What if a single sun-derived nutrient could help your body do the quiet work of repair after a hip replacement—while also acting as a future-minded guardrail? It sounds almost too whimsical, doesn’t it? Yet vitamin D is anything but frivolous. It’s a hormone-like micronutrient that choreographs calcium balance, bone remodeling, muscle function, and immune behavior. And when you’re recovering from hip surgery—or trying to reduce the risk of frailty-related setbacks later—those roles can become surprisingly consequential.
Why hip replacement recovery is more than “just healing”
Hip replacement recovery is not a single event. It’s a sequence of coordinated biological tasks that must happen in the correct order: inflammation settles, tissues knit, bone integrates around the implant, and muscles regain strength without tipping into overuse. The body has to manage calcium transport, remodel bone at the right tempo, and preserve functional mobility.
Here’s the playful challenge: imagine your hip as a stage where every performer depends on timing. If vitamin D is in short supply, the lighting director forgets a crucial cue. Calcium absorption becomes less efficient, muscle contraction may feel slightly “thinner,” and the bone-building process can slow. Even mild deficiency can nudge the recovery curve in an unhelpful direction.
Vitamin D’s backstage role: calcium, bone metabolism, and implant integration
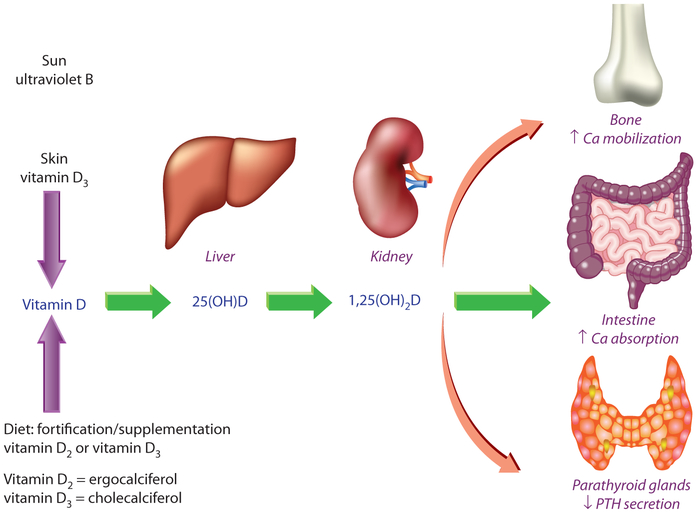
Vitamin D supports intestinal absorption of calcium and helps maintain adequate serum calcium and phosphate—ingredients needed for mineralization. After hip replacement, mineralization and remodeling aren’t abstract concepts; they’re the difference between a stable, well-integrated reconstruction and a slower, less resilient recovery.
Vitamin D also interfaces with osteoblast and osteoclast signaling—the team responsible for laying down bone and removing old material. This balance is essential because bone around the implant must adapt to mechanical loading. Too little vitamin D can tilt the metabolic ledger toward weaker mineralization and less robust structural maintenance.
Pre-operative preparation: treating vitamin D like an essential ingredient, not an afterthought
Before surgery, clinicians often assess overall risk factors: nutrition, activity level, comorbidities, and sometimes vitamin D status. Pre-operative vitamin D optimization can be particularly relevant for people who have limited sun exposure, darker skin pigmentation, malabsorption disorders, or are older adults with reduced skin synthesis.
Many people don’t realize how quickly deficiency can accumulate. Winter months, indoor routines, and consistent sunscreen use can all reduce cutaneous production. Add in dietary constraints, and vitamin D status may drift downward without obvious symptoms.
Think of pre-operative planning as a rehearsal. If the rehearsal room lacks a critical prop, the performance suffers later. Vitamin D is that prop—often understated, frequently overlooked.
Recovery phase: how vitamin D may support strength and mobility
Muscle function is a major storyline in post-hip replacement recovery. Vitamin D plays a role in muscle performance, including muscle fiber function and neuromuscular coordination. When vitamin D status is adequate, muscle strength may improve more reliably alongside physical therapy.
That doesn’t mean vitamin D is a replacement for exercise. It’s more like the fuel that helps training translate into results. After surgery, physical therapy already asks your body to rebuild. Vitamin D helps ensure the rebuilding materials—particularly calcium-related systems—are available for muscle and bone to work harmoniously.
A small practical question can guide behavior: are you treating rehab as the entire effort, or are you supporting the biology that makes rehab effective? The second option is usually the more strategic one.
Prevention mindset: beyond surgery to long-term bone resilience
Hip replacement is a milestone, not an endpoint. The long-term goal is to preserve mobility, protect the remaining joints, and minimize falls. Falls risk is influenced by balance, muscle strength, vision, medications, and—yes—bone and muscle health.
Vitamin D contributes to a bone environment where remodeling remains efficient. It also supports muscle function, which is key for balance and safe ambulation. Over time, adequate vitamin D can help reduce the likelihood of fracture-related consequences, especially when paired with adequate calcium intake and resistance-oriented conditioning.
In a sense, vitamin D is preventive medicine with a slow-burning fuse. Its effects may not be dramatic on day one. But over months and years, it can support a steadier foundation.
Signs of deficiency (and why they’re easy to miss)
Vitamin D deficiency can be oddly silent. Some people experience generalized aches, fatigue, or muscle weakness. Others notice nothing until a bone density issue appears or a fracture occurs after a minor fall.
Because symptoms are non-specific, the “detective work” often relies on lab testing rather than guesswork. If you’re planning hip surgery or are already in the recovery window, asking about vitamin D screening can be a smart, proactive move—especially if you have risk factors such as older age, limited outdoor time, or conditions affecting absorption.
Testing and target ranges: aligning plans with real physiology
Clinicians often evaluate vitamin D status using serum 25-hydroxyvitamin D. This measurement provides a snapshot of vitamin D availability that can guide supplementation decisions. The goal is not to chase an arbitrary number—it’s to reduce deficiency and support normal biological functioning.
Different individuals may need different dosing strategies. Some benefit from higher short-term repletion, while others do well with maintenance dosing. The most effective plan is individualized and considers kidney function, calcium levels, dietary intake, and medication interactions.
After all, a well-designed recovery plan is less about maximalism and more about precision.
Supplementation strategies: typical approaches and common considerations
Vitamin D is often taken as D3 (cholecalciferol) because of its reliable effectiveness. Dosing regimens vary—some people use daily amounts, while others take intermittent higher doses under guidance.
Calcium intake is frequently paired with vitamin D, since calcium is the structural partner that vitamin D helps absorb and utilize. However, calcium should be considered thoughtfully. It’s best to align with dietary intake and clinician recommendations, particularly for individuals with kidney stone history or certain cardiovascular risk considerations.
Practical tip: taking vitamin D with a meal that includes fat can improve absorption. This turns an ordinary pill into a better-conducted intervention.
Safety and the “too much” question
Vitamin D is powerful, but it’s not infinite. Excessive vitamin D can raise calcium levels, potentially leading to complications such as hypercalcemia. This is why supplementation should not be a casual guessing game.
If you’re already taking vitamin D through a multivitamin, fortified products, or separate supplements, it matters to total your intake. Monitoring—when appropriate—can help ensure that the intervention remains within a safe and effective window.
The challenge becomes: can you be consistent without overdoing it? That balance is the hallmark of a responsible recovery strategy.
Pairing vitamin D with rehab: an integrated, resilient routine
Vitamin D should be integrated into a broader framework: physical therapy, safe strengthening, gait training, pain management, and fall-prevention habits. Bone and muscle respond best when nutrition and movement are coordinated.
One elegant approach is to treat your recovery as a three-part equation: supplementation for biology, exercise for function, and environmental adjustments for safety. When those elements align, progress tends to feel less sporadic and more dependable.
When to talk to your clinician
If you have upcoming hip replacement surgery, a history of fractures, malabsorption concerns, chronic kidney disease, or you’re taking medications that can affect vitamin D metabolism, a conversation is especially warranted. Even without symptoms, vitamin D status may influence how smoothly recovery unfolds.
Ask about testing, dosing targets, and how to coordinate vitamin D with calcium and your rehabilitation plan. That conversation can turn uncertainty into a clear pathway.
A final playful reminder: will you support your hip’s “materials” today?
Hip replacement recovery is often framed as grit and physiotherapy. Those matter immensely. But consider this: vitamin D is the quiet collaborator that helps your body handle calcium, maintain muscle function, and sustain bone remodeling. The playful question becomes practical—will you simply wait for healing, or will you help your body build better conditions for it?
With thoughtful testing, a clinician-guided supplementation strategy, and a rehab plan that keeps moving forward, vitamin D can become more than a nutrient. It can become part of your long-term prevention story—one where recovery isn’t only repaired, but reinforced.