Vitamin D is often discussed like a simple solution—take it, feel better, move on. Yet timing has a way of turning “simple” into “finicky.” Picture your body as a lighthouse keeper: the sun’s instructions arrive in cycles, and your metabolism—patient, particular—reads those signals with a clock-like precision. When you take vitamin D at the wrong time of day, you may still “get the vitamin,” but you can disturb the rhythm that helps your cells use it well. That timing error is small in appearance, but it can be loud in outcome.
The Body’s Circadian Orchestra: Why Morning and Night Matter
Your internal timetable is not a decorative concept; it’s an operating system. Hormone production, gene expression, and cellular repair all follow circadian cadence. Vitamin D is not merely a nutrient—it behaves like a prohormone that interacts with intracellular receptors, influencing downstream processes. When you ingest it, you create a surge of availability and metabolites that your body then attempts to integrate. If your timing clashes with your natural rhythms, that integration can become less efficient.
Morning routines often align with higher daytime physiological activity. Evening routines, especially late-night supplement habits, can coincide with reduced metabolic “throughput.” That doesn’t mean night is forbidden; it means the body prefers consistency. Think of vitamin D as a key you’re trying to insert into a lock. If the lock mechanism is sluggish—because your body is shifting into rest mode—the key may still fit, but turning it smoothly becomes harder.

Absorption Isn’t Universal: Food Pairing and Fat Content
Timing is only half the story; absorption is the bridge between the moment you take it and what your body can actually use. Vitamin D is fat-soluble. That means the small intestinal environment, bile flow, and meal composition influence how effectively it is absorbed. If you take a dose on an empty stomach—or at a time when your gastrointestinal activity is subdued—you can reduce the odds of efficient uptake.
So the “wrong time” can also mean the “wrong digestive context.” For example, a noon dose with a balanced meal often behaves more predictably than a late-evening dose without dietary fat. Imagine trying to light a candle with damp matches. The intent is good, but the conditions are inconvenient. The same nutrient can produce a dimmer effect when your absorption conditions are mismatched.
Practical nuance helps: pair vitamin D with a meal that contains some fat—eggs, yogurt, avocado, olive oil, or nuts. Even modest fat content can nudge absorption upward. If you’re unsure, observe your routine rather than chasing perfection. Consistency is a surprisingly strong ally.
Energy, Mood, and the “Delayed Ripple” Effect
Many people take vitamin D hoping for immediate benefits, but the body’s response can be slower than expected. Vitamin D participates in immune modulation and influences calcium homeostasis, both of which can affect energy perception and muscle function. Yet these outcomes are not instant fireworks. They are more like delayed ripples from a stone dropped into a pond—subtle at first, then gradually more visible.
If you take vitamin D late at night, you might interpret the next day’s energy changes incorrectly. Sleep quality, total caloric intake, and stress hormones can all blur the signal. What feels like “vitamin D didn’t work” might actually be “timing and context muddied the data.” Your body remembers schedules, not just doses.
Still, timing can matter for how you notice changes. Morning dosing may feel cleaner for tracking: you take it early, you eat normally, and you observe effects across the day. Evening dosing can confound observation, particularly if you also snack, drink caffeine, or shift bedtime patterns.
Night Dosing and Sleep: What Changes When You Take It After Dark
Vitamin D doesn’t typically act like a stimulant. However, the timing of any supplement can influence sleep indirectly. If nighttime dosing leads to reflux, unsettled digestion, or simply disrupts your pre-bed routine, the downstream effect on sleep architecture can be real. And because sleep governs metabolic hormones—cortisol, leptin, ghrelin—the entire “integration ecosystem” may shift.
Some people also report mood differences when they take certain supplements in the evening. The mechanism might involve indirect pathways: stress regulation, inflammation modulation, or simply the habit loop around taking pills. Even if vitamin D itself isn’t the direct cause, the timing can still become a variable that changes your day-to-night physiology.
If you prefer evening dosing, consider taking it earlier—during dinner rather than right before sleep. Let it ride the same tempo as your meal absorption window. Your bedtime should be a landing, not a negotiation.
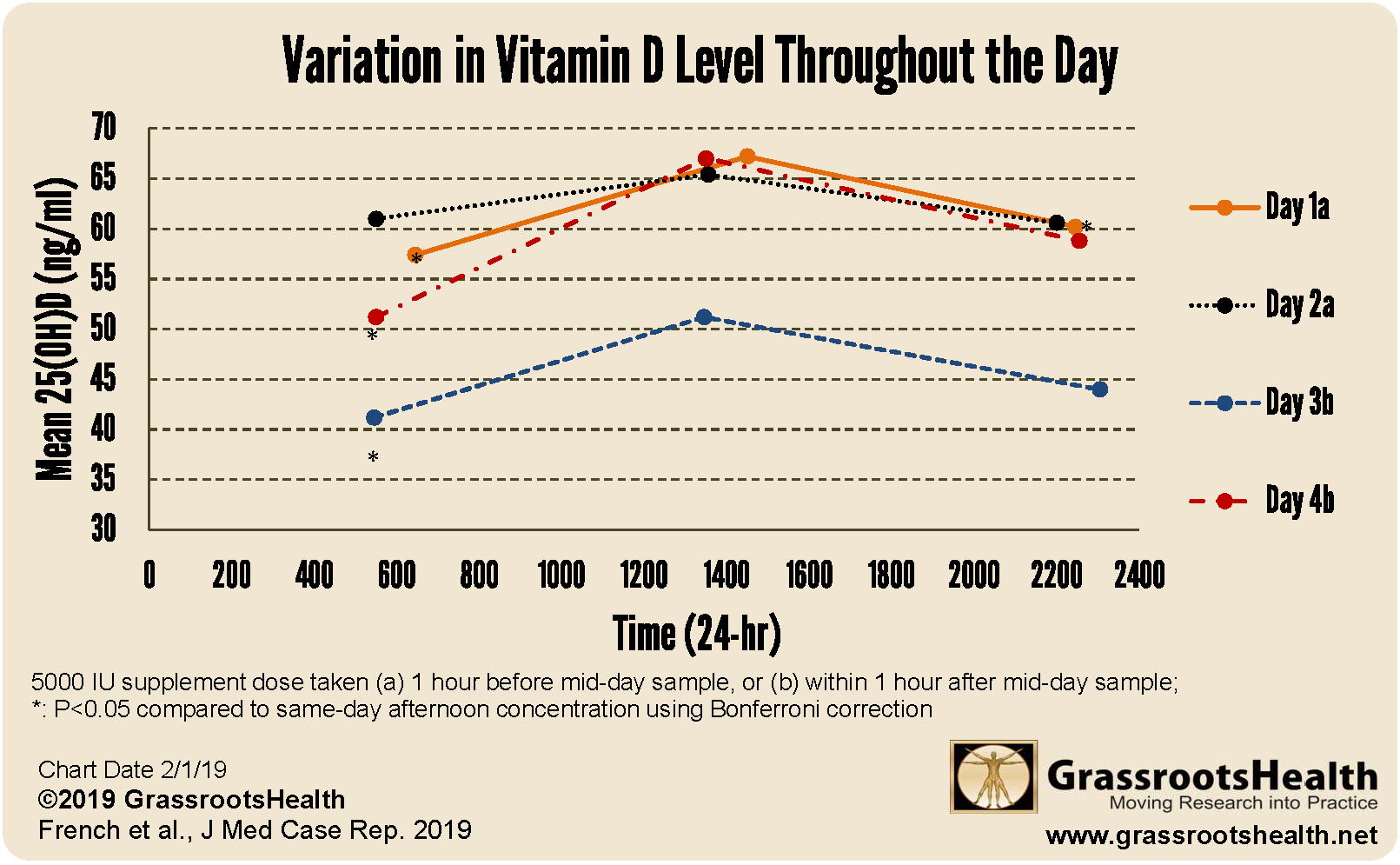
The Lab Reality: Levels Rise Gradually, Not Like a Stopwatch
Vitamin D status is measured by 25-hydroxyvitamin D (25(OH)D). This marker changes over time as intake, storage, and metabolism adjust. That means timing affects the efficiency of each dose, but the overall trend is still governed by weeks of consistency. Many people expect a quick jump and become discouraged when labs don’t move within days.
A common timing mistake is dose irregularity—taking vitamin D “whenever” or only during a period of feeling tired. Another is changing the schedule dramatically every few days. Your body’s vitamin D “banking system” operates with a preference for steadiness. Think of it like replenishing a reservoir. The height rises with repeated fills, not with one frantic splash.
Rechecking labs after an appropriate interval helps confirm whether your schedule, dose, and meal pairing are working together. Timing becomes less guesswork and more evidence-based rhythm.
Too Much Isn’t Just a Number: Accumulation and Overcorrection
Another reason timing errors matter is the temptation to correct too aggressively. People who feel nothing after a short time sometimes double doses or shift schedules, chasing a fast result. Vitamin D can accumulate because it’s stored in fat tissue and released gradually. If you take large amounts inconsistently—or increase the dose without guidance—you can overshoot.
Excess vitamin D can raise calcium levels and create symptoms that are easy to misattribute: fatigue, nausea, constipation, excessive thirst, or frequent urination. Some of these signs are broad enough to mimic other conditions, which makes overcorrection particularly risky.

Timing doesn’t prevent over-supplementation, but poor timing habits often accompany poor dosing habits. The remedy is not only “take it earlier,” but “take it thoughtfully.” Stick to the dose that aligns with your plan, and adjust only with data and guidance when appropriate.
A Simple Timing Strategy: Choose One Anchor and Keep It
The most elegant schedules are the ones you can maintain. Pick a daily anchor that matches absorption: a meal you reliably eat—breakfast, lunch, or dinner—and take vitamin D with that meal. Morning dosing works well for many people; midday also performs admirably. Evening can be fine if it’s paired with dinner rather than bedtime.
Consider setting a cue: a water bottle on the counter, a note near your coffee, or a pill organizer placed next to your usual food. Small behavioral scaffolding can outperform willpower. Your goal is to turn vitamin D timing from an intellectual exercise into an automatic ritual.
Finally, don’t forget interactions. Magnesium, vitamin K2, and overall dietary fat intake can influence how your body handles calcium and vitamin D-related pathways. If your routine is fragmented—supplement here, skipped tomorrow—your body receives mixed instructions.
When to Personalize: Lifestyle, Medications, and Medical Caution
Different lifestyles shift the optimal timing. Shift workers, people with irregular meal patterns, and those who struggle with late-night reflux may need a tailored approach. Some medications can also influence vitamin D metabolism or absorption. In these cases, “the right time” is the time that respects both your physiology and your treatment plan.
If you have kidney disease, high calcium, a history of kidney stones, or conditions that affect vitamin D handling, timing and dosing should be approached with extra caution. The goal isn’t experimentation. The goal is precision, steady monitoring, and safe targets.
Conclusion: Timing Is the Hidden Ingredient
Vitamin D doesn’t arrive like a single note. It becomes a chord—dose, absorption, meal context, circadian rhythm, and follow-up labs all blending into the final outcome. The timing error is not a dramatic mistake; it’s a subtle misalignment. Yet subtle misalignments have a way of accumulating, like dust in the corners of a familiar room.
Take vitamin D with a consistent meal, consider morning or midday for simpler tracking, and avoid treating the supplement like a short-term hack. When timing supports rhythm, the body can do what it does best: convert intention into function—quietly, reliably, and on schedule.