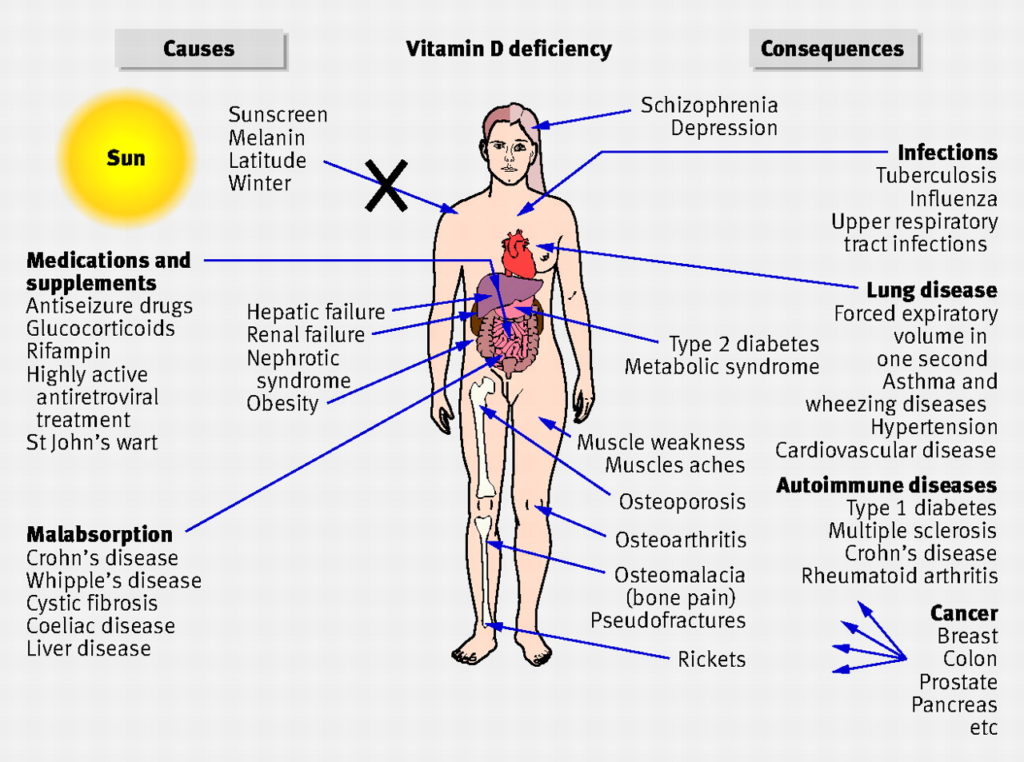
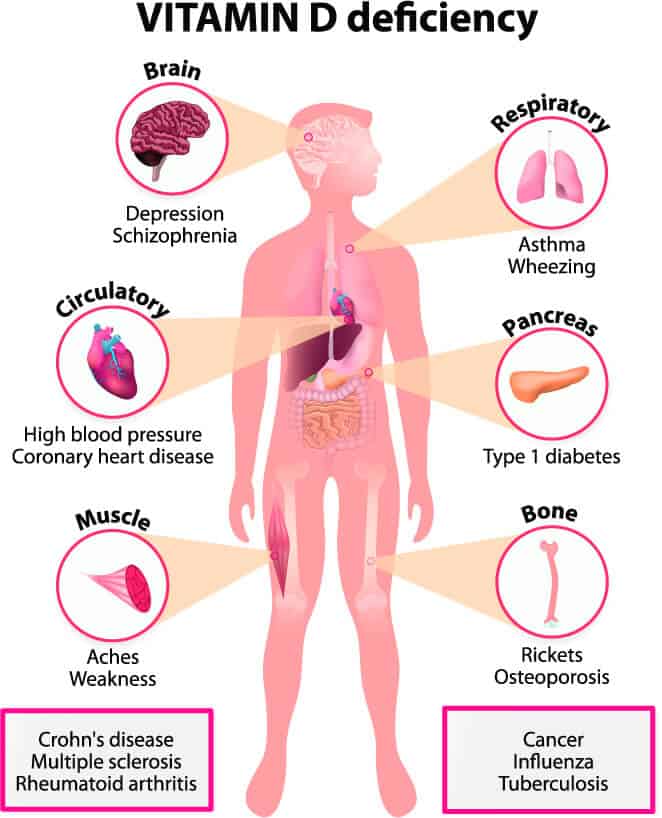
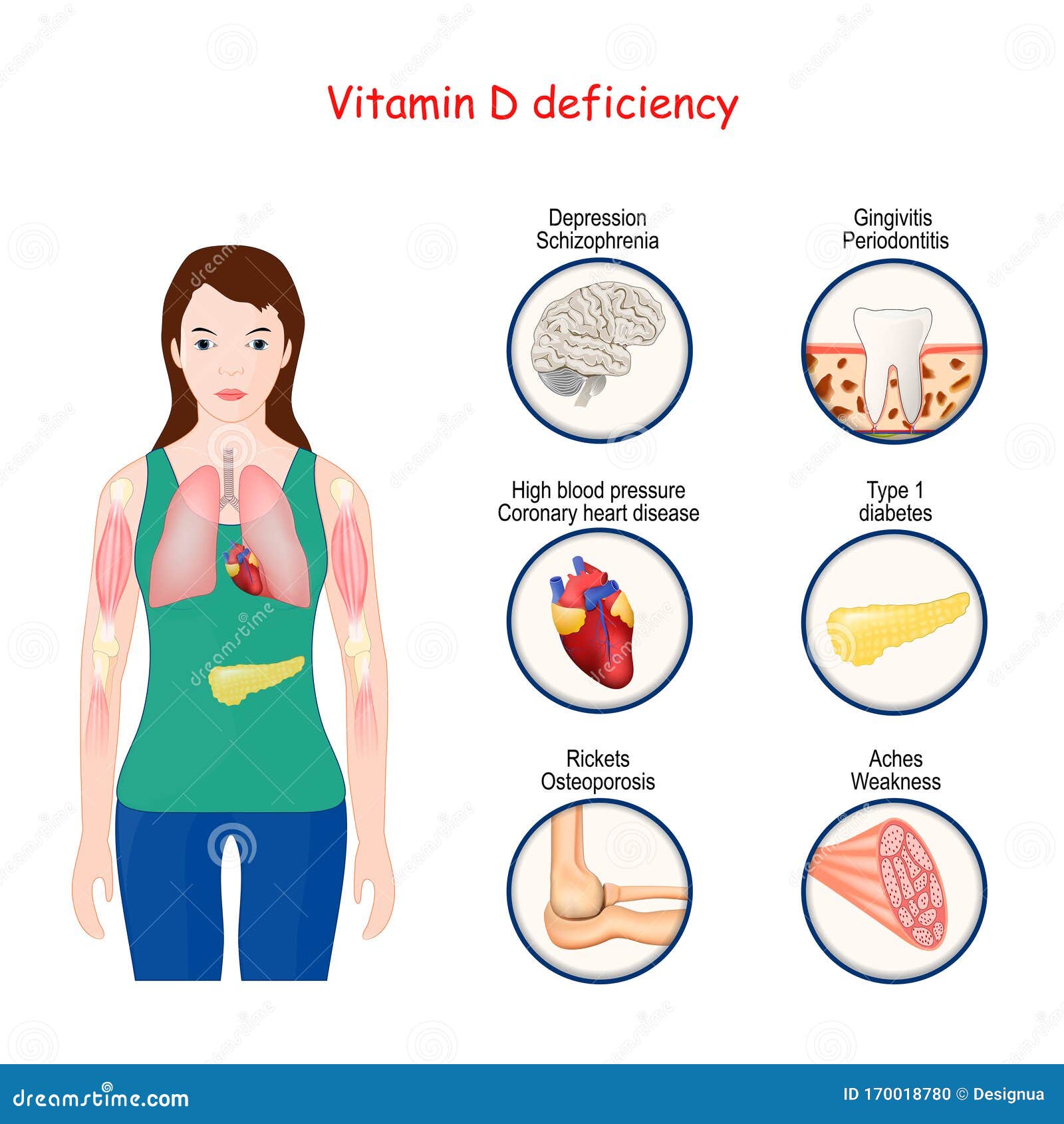
In the human body, vitamin D is less a “vitamin” and more a quiet conductor—standing just behind the curtain, shaping how music becomes movement. Yet when vitamin D levels sink, especially in people carrying extra weight, the orchestra can sound strangely muted. Symptoms may arrive like fog at dawn: subtle at first, then undeniable. This is why recognizing vitamin D deficiency in overweight individuals matters—not only for comfort, but for the integrity of everyday energy, bone strength, mood, and immunity.
Why Extra Weight Can Turn Vitamin D Into a Vanishing Resource
Imagine vitamin D as sunlight captured in a bottle. Now imagine that bottle stored in a cluttered attic filled with heavy boxes. The light is still present, but its accessibility diminishes. In overweight individuals, vitamin D can become sequestered in adipose (fat) tissue, effectively reducing the amount available for circulation and use. The body may hoard what it can’t easily deploy, leaving critical systems under-rehearsed.
This dynamic can produce an unusually persistent pattern: deficiency risk rises not simply because less sunlight reaches the skin, but because the body’s internal “distribution logistics” become less efficient. The result is not always dramatic illness. Often it is a slow, incremental deterioration of resilience—like a bridge that creaks before it cracks.
Fatigue That Feels Unreasonable for the Schedule
Fatigue is common, but vitamin D deficiency has its own flavor. It often feels out of proportion—sleep doesn’t fully restore it, and energy dips may appear even after a “normal” night. In overweight individuals, this can be especially perplexing: they may already be managing metabolic strain, yet the fatigue intensifies as if an extra weight has been placed on the nervous system.
Some people describe a low-grade exhaustion that lingers. Short errands can feel like workouts, and motivation becomes curiously brittle. Long sentences of productivity collapse into fragments. This isn’t laziness; it’s the body searching for missing cues that help muscles and energy pathways function smoothly.
Muscle Weakness and Achy Discomfort: The Body’s Low-Volume Alarm
Vitamin D supports muscle function and neuromuscular coordination. When it’s low, the alarm may not be a loud siren. It can appear as aching limbs, heaviness in the legs, and a sense that muscles “don’t respond” the way they used to. Overweight individuals may interpret these sensations as merely the consequence of carrying extra weight, but deficiency can sharpen the discomfort and prolong recovery.
There may be tenderness or vague soreness, particularly in the thighs, hips, or back. The body’s movements can start to feel less agile, as though the joints have lost some of their lubricating confidence. Think of vitamin D as part of the body’s internal scaffolding—without enough of it, stability becomes harder to maintain.
Bone Pain, Cracking Suspicions, and the Quiet Approach of Osteomalacia
When vitamin D deficiency persists, bones can behave like brittle architecture. People may notice bone pain in the lower back, pelvis, ribs, or legs. In more severe cases, osteomalacia (softening of bones) can develop, bringing increased fragility and an aching, persistent discomfort that seems to echo across movement.
Overweight individuals sometimes underestimate this risk because they assume soreness always has a mechanical origin. But vitamin D deficiency can act as a biochemical saboteur—undermining mineralization even when the body is doing its best to compensate. The pain can be dull yet insistent, like a persistent drizzle that never fully dries.
Mood Changes and Cognitive Fog: When the Sunlight Narrative Goes Missing
Vitamin D is frequently associated with mood regulation and brain function. Deficiency can correlate with irritability, low mood, and a foggy, slow-thinking sensation. Overweight individuals may already face mood challenges related to stress, body image pressures, or inflammatory burden; vitamin D deficiency can add another layer of haze.
It’s not that every low mood is caused by vitamin D—but deficiency can tip the balance. Some individuals report reduced mental clarity and a diminished sense of emotional buoyancy. The mind may feel like it’s wading through warm syrup, where tasks take longer and decisions feel heavier.
Lower Immunity and Frequent “Small Defeats”
The immune system operates with rhythm and readiness. Vitamin D helps modulate immune responses, supporting a balanced defense. With deficiency, some people experience more frequent infections or prolonged recovery from colds and minor illnesses.
This doesn’t always look like severe disease. Sometimes it’s more subtle: lingering coughs, repeated bouts of fatigue after sickness, or a general sense that the body doesn’t “bounce back” as quickly. For overweight individuals, where metabolic inflammation may already be present, insufficient vitamin D can intensify vulnerability—like turning down the volume on protective mechanisms at the exact moment you need them loudest.
Weight-Related Complications That May Worsen Together
Vitamin D deficiency and overweight often travel in the same convoy. Low vitamin D has been associated with insulin resistance and metabolic disturbances in some studies, and deficiencies may complicate efforts to improve energy, exercise tolerance, and overall health.
While correlation is not identical to causation, the combined experience can be frustrating. A person may work diligently on lifestyle changes, yet fatigue, weakness, and mood shifts make consistency harder. The symptom suite becomes an obstacle course—one that feels unfair because it’s not solely driven by willpower.
A key insight: addressing vitamin D may be one lever among many. Still, when deficiency is present, correcting it can help restore traction to the body’s routines.
Hair Shedding and Skin Changes: Not Always Obvious, Often Misattributed
Some individuals notice increased hair shedding, changes in skin texture, or a generally “thinner” feeling to vitality. These symptoms can be misattributed to stress, nutrition, or hormones. Yet vitamin D deficiency can overlap with other skin and hair concerns through its role in cellular signaling and inflammation.
Overweight individuals—already navigating skin sensitivity, friction-related irritation, or metabolic inflammation—may notice skin changes more readily. The important nuance is that these signs are not diagnostic on their own. They are clues, like breadcrumbs that become meaningful when paired with other symptoms and lab results.
The Most Common Overlooked Clues: Pain, Low Stamina, and Slow Recovery
It’s easy to focus on one headline symptom and ignore the pattern. Vitamin D deficiency often shows up as a cluster: aches plus fatigue, reduced stamina plus mood shifts, infections that linger, and bones that feel like they complain more than they should.
Overweight individuals might assume their body is simply “more prone to discomfort” due to load. But the body can be dealing with both mechanical stress and biochemical deficiency simultaneously. When both forces converge, recovery becomes sluggish. A workout feels harder. Household tasks become heavier. Even sleep may not erase the residual ache.
How to Confirm and What Testing Usually Looks Like
The most reliable approach is medical assessment, usually including a blood test for 25-hydroxyvitamin D. Healthcare providers may also evaluate calcium, phosphate, parathyroid hormone, and sometimes markers of bone turnover depending on symptoms and risk factors.
Testing matters because vitamin D levels can vary widely. Some people may have deficiency with minimal symptoms; others may feel intense discomfort even with borderline results. Confirmation prevents guesswork, allowing a precise plan rather than a hopeful spray of supplements.
Supportive Habits: Sunlight, Diet, and Movement That Doesn’t Punish the Body
Vitamin D can be influenced by sunlight exposure, dietary intake, and supplementation when appropriate. Overweight individuals may benefit from strategies that improve absorption and circulation of health habits: consistent, gentle movement; nutrient-rich meals; and practical sunlight exposure when feasible and safe.
Nutrition sources may include fatty fish, fortified dairy or alternatives, egg yolk, and some mushrooms exposed to UV light. But diet alone can be insufficient for many people, particularly when sequestration in adipose tissue reduces bioavailability. That’s where healthcare-guided supplementation often becomes the missing piece of the puzzle.
Movement is also crucial. Strength training and weight-bearing exercise support bone and muscle health. The best plan is one that feels sustainable, not punitive. Consider it a choreography: gradual strength, steady balance, and endurance built one careful step at a time.
When Symptoms Require Prompt Attention
Seek timely medical advice if there is severe bone pain, frequent fractures, profound weakness, or persistent symptoms that are worsening. If numbness, significant muscle cramps, or marked changes in overall function appear, assessment becomes more urgent.
Vitamin D deficiency is common, but it shouldn’t be normalized. When the body’s signals grow louder—through escalating pain or declining ability to function—the storyline deserves a professional chapter.
The Intriguing Appeal of Addressing Deficiency Early
There is something hopeful in early recognition. Vitamin D deficiency can feel like living under perpetual shade, but correction can restore brightness—quietly, through improved stamina, steadier mood, reduced discomfort, and more confident movement. For overweight individuals, where multiple factors may be stacking together, addressing vitamin D can become a pivotal adjustment.
The goal is not perfection; it’s clarity. When you understand the body’s hidden bottlenecks, you can respond with precision rather than exhaustion. And sometimes, that precision feels like stepping from fog into daylight—one breath, one step, one day at a time.