clues” That Often Travel With Deficiency
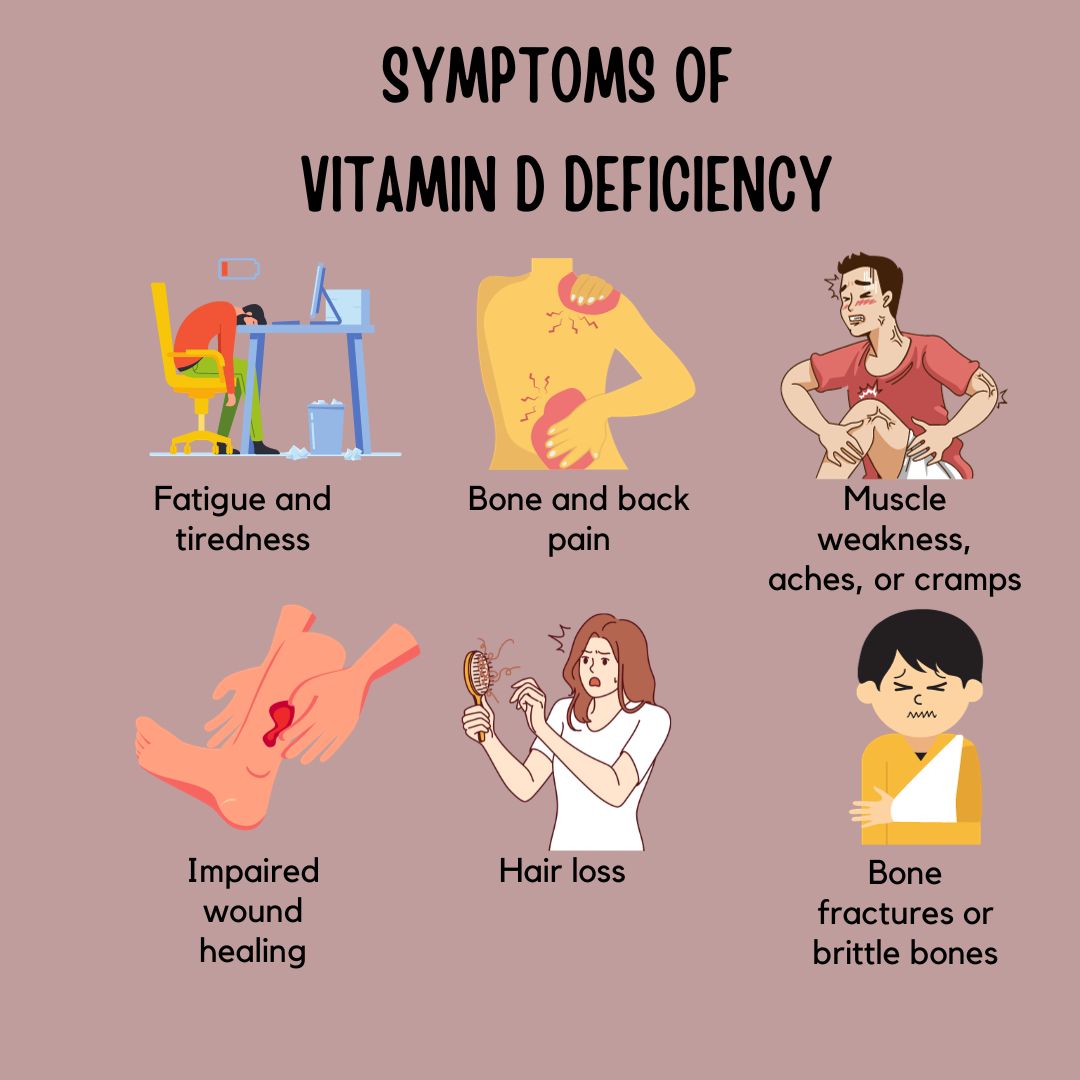
Leg ache is only one potential sign. Vitamin D deficiency can present as a mosaic of small symptoms that don’t always point to a single cause. You might notice fatigue that feels disproportionate to your sleep. You might experience vague body aches, reduced resilience after activity, or a sense that recovery takes longer.
Some people report weakness, mood changes, or increased susceptibility to illness. Others discover the pattern only after lab testing reveals unexpectedly low levels.
Skin can also provide hints. While no symptom is diagnostic alone, vitamin D deficiency has been associated with certain skin-related concerns. The body is constantly adapting, and the adaptations can look like unrelated issues until you connect the dots.
:max_bytes(150000):strip_icc()/VWH-JulieBang-VitaminDDeficiency-txt-4000x2700-25d3aac6e3914cf98d08db2ba4d87be2.png)
Restless Legs vs. Crampy Pain: Two Roads, One Destination
Not all night leg discomfort is identical. Restless legs syndrome (RLS) tends to bring an irresistible urge to move, often accompanied by creepy-crawly sensations. Cramping pain feels more like a sudden tightening or sustained spasm. Still, the boundary between them can blur in real life.
Low vitamin D may contribute to muscular sensitivity, while RLS has its own common associations, including iron deficiency in many cases. That means you could have overlapping mechanisms: one driving restless sensations, another increasing musculoskeletal vulnerability.
Here’s the useful perspective shift: treat nighttime leg discomfort as a signal, not a single-label diagnosis. That framing encourages comprehensive assessment rather than guesswork.
Why Nighttime Makes Everything Feel Worse
During the day, you move, shift positions, and distract your brain with tasks and environment. At night, those inputs fade. Sensory perception becomes more prominent. Muscles may stiffen slightly. The nervous system, unoccupied by motion, may “scan” for discomfort.
Additionally, hydration and electrolytes—like calcium and magnesium—can influence the likelihood of cramps. Vitamin D participates indirectly in calcium regulation, so a deficiency can make the whole balance more fragile.
It’s not that vitamin D magically “turns on” at bedtime. It’s that bedtime is where small biochemical issues become noticeable because nothing else is competing for attention.
How to Think About Testing: Turning Curiosity Into Clarity
If your legs ache at night, especially alongside other possible deficiency hints, laboratory evaluation can transform speculation into information. A blood test measuring 25-hydroxyvitamin D is often used as a marker for vitamin D status. That test doesn’t guarantee the cause of leg symptoms—but it can reveal whether vitamin D is a plausible contributor.
Many clinicians also consider related factors, such as calcium status, magnesium, kidney function, and sometimes iron studies if restless sensations dominate. This broader evaluation is valuable because nighttime leg discomfort is frequently multifactorial.
In other words, curiosity is useful, but confirmation is powerful.
What About Supplements? Safety, Timing, and Realistic Expectations
Vitamin D supplementation may help some people, but it should be approached thoughtfully. Dosing matters, because vitamin D is fat-soluble and accumulates. Too little may do nothing; too much can create problems. The best plan is guided by test results and professional recommendations.
Timing can also play a role. Many people take vitamin D with a meal containing fat to enhance absorption. If your legs are already aching nightly, you might be tempted to “fix it immediately.” Yet the body often requires time to replenish stores, recalibrate pathways, and reduce musculoskeletal sensitivity.
Expectations should be gentle but honest: improvement may be gradual. If symptoms worsen, diversify, or involve swelling, numbness, or significant weakness, medical evaluation becomes essential.
Supporting Your Muscles Tonight: Practical Steps While You Investigate
While you explore vitamin D status, consider supportive measures that address the immediate experience of night discomfort. Gentle calf stretches, slow leg massage, and careful posture changes can reduce tension. Warmth—like a warm shower or heating pad—may relax muscle tone. Hydration and consistent electrolytes can also help some people, especially if cramps are prominent.
These steps won’t replace proper evaluation, but they can reduce suffering now. Think of them as scaffolding: temporary structure while the deeper cause is clarified.
When to Treat This as Urgent, Not Routine
Most nighttime leg ache is manageable, but certain red flags deserve prompt attention. Seek care if you have one-sided swelling, redness, warmth, sudden severe pain, shortness of breath, or neurological symptoms like persistent numbness or progressive weakness. Those signs can indicate conditions unrelated to vitamin D.
The goal is not fear—it’s precision. Vitamin D deficiency is one possibility, not a universal explanation for every symptom.
A New Perspective: Listening to the Body’s Night Signals
Leg ache at night can feel like an inconvenience, a nuisance, or a normal part of aging. But a more curious lens turns it into a message: your body might be hinting at nutritional imbalance, muscular sensitivity, or regulation issues that surface when the lights go out.
If vitamin D deficiency is in the picture, addressing it can sometimes shift the entire trajectory of discomfort—quietly, gradually, and with less drama than you’d expect. And even if vitamin D isn’t the only cause, the act of investigating can still be transformative.
Your legs may ache at night, but they can also guide you toward better understanding—one bedtime signal at a time.